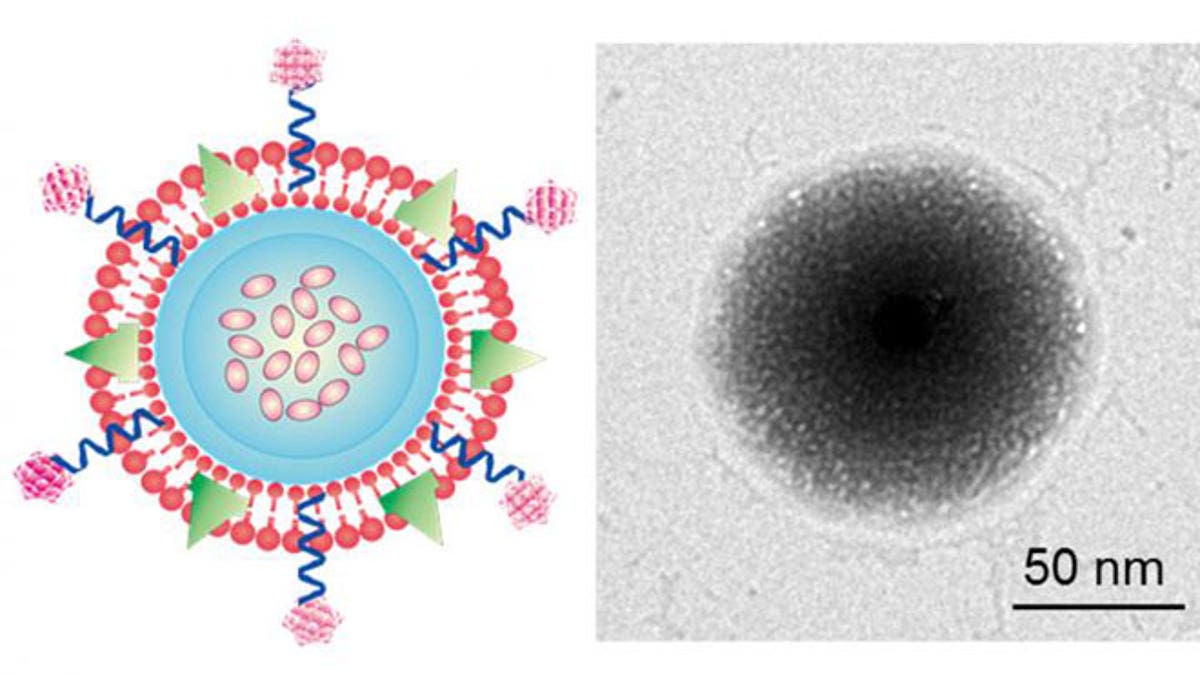
On the left is the schematic design of the TRAIL/Dox loaded platelet membrane-coated nanogel delivery system. The TRAIL is attached on the surface of membrane and Dox is loaded in the core of nanogel. On the right is a transmission electron microscope image of the drug delivery system. Black is the synthetic core nanogel, the outside shell is the platelet membrane. (Photo courtesy Quanyin Hu)
Coating anticancer drugs in membranes made from patients’ platelets may improve cancer treatment and help stop the disease from spreading, researchers in North Carolina have found.
"There are two key advantages to using platelet membranes to coat anticancer drugs," study author Zhen Gu, an assistant professor in the joint biomedical engineering program at North Carolina State University and the University of North Carolina at Chapel Hill, said in a news release. "First, the surface of cancer cells has an affinity for platelets— they stick to each other. Second, because the platelets come from the patient's own body, the drug carriers aren't identified as foreign objects, so [they] last longer in the bloodstream."
Lead study author Quanyin Hu, a PhD student in the joint biomedical engineering program, said that the combination results in the drugs attacking not only the main tumor site but also gravitating toward and attaching themselves to the other tumor cells circulating in the bloodstream, thus preventing the formation of new tumors.
During the process, which has been studied only in mice thus far, researchers draw blood from the patient, then draw platelets from the sample. They then place platelet membranes in a solution with a nanoscale gel consisting of the anticancer drug doxorubicin (Dox), which targets the nucleus of a cancer cell, according to the release. The solution is then compressed to form nanoscale spheres consisting of platelet membranes and Dox-gel cores. Researchers then coat the surfaces of the spheres with the anticancer drug TRAIL, the best medication to obliterate cancer cell membranes.
According to the news release, the mice study indicated that implementing Dox and TRAIL in the pseudo-platelet drug delivery method helped attack large tumors and circulating tumor cells better than using Dox and TRAIL in a nano-gel delivery system without the platelet membrane.
After being released into a patient’s bloodstream, the pseudo-platelets can travel for up to 30 hours, compared to only six hours that the nanoscale versions do without the coating.
Researchers said they plan to do more pre-clinical testing with the method.
“We think it could be used to deliver other drugs, such as those targeting cardiovascular disease, in which the platelet membrane could help us target relevant sites in the body,” Gu said in the release.








































