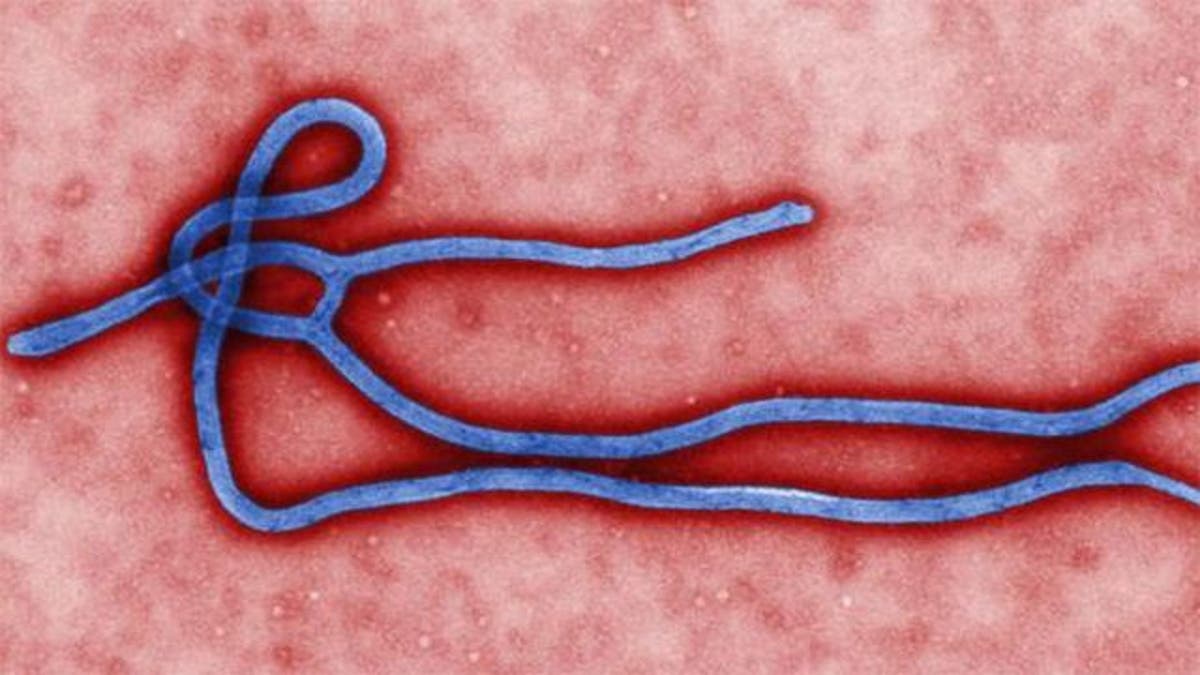
With the first Ebola patient diagnosed in the U.S. earlier this week, questions have been raised as to the preparedness of the country’s hospitals -- but infectious disease specialists say facilities are ready.
“There are measures that are recommended for Ebola that are also part of routine hospital measures that they use for other diseases that are more common, like tuberculosis, hepatitis, measles,” Dr. Jeffrey Duchin, chief of communicable disease epidemiology & immunization of public health in Seattle and King County, Washington, told FoxNews.com. “The precautions, facilities, processes and procedures are already routinely used for other diseases and monitored in that context.”
These measures are regulated by multiple organizations, including The Joint Commission, state governments, the Centers or Medicare & Medicaid Services, and the Healthcare Infection Control Practices Advisory Committee of the Centers for Disease Control and Prevention (CDC).
Dr. Amesh Adalja, infectious disease specialist at the University of Pittsburgh Medical Center, noted that efforts to monitor hospital-acquired infections, including MRSA, have been under high scrutiny lately.
“I think the general public may not be aware of all the effort hospitals do to prevent infection,” he told FoxNews.com. “Really, what we’re talking about [with Ebola] is a hospital-acquired infection,” he said.
Adalja, a member of the Infectious Disease Society of America's (IDSA) public health committee, cited past importations of diseases that have been managed, without the public awareness Ebola has drawn, such as Lassa fever and Marburg virus disease, a severe and highly fatal disease caused by a virus from the same family as the one that causes Ebola.
“If Lassa fever and Marburg can come in the U.S. and not have secondary infections in hospitals, it’s a good indicator of what Ebola will behave like in the U.S. as well,” he said.
In the case of an infectious disease, a patient may need to be isolated, or taken away from contact with others.
“To isolate, you need a single room that is closed off from access to other patients, preferably with an anteroom where gowns and gloves can be changed and thrown away,” Duchin, a professor of infectious diseases at the University of Washington, said.
The personal protective equipment required for infectious disease control starts with barrier precautions— gloves, gowns, face masks to prevent splashes and droplets and provide eye protection. With Ebola, if a patient has a lot of vomiting, diarrhea or bleeding, protective booties can be worn over shoes.
“All hospitals should be able to use a type of personal protective equipment, which is recommended for Ebola, but also used routinely for other common diseases, such as HIV, hepatitis, MRSA … all these common infections require similar measures,” Duchin said.
According to Duchin, most large hospitals have isolation rooms that also have negative pressure, which only draws air into the room. These are used for patients with airborne infections such as measles and tuberculosis. Ebola is not an airborne virus.
“A hospital may use respiratory protection — which is not recommended routinely by the WHO or CDC — as an extra precautionary measure because of the images [in the media],” Duchin said.
There is the possibility that Ebola could become airborne in a hospital setting if a patient undergoes a procedure which causes aerosolization, such as intubation, if they, for example, become critically ill and unable to breathe on their own. In this case, respiratory protection would be put in place to filter air.
“That’s the hoods and respirators that are being used because health care workers are concerned an Ebola patient may need to be put on respirator and as a precaution many elected to use respiratory protection right away … even though it’s not necessarily recommended,” Duchin said.
There have been no incidences where an Ebola patient in the U.S. needed to be intubated or undergo an aerosol generating procedure, Dr. Ryan Fagan, medical epidemiologist and lead of U.S. infection control for the Ebola response, told FoxNews.com.
“In all the outbreaks that have happened previously, there’s never been evidence that Ebola ever spread by an airborne route from human to human,” he said.
As for smaller hospitals, while there may be some disparities in health care, experts agree that all should be capable of handling a possible Ebola patient. Many are part of health care coalitions of multiple local hospitals — a development that came in the wake of September 11, and the anthrax scare, for hospitals to be better equipped to deal with hazards, Adalja said.
“A small hospital may be resource-strapped and may not be able to take care of the patient there, but you have to remember those hospitals are usually very good at triaging patients and deciding how they have to be taken care of — they do that for heart attacks … [the hospital] will move patients if needed if the resources are outstreteched,” Adalja said.
Smaller hospitals may not feel prepared for a possible Ebola patient because of lack of familiarity with infectious control cases, likely not because they had inadequate facilities or lack of understanding, Duchin noted.
“If hospitals don’t see a certain type of patient… they may not have familiarity … don’t feel comfortable in that sense,” he said.
Ebola virus disease is a severe, often fatal hemorraghic disease, that is transmitted from human-to-human by direct contact with the blood, saliva mucus or other bodily fluids of an infected person who is showing active symptoms, which can include the sudden onset of fever, muscle pain, headache and sore throat. Humans are not considered infectious until the onset of symptoms.
Experts noted that Ebola is not easily spread between people.
“Ebola is less contagious than a cold. There’s a lot of confusion because there are deadly infectious diseases and deadly infectious contagious diseases but [Ebola] is not very contagious, which is how we’re able to say with confidence that it is not something that will spread in the U.S.,” Adalja said. “[Ebola] is not going to find the U.S. to be a conducive environment for spread because of the way we operate our hospitals, the way we do burial practices … [spread of Ebola] is not applicable to the U.S.”







































