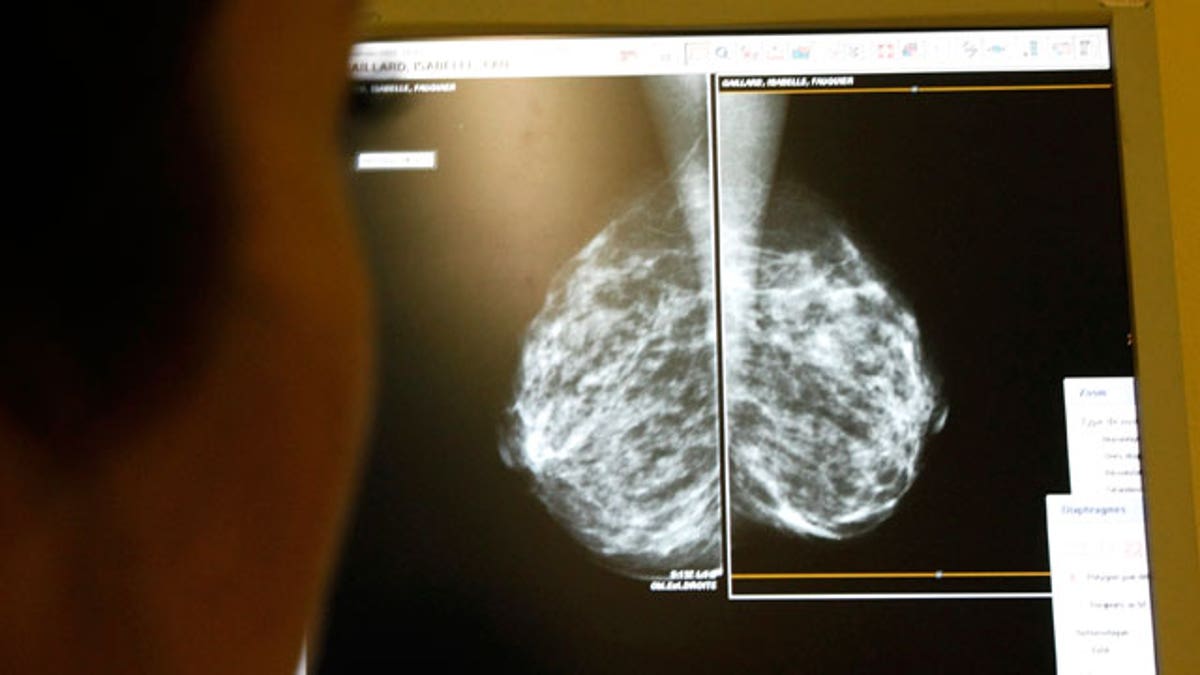
One in four women who have breast-conserving surgery for cancer need a second operation to remove more breast tissue, suggests a new study that also found the rate of re-operation varied widely by surgeon.
Researchers said the goal shouldn't be to never conduct a repeat surgery, which might cause surgeons to take out too much tissue the first time around, or to avoid operating again on women who need it.
Still, very high rates of re-operation mean some of those surgeries might be unnecessary, or could be prevented.
"I don't think it's so great to put a patient through an operation and 30 to 40 percent of the time to say, 'Hey, guess what, we have to do this again.' I just think that's too high," said Dr. Laurence McCahill, from the Lacks Cancer Center at Saint Mary's Health Care in Grand Rapids, Michigan, who worked on the study.
"For many reasons, (a second surgery) is very hard on patients," he said. "It's hard on patients from a psychological standpoint, from a physical standpoint and from an economical standpoint as well."
Breast-conserving surgery, also called partial mastectomy or lumpectomy, on average costs between $6,000 and $7,000, according to the Healthcare Blue Book.
McCahill's team studied about 2,200 women getting a first breast-conserving surgery at four different research sites in the United States between 2003 and 2008.
In that procedure -- a typical initial breast cancer treatment along with radiation -- the surgeon tries to remove just the cancerous cells and a few healthy ones around them to keep the breast as intact as possible.
Dr. Rachel Wellner, director of breast services at NYEE, Continuum Cancer Center in New York City, said it is important to note that this study excluded women who had multi-focal disease – cancer in more than one quadrant of the breast.
"McCahill's study population were found to have, on average, about 1.5 centimeters of cancer. These data points cannot be extrapolated to patients with multi-focal disease,” Wellner said. “We know breast conservation is safe and generally the recommended standard in this type of patient population. However, if our long term goal as a medical community is to minimize re-excision rates, we should aim for consensus as to what constitutes a safe negative margin.”
In 23 percent of the study cases, surgeons decided from lab reports that they didn't take out enough cells in the first operation, and went back in to remove more tissue. Between eight and nine percent of all women initially getting breast-conserving surgery ended up later having a total mastectomy.
McCahill and his colleagues didn't know what went into each surgeon's decision to do a second surgery on a particular woman, and they couldn't tell whether those re-operations, or re-excisions, reduced the risk of the cancer coming back.
But they did find that the rate of re-operations varied greatly between doctors. Individual surgeons performed a second procedure on anywhere from none to 70 percent of their patients, the researchers reported Tuesday in the Journal of the American Medical Association.
Dr. Kathie-Ann Joseph, assistant professor of surgery at NYU Langone Medical Center in New York, said many women opt for a lumpectomy upon hearing a cancer diagnosis because they want to save their breasts.
"There are a significant amount of women who are comfortable choosing a mastectomy," Joseph said. "But the goal has always been – as we have moved forward with surgical options - that we do the least invasive option."
Joseph said it used to be standard to remove the whole breast and all the surrounding tissue, now many doctors, like herself, prefer to remove just the cancer and preserve the breast.
"We were as concerned with the zero percent re-excision rate," McCahill said, as that might mean doctors were removing too much tissue on the first surgery or weren't operating again when they left cancer cells behind.
That's why it probably wouldn't be a good idea to measure or reward surgeons based on how low their rates of re-operation are, he said. Instead, McCahill suggested doctors working together and with their patients to get that rate down to somewhere between one out of every 20 and one out of every five women needing re-excision.
Joseph, who was not involved in the study, said surgeons can't always avoid re-operation because some cancer cells are too difficult to spot or feel on a first surgery.
"When you compare a lumpectomy to a mastectomy, yes, you have a higher rate of recurrence, but there's no difference in survival," Joseph added. "That's why we do a lumpectomy."
Joseph said these microscopic cells are undetectable on mammograms or ultrasounds, and that’s when surgeons start talking about mastectomies.
"I don’t think the answer is to tell patients they automatically need a mastectomy," Joseph said. "Women who are reading this article – and this new study – that’s not what they should take from this. Discuss with your surgeon what you are comfortable with. It’s not an exact science.”
Wellner said the study raises an important point: Surgeons in the breast care community should come up with a consensus on what constitutes a safe margin, and maybe find better detection of margins at first operation in order to avoid a second or third surgery – or even a mastectomy.
FoxNews.com's Jessica Ryen Doyle and Reuters contributed to this article.







































