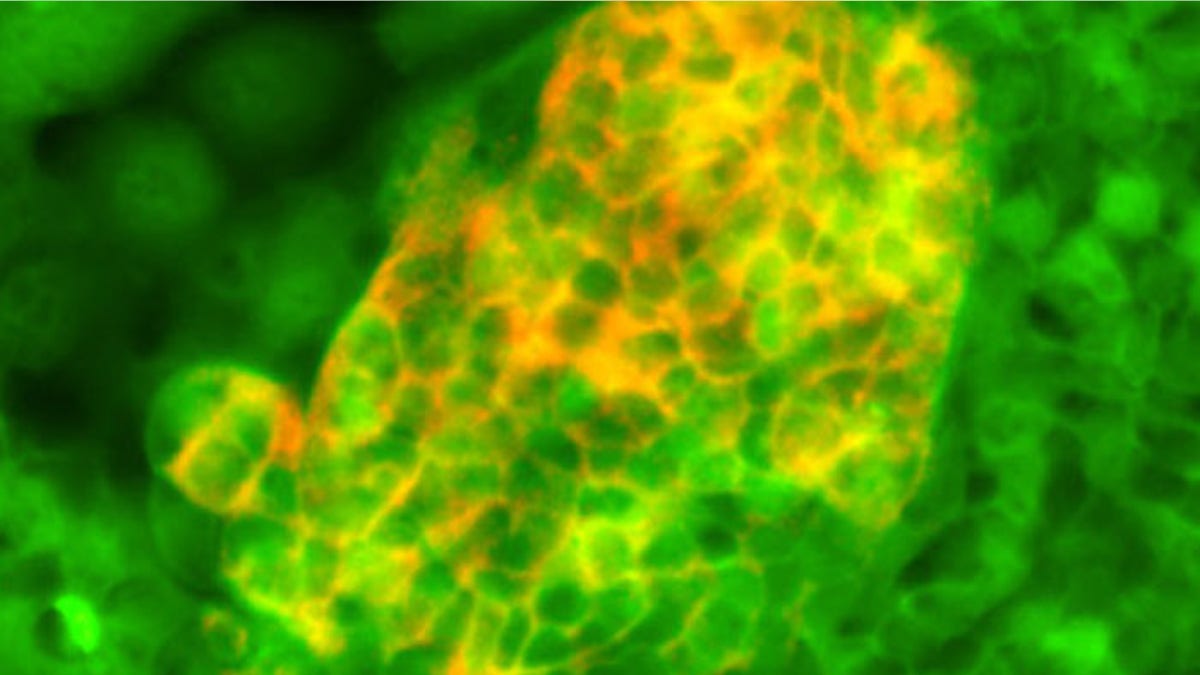
Foregut stem cells (green) differentiated into pancreatic cells expressing insulin. (Dr. Nicholas Hannan)
Researchers from the University of Cambridge have developed a new technique for creating stem cells of the human liver and pancreas – a breakthrough that could significantly transform the future of transplant therapies.
The novel method involves altering the signal pathways of cells specific to the human foregut – the upper portion of the gastrointestinal (GI) tract. Through this manipulation, researchers were able to stop the cells from developing fully and push them into a state of constant self-renewal.
As a result, these “foregut stem cells” can then be further amplified by physicians, who can then form them into liver or pancreatic cells. These cells could potentially be used to treat damaged organs or tissue, in addition to conditions such as type 1 diabetes or metabolic liver disease.
According to the researchers, their technique improves upon existing methods for creating liver or pancreatic stem cells, which sometimes do not yield enough cells for transplantation.
“We had identified that problem going forward: There is no process to amplify a population of cells that can be used for transplant therapy,” lead author Dr. Nicholas Hannan, from the University of Cambridge Wellcome Trust MRC Stem Cell Institute, told FoxNews.com. “We thought if we could develop a technique that would allow us to capture the progenitive population of cells, this would be the perfect cell type you would want to expand and have at the ready to differentiate into liver and pancreatic cells.”
Currently, most stem cells begin as human pluripotent stem cells (hPSCs). These types of stem cells sit at the top of the hierarchy for differentiation, as they have the potential to transform into any one of the three primary embryonic layers of human cells – the mesoderm, the ectoderm or the endoderm. Since these kinds of stem cells are also self-renewing, they provide physicians with a potentially infinite source of viable cells for regeneration.
However, differentiating hPSCs into liver and pancreatic cells can be tricky. To create these kinds of cells, hPSCs must be differentiated solely into the endoderm layer – the tissue primarily associated with organs of the digestive and respiratory system.
But since hPSCs have a lot of variability in terms of how they are derived and the kinds of cells they can become, cell cultures intended to create pancreatic or liver cells are often “contaminated” with the wrong cell types, rendering the precursor population unusable for further differentiation.
To address this problem, the researchers studied the conditions under which cells differentiate specifically into the human foregut. Hannan explained that at some point during development, all cells eventually move through the foregut state – when they are just part of the endoderm layer.
“As we do develop organs, we have to naturally move through the foregut state,” Hannan said. “Everyone develops a foregut during development, and most of the techniques that produce cells actually transition through the foregut state, but isolating it is difficult. Our natural tendency is to move down the developmental program.”
Hannan and his team discovered that in order to restrict these cells to the foregut state, a specific set of genes in the cells needed to be expressed. When they developed their stem cell populations under these conditions, the non-endodermal cells eventually stopped growing while the endodermal cells flourished.
“We’ve basically taken pluripotent cells and induce them into the endoderm,” Hannan explained. “So these foregut cells can’t make mesoderm or ectoderm. They’re restricted solely to the endoderm layer.”
The result of this gene manipulation was a “purer” population of human foregut stem cells (hFSCs), able to self-renew and differentiate into any cell in the human foregut. The researchers also found that transplanting these cells did not form any tumors, making them a safe choice for physicians and patients.
According to Hannan, these cells have the potential to aid a variety of patients – such as those suffering from type 1 diabetes, individuals with inherited metabolic problems of the liver, and even patients who require a liver or pancreas transplantation.
“What we have now is a progenitive pool of cells that can make any cell type in the foregut,” Hannan said. “Literally, the millions and millions of cells required (for transplantation) are difficult to amplify without the culture system we’ve developed.”
The research was published in the journal Stem Cell Reports.







































