When will people with Social Security receive stimulus payments?
David Asman explains when stimulus payments will reach Social Security recipients
Get all the latest news on coronavirus and more delivered daily to your inbox. Sign up here.
Over the past decade, the U.S. government spent nearly $100 billion on preparation for major health crises including pandemics, according to a 2018 paper on such funding -- though the coronavirus outbreak still had Washington and states across the country scrambling to muster supplies and respond when it hit.
Numbers from a paper in the academic journal "Health Security" released in late 2018 indicate that the government spent between $10 billion and $12 billion each year from 2010 to 2018 across several agencies on programs that contribute to "biosecurity," the management of "pandemic influenza and emerging infectious diseases," and "multiple-hazard and general preparedness" programs that assist in readiness for and response to different types of health threats, including diseases like the coronavirus.
COVID-19 seems to be the kind of problem the U.S. was preparing for, but a debate has raged in Washington over whether the money was spent effectively.
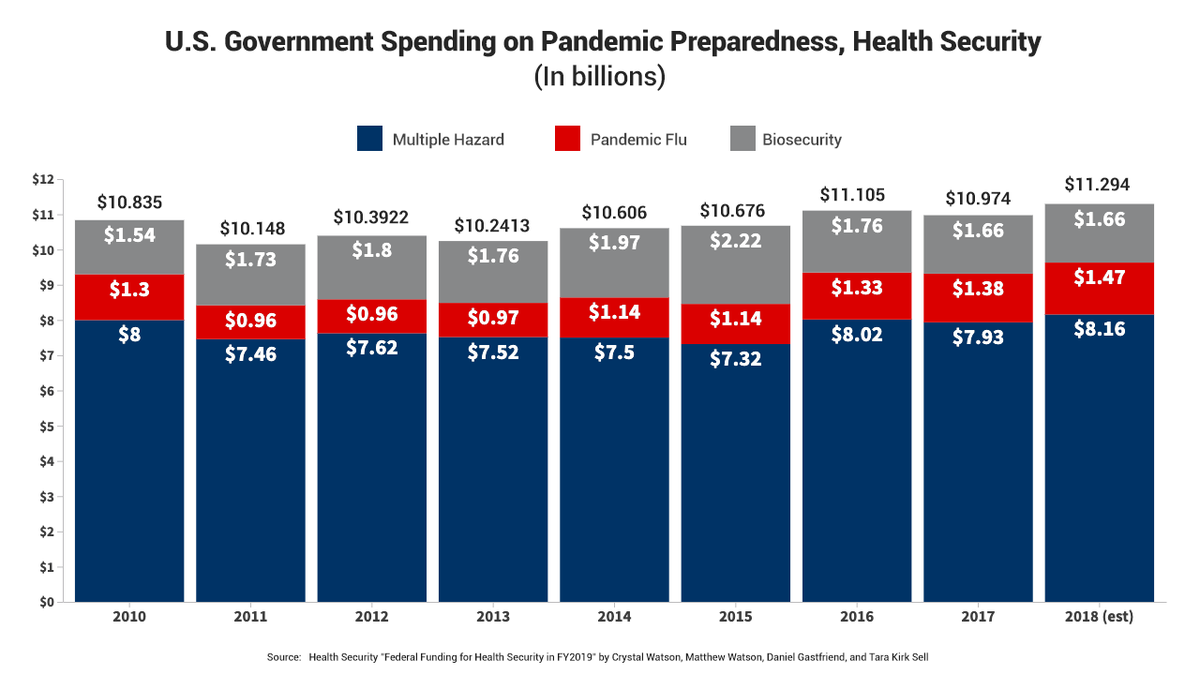
A breakdown of federal government spending aimed at preparing for health crises. (Data: "Federal Funding for Health Security in FY2019," Health Security)
TRUMP SET TO PRESIDE OVER RECORD SPENDING, DEFICITS AS CORONAVIRUS COSTS EXPLODE
"Ventilators, which were few & in bad shape, are now being ... produced in the thousands, and we have many to spare," President Trump said in a Wednesday tweet thread, alluding to how the U.S. did not have the resources it needed at the outset of the pandemic. "We are helping other countries which are desperate for them. Likewise, after having been left little, we are now doing more testing than all other countries combined, and with superior tests. Face masks & shields ... gloves, gowns, etc. are now plentiful."
Democrats have countered that GOP-driven budget cuts early in the decade squeezed areas like the stockpile of personal protective equipment (PPE).
Trump was also faulted for initially downplaying the coronavirus threat, as did many in the media and some Democrats like New York Mayor Bill de Blasio. But even when state and federal responses kicked into full gear they struggled to get medical supplies like ventilators and PPE to front-line health care workers. Additionally, federal and state governments are still working to secure enough coronavirus tests to open their economies, with some reaching out to other countries -- in Maryland's case, South Korea.
The White House coronavirus task force said last week it is working to expedite the production of a coronavirus vaccine, but it is still unclear when such a vaccine could become available, with some estimates placing the timeline at about 18 months despite prior plans that aimed for a faster timetable -- at least for unknown flu strains. The Strategic National Stockpile has only helped on the margins, and the Trump administration has had mixed success, at best, in using the Defense Production Act to get domestic industries to produce ventilators, testing swabs and PPE.
TREASURY TO BORROW $3T FOR CORONAVIRUS RELIEF, ADDING MORE DEBT IN 1 QUARTER THAN ALL OF 2019
"Our country is unable to meet an immediate need for critical medical supplies and personal protective equipment in the face of a crisis," Scott Paul, the president of the Alliance for American Manufacturing, said in a New York Times op-ed. "The absence of adequate domestic production capacity for things like face shields and respirators, coupled with the frailty of on-demand global supply chains and our utter reliance on them — for everything from the ingredients in our medications to parts of breathing machines — has left us dangerously exposed during an international health emergency."
The slow coronavirus response from all levels of government, particularly the federal government, came despite significant funding over the past decade for programs across multiple agencies, including the Defense Advanced Research Projects Agency (DARPA) under the Department of Defense (DOD); the Centers for Disease Control and Prevention's Emerging and Zoonotic Infectious Disease Programs under the Department of Health and Human Services (HHS); the National Institutes of Health (NIH) Biodefense and Emerging Infectious Disease research program, also under HHS; and others.
The "Health Security" paper, titled "Federal Funding for Health Security in FY2019," also recorded government spending in preparation for nuclear and chemical threats, which Fox News has excluded from this analysis. It also analyzes the president's 2019 budget, data which is excluded as well because presidential budgets do not reflect actual or estimated spending.
The government's struggles dealing with increased hospitalizations and demand on medical equipment were largely cited as reasons why widespread economic shutdowns were needed, as government officials and health experts stressed the need to "flatten the curve" of coronavirus infections in the United States. The resulting economic hardships forced Congress to take drastic measures to prop up the economy and Americans' everyday finances, including the $2.2 trillion CARES Act, which is ballooning the federal deficit to a projected $3.7 trillion for 2020, according to the Congressional Budget Office, with three other coronavirus spending bills already passed and another, potentially $1 trillion-plus, piece of legislation being considered.
COUNTIES DEFYING STATE CORONAVIRUS 'STAY-AT-HOME' ORDERS AND REOPENING FOR BUSINESS
Penn State Assistant Professor of Public Policy Simon Haeder, who specializes in health policy, noted some of the shortfalls -- and highlights -- in U.S. preparation for the coronavirus.
Haeder specifically complimented the many highly trained and educated workers -- largely because of programs run by the Centers for Disease Control and Prevention (CDC) -- available in the U.S. to plan responses, strong research capabilities at American universities and creative members of the private sector willing to respond to the public health crisis.
"I think we had good infrastructure in place, or we had people thinking about this, the CDC has good training programs, I think that was one of the benefits we had," he said. "The CDC has a special training program that trains people and puts them back into the community as doctors, researchers and those kinds of things that are supposed to spot developments on the ground as they happen, and I think we are ahead of a lot of other countries when it comes to that."
Underscoring Haeder's point, the Global Health Security Index, which is put together by the Nuclear Threat Initiative -- an organization that works on both nuclear security and biosecurity -- ranked the U.S. as the most prepared of 195 countries ranked to deal with threats to its health security.
But, he said, as states begin to reopen their economies, the U.S. is not in a much better place than it was at the outset of the pandemic.
"A month ago or two months ago we didn't have a solution to the virus. We don't have any treatment that really works and we don't have any way to vaccinate people," Haeder said. "Now we were able to withstand the initial onslaught of what was coming, but ... the same problem exists today. We don't have any treatment, and we don't have any vaccine. And the only thing we've done is we've not overwhelmed, in most places ... the health care system yet," by flattening the coronavirus curve with economic shutdowns.
It's a common misconception that business closures and stay-at-home orders aimed at "flattening the curve" are meant to reduce the total number of people who will fall ill because of the coronavirus. Rather, these curve-flattening measures are meant largely to reduce the number of people who are sick at any given time, thus avoiding a surge in cases that overwhelms the health care system and causes otherwise preventable deaths because not all patients are able to access lifesaving critical care.

FILE - This April 23, 2020, file photo shows President Donald J. Trump's name printed on a stimulus check issued by the IRS to help combat the adverse economic effects of the new coronavirus outbreak in San Antonio. (AP Photo/Eric Gay, File)
TREASURY TO BORROW $3T FOR CORONAVIRUS RELIEF, ADDING MORE DEBT IN 1 QUARTER THAN ALL OF 2019
Outside of a few hotspots, the U.S. has largely accomplished the goal. Most hospitals are not overwhelmed and the death rate from the coronavirus in the U.S. is either in line with or lower than that of other countries. But that has come with the drastic economic costs stemming from the large-scale shutdowns that made it possible.
According to Haeder, despite what the government spent in the past decade to deal with health threats, it neglected to ensure there was a supply of medical means to keep the coronavirus from upending daily life in the way it has.
"We could keep more things open longer if our capacity to respond to this would have been higher," Haeder said. "For sure, the curve that you're able to sustain medically is a lot higher if you're prepared."
Achieving that capacity, Haeder said, would mean more concerted efforts to store things like ventilators and N95 masks, moving the production of many medical products back to the U.S. from India and China, and ensuring that U.S. industry has the ability to quickly ramp up the production of essential items when called upon.

The headquarters for Centers for Disease Control and Prevention in Atlanta, Georgia. (AP Photo/ Ron Harris)
ALARM BELLS SOUND OVER HISTORIC DEFICIT SPENDING, AS CORONAVIRUS BILLS COULD NEAR $5T
Those measures, of course, would cost even more money. But Haeder says they would be worth it considering the United States' yearly health preparedness expenditures are dwarfed by the economic costs of responding to the crisis -- the CARES Act alone outsizes the government's yearly spending on health preparedness by a factor of about 200.
"We're hit with two things right now," he said. "We're hit with the fallout from the medical issue of dealing with the virus, but it's made much, much worse from the economic side because the economic side will be with us for a very long time. There's a massive dip in income, lots of people lost their jobs. Lots of them will have lost their jobs permanently ... the debt has massively increased, and we could have dealt with a lot of that off-hand if we would have been better prepared."
The kind of efforts that would have allowed the U.S. to remain largely open, or at least more than it has, would be expensive, Haeder said. But he said "no" and laughed at the suggestion that their cost could approach $2.2 trillion.
"While I can't give you any numbers, I think you can make a sound case that spending just a little bit of money upfront is gonna be a really, really good investment," Haeder said, mentioning that there are ways, like rotating stocked-up supplies and selling them before they expire, to cut costs.
Haeder also suggested that a lack of planning and organization on how governments and institutions coordinate their responses contributed to the severity of the pandemic in the U.S.
"When people got on Jared [Kushner]'s good side, they were able to get stuff. And, you know, when they could explain that they really needed it. I don't think that's a good way to handle a nationwide catastrophe, but I think we really need to think about how we put those lines of communication and lines of resources in place from a government-to-government perspective," Haeder said.
MCCONNELL, SCHUMER SPAR OVER HEALTH OF LAWMAKERS AS SENATE CONVENES FOR FIRST TIME IN WEEKS
Such measures, involving more planning than spending money on tangible things, would also be a lot cheaper than economic stimulus after the fact. Trump critics often note that the Obama administration created a pandemic playbook and a council to prepare for and coordinate pandemic responses. The Trump administration eliminated the council and merged its responsibilities with other bodies during a reorganization of the National Security Council, and it did not use the playbook.
Of course, there is rarely much appetite from lawmakers to funnel any amount of taxpayer money into preparing for invisible, undefined threats that may appear sometime in the future. There are other issues more palatable to voters -- like tax cuts, entitlement programs or infrastructure.
Calls for increased health preparedness for future health crises have emerged in the wake of recent ones -- there are already people using the phrase "never again" about the coronavirus -- but if the current pandemic follows the same pattern as past health scares, those calls may die down eventually.
An example of this phenomenon can be found in New York City, which in 2006 under former Mayor Michael Bloomberg moved forward with an aggressive plan to prepare for a pandemic similar to the coronavirus.
But, in a story first reported by ProPublica, the city never purchased even half of the ventilators that it planned to. And those it did buy were eventually auctioned off because of the costs of maintaining and storing them, and the company that manufactured the ventilators stopped making the model the city bought.
CLICK HERE TO GET THE FOX NEWS APP
The city also stocked up on N95 masks, but, the city's health department told ProPublica, they "all expired, and it became cost-prohibitive to replace them in any meaningful quantity."
Despite the costs and challenges, Haeder said, improving stockpiles of medical equipment and government planning would be a good investment for the next time a coronavirus-level pandemic hits.
"The argument that I'm making is if you're prepared, then your measures to deal with this don't have to be so draconian and ... we would have been able to keep more stuff open longer, and keep interaction to a degree up longer, and keep businesses open."













































