Rhode Island State Seal
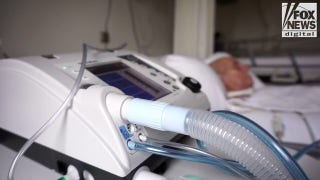
CRANSTON, R.I. — As the country reckons with an unfolding opioid crisis, and officials from both parties talk about improving access to care, jails and prisons remain treatment deserts. Few facilities provide any addiction treatment, and when prisoners are released, they return to the same environments — and the same triggers — that fostered their addiction in the first place.
Here, at its campus of squat brick buildings, the Rhode Island Department of Corrections is trying something different. Over the past year, it has expanded its so-called medication-assisted treatment program, becoming the first state system to offer such a broad range of therapies — including all three drugs approved to treat addiction — to its entire prison population.
For supporters, there’s a simple argument behind the initiative: Medication-assisted treatment, or MAT, is considered the most effective therapy for opioid addiction, and so providing it is the right thing to do from a public health perspective. And if it can help reduce recidivism, it’s the right thing to do from a criminal justice perspective.
“It is standard of care in the community, so I think eventually it will become standard of care in correctional facilities,” said Dr. Jennifer Clarke, the medical programs director for the corrections department.
MAT consists of three therapies. Two, methadone and buprenorphine (often referred to as Suboxone), are opioids that help stave off withdrawal symptoms and reduce cravings, while the third, Vivitrol, is an “antagonist,” meaning it blocks people from getting high if they use drugs.
John Young, a 27-year-old inmate here, said his daily dose of methadone has saved him from the worst of withdrawal’s effects. He began treatment four months ago at the start of a six-month sentence for a probation violation tied to a drug-related charge, and it’s provided him with a level of stability.
Young said he plans to maintain his methadone regimen after he’s released.
“It’ll keep me safe — you don’t have to take the risk of getting out there and trying to find heroin or using needles,” he said. Without methadone, “as soon as I got out, I’d probably want to get high.”
“I want a good job, I want to succeed, I want to be better for my family,” he added. “I want actual things to be proud of.”
An estimated half to two-thirds of all prisoners have some form of substance abuse disorder. Doctors say there’s a public misconception that incarceration, particularly years-long incarceration, can help prisoners break an addiction.
But abstinence does not in and of itself treat substance use disorder. And upon release, prisoners generally have a reduced tolerance for opioids; one study found that within two weeks of being released, former inmates overdose at rates nearly 130 times as high as the general population.
But researchers studying Rhode Island inmates have found that prisoners who take methadone before their release are more likely to continue their treatment. If they do that, the hope goes, they will be less likely to overdose or to commit crimes.
“We cannot afford to keep getting all these people with opioid use disorders coming into these publicly funded institutions and not get treated, because it only fans the flames of this crisis as they are released,” said Dr. Josiah Rich, a Brown University researcher who is assessing Rhode Island’s MAT program.
Other states have started to look to Rhode Island to learn from its MAT program, and the Obama administration highlighted it as a national model.
This week, the White House’s commission on combating the national opioid epidemic released an interim report recommending that the Justice Department increase MAT in prisons. The panel noted that multiple studies have shown that inmates who received treatment had lower recidivism rates than those who did not.
But there are challenges to replicating Rhode Island’s system, and the corrections system here enjoys some advantages.
It had political support for the effort, with the state government approving $2 million annually for MAT in prisons. And the corrections system is compact: Rhode Island does not have county jails. All inmates are brought to one center here, and the state’s prisons are all on the same campus.
“If we start someone on MAT in jail, we’re not worried about them getting sent upstate to prison,” Clarke said. “They’ll go across the street, and they continue or we can take them off slowly.”
Read more: How effective is medication-assisted treatment for addiction? Here’s the science
Clarke has worked in the corrections department for 20 years, and she’s been advocating to expand MAT for just as long. But until last year, only people already on methadone when they were incarcerated could get a week’s worth of treatment (except for pregnant women, who have always remained on treatment).
Now, inmates are screened when they arrive, and those with opioid use disorders are given the option of treatment. Inmates can take methadone or buprenorphine for up to a year, and restart treatment before they are released. Vivitrol is given a month or two before release. The program also includes counseling.
The treatment is provided by CODAC Behavioral Healthcare, a nonprofit with clinics around the state, and the idea is that inmates will transition to one of those clinics when they are released to continue their care.
Some law enforcement authorities have embraced Vivitrol because it is not an opioid, a message touted by its manufacturer, Alkermes, as it has lobbied lawmakers and drug courts. Other experts have questioned the data supporting Vivitrol and noted that there is more rigorous evidence supporting the use of methadone and buprenorphine. (Data from the first study to compare Vivitrol and Suboxone are expected this year.)
But for Clarke, what matters most is that inmates find a treatment they will stick with. Giving prisoners Vivitrol, for example, is useless if they don’t show up for another dose when released.
“Vivitrol is a great medication, for the right patient,” she said. “Really, the best treatment is the treatment that the patient will engage in.”
Experts said they see hints that MAT is becoming more accepted.
“There are all these ways to bash the treatment, but none of that is based on an argument about the effectiveness of the data,” said Dr. Joshua D. Lee, an associate professor at New York University School of Medicine. “In general, attitudes are certainly shifting in favor of finding solutions.”
Still, there is always concern that buprenorphine and methadone will be diverted and used illicitly. While the medications typically cannot give users a heroin-like high, they can generate a buzz. Some illicit use may also stem from inmates seeking out the medications to assuage their withdrawal symptoms, experts say, meaning the treatments are, in a way, being used for their approved purpose.
“So it’s hard, right?” said Dr. Warren Ferguson, an expert in criminal justice and health at the University of Massachusetts Medical School, who is studying MAT in New England jails and prisons. “If the primary mission of a correctional facility is safety and security, and health care is secondary to that, if you look at it through that lens, you can understand why correctional facilities are enthusiastic about antagonists” like Vivitrol.
But, Ferguson said, evidence shows that treatment with methadone and buprenorphine improves outcomes in communities. Now, researchers are trying to replicate that in jails and prisons.
“What are some of the facilitators and barriers to establishing those programs?” Ferguson said. “What are some of the adaptations that need to be made for that to be successful?”