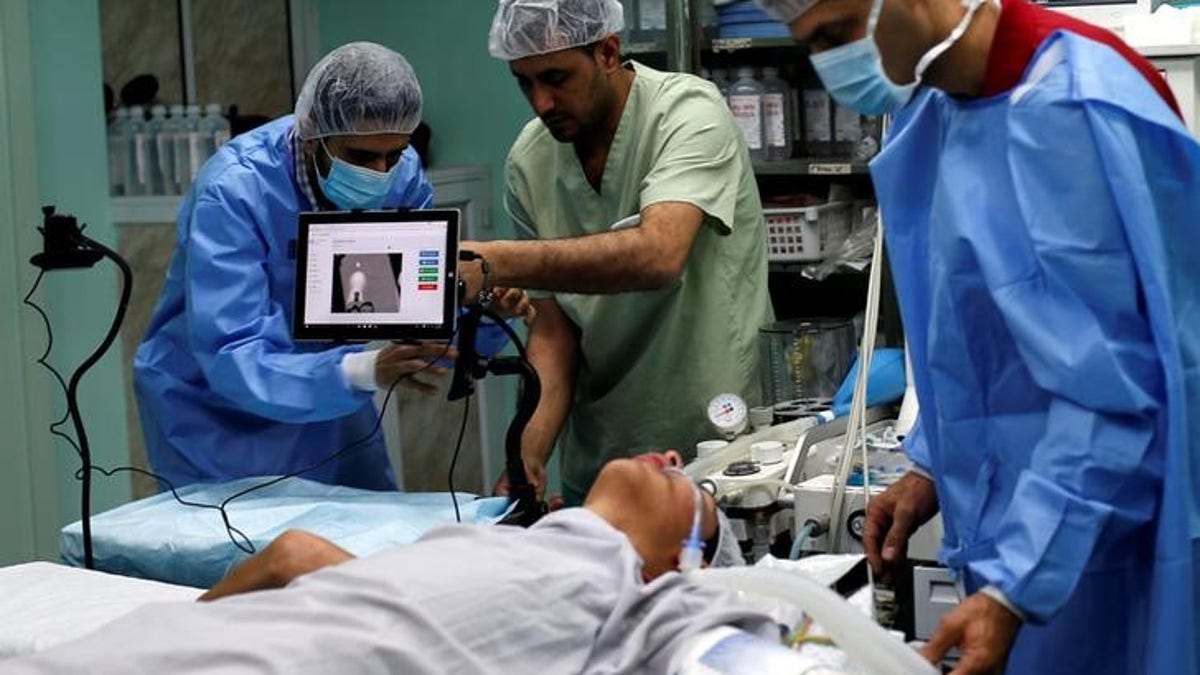
A patient lies on a bed as a technician adjusts a screen before the start of a Proximie surgery, with doctor Ghassan Abu Sitta in Beirut guiding Palestinian surgeon Hafez Abu Khousa in the operating room at Al Awda Hospital in the northern Gaza Strip (Copyright Reuters 2016)
How many people survive after emergency surgery is one measure of the quality of care they have access to, and post-surgery death rates in low- and middle-income countries suggest quality needs to be better, researchers say.
Using mortality rates within 24 hours and 30 days after emergency abdominal surgery as a measure, the study covered 58 countries and found risk of death was three times higher in low-income compared to high-income nations.
"Safety practices at the time of surgery are now embedded in high-income settings, which have the resources to plan and deliver them," said study coauthor Dr. Aneel Bhangu, from the University of Birmingham in the U.K.
"They are less routinely used in low and middle income countries, due to a lack of resources and training in safety cultures," which may include equipment sterility, availability of antibiotics, and type of skin preparation used at the time of surgery, he told Reuters Health by email.
"Around the time of surgery, lack of critical care facilities and imaging due to resources may also affect outcome adversely," Bhangu said.
For the study, 357 medical centers reported data on more than 10,000 patients receiving emergency abdominal surgery over a six-month period in 2014, not including women undergoing cesarean section. Many surgeries involved the appendix or gallstones.
Sixty percent of the patient records collected came from high-income countries like the U.S., U.K. and Sweden, while the rest came from middle-income countries like Egypt and low-income countries like Mozambique.
There were 174 deaths within 24 hours of surgery and 404 deaths within the following 30 days. In the first 24 hours, mortality rates were about 1 percent in high-income countries, 2 percent in middle-income countries and 3.4 percent in low-income countries. By the 30-day mark, mortality rates were 4.5 percent, 6 percent and 8.6 percent, respectively.
Trauma leading to surgery was more common in lower income countries, according to the results in the British Journal of Surgery.
"There is a lack of safe and affordable surgery in low- and middle-income countries," Bhangu said.
"This means that patients can take some days to get to hospital, or may choose to avoid medical treatment in the first instance due to cost," he said. "In total, this may be creating the situation where diseases are more advanced when the patient reaches the operating theater."
Some strategies, like using a surgical safety checklist, may be effective in high and low-income settings, or may be a marker of safer hospital systems, he said.
"Given the lack of essential resources and immediate availability of highly trained providers of all cadres, including technicians, nurses, physician's assistants, physicians and surgeons, surgery is more dangerous in many low-income countries than it is in higher income countries," said Dr. Barclay Stewart of the University of Washington in Seattle, who was not part of the new study.
"We all must advocate for greater global attention on the extreme inequity that is represented by the lack of emergency and surgical care in low-income countries," Stewart told Reuters Health by email. "This is particularly true for those of us who work in the global health community, which is often focused on highly politicized conditions that exact a lesser toll on societies than conditions that require emergency and surgical care."
Living in richer countries is associated with increased survival in general, not just for emergency surgery, said Dr. Mark G. Shrime, director of research in the Program in Global Surgery and Social Change at Harvard Medical School in Boston who also was not part of the new study.
Currently, 5 billion people around the world don't have this sort of access to available, safe, affordable and timely care, Shrime told Reuters Health by email, "and, of those who do, 80 million people impoverish themselves every year trying to get surgery."