(iStock)
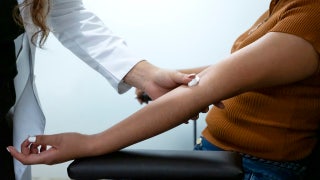
As rates of melanoma rise, scientists at the University of Pittsburgh School of Medicine are suggesting a possible solution: screenings at primary care physicians’ (PCP) offices. In a study presented Tuesday at the American Society of Clinical Oncology (ASCO) annual meeting in Chicago, researchers found that, on average, participants screened for skin cancer at their PCP had melanomas that were nearly twice as thin as those who were not screened by their doctor.
Not all PCPs are trained in detecting melanoma, and usually patients have to go to their dermatologist to get a screening. According to the American Cancer Society, melanoma accounts for only 1 percent of skin cancers but kills a majority of skin cancer patients. This year, more than 10,000 people are predicted to die of the disease, and more than 76,000 may be diagnosed.
"Our findings suggest that PCP screening is an effective way to improve early detection of melanoma, which could potentially save lives," lead study author Laura Ferris, M.D., Ph.D., associate professor of dermatology at the Pitt School of Medicine, said in a news release.
Ferris and her team trained PCPs involved in the study to screen for melanoma based on a German program thought to make the procedure easier. PCPs conducted the screening during office visits to patients ages 35 and older, and during the first year of the program, 2014, 15 percent of the nearly 334,000 eligible patients received the screening. On average, the participants who underwent the evaluation had melanomas that were nearly twice as thin as those who didn’t get the screening. Earlier-stage, thinner melanomas allow for quicker treatment and better prognoses.
Researchers also noted that among the screened group, only 5 percent had concerning melanomas thicker than 1 millimeter, which require biopsy of a nearby lymph node to ensure no metastasizing has occurred, compared with 20 percent of the unscreened group.
"The PCP screenings prevented a lot of people from needing more aggressive therapy. Additionally, we did not see a high rate of false positive biopsies, in which no skin cancer was present, nor did we see a high rate of unnecessary dermatology referrals or skin surgeries, all of which suggest that the program did not simply drive up health care costs needlessly," Ferris, also a member of the Melanoma Program, University of Pittsburgh Cancer Institute, said in the release.
Study authors said that notably, half of the screened patients were men, who are at a greater risk of dying from melanoma and have been underrepresented in other skin cancer screenings so far.
"It's exciting that our approach improves detection in this especially vulnerable population," Ferris said in the release.