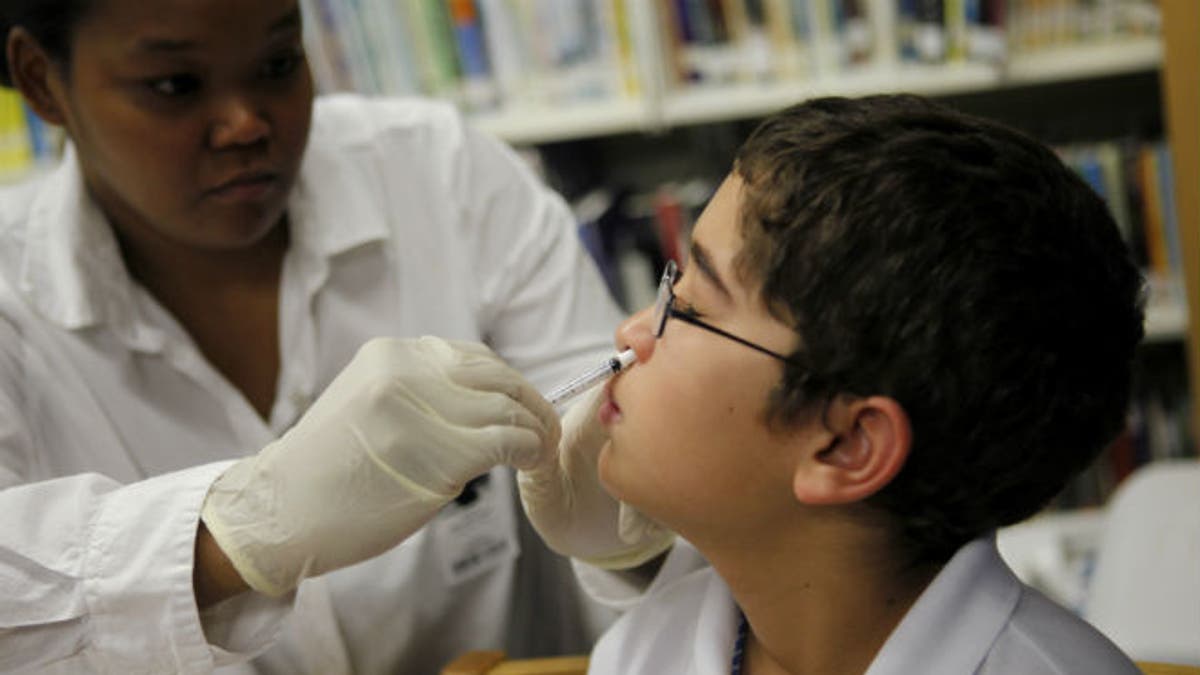
(REUTERS/Carlos Barria)
ATLANTA — The road back to the nostrils of the nation’s children will likely take longer than the makers of the influenza vaccine FluMist would have liked.
And that, some observers worry, could put in jeopardy the future of the country’s only non-injectable flu vaccine, a product thought to be an important component of the response to future flu pandemics.
Once a darling of pediatricians and parents, the nasal mist vaccine was not recommended for use in the United States this winter because studies showed it offered limited protection in recent years.
On Wednesday, officials from MedImmune, the division of AstraZeneca that makes the vaccine, reported on their efforts to fix the vaccine during a meeting here of the Advisory Committee on Immunization Policy, the expert panel that counsels the Centers for Disease Control and Prevention on vaccine use.
More From Stat News
Read more: FluMist mystery on experts’ agenda: Why was it so weak, and only in US studies?
It was the ACIP that last June decreed that FluMist should not be recommended for use this flu season — a move that effectively denied the product access to its most important market.
Though MedImmune officials wrote a letter to a scientific journal late last year suggesting they may have pinpointed the problem, the presentation to ACIP revealed there are still big questions.
“It’s not clear to me what the reason for the lack of vaccine effectiveness has been. There are a number of hypotheses that are being pursued,” ACIP member Dr. Robert Atmar said after the presentation. Atmar is interim chairman for infectious diseases at Baylor College of Medicine in Houston and a vaccines researcher; in the past, he has studied this vaccine.
The vaccine is administered as a mist that is puffed up a nostril. It contains live but attenuated — weakened — viruses that work by initiating infection, which in turn alerts the immune system to recognize and respond to those viruses during flu season. Because the vaccine viruses have been weakened, they do not make recipients sick with flu.
FluMist is a quadrivalent vaccine, meaning it protects against four different types of flu viruses.
The problem with FluMist, which began in 2013, specifically relates to one component of the vaccine — the influenza A virus known as H1N1.
H1N1 is a family of viruses that has been infecting people for much of the last century. But in the flu pandemic of 2009, a distant cousin — a flu virus that had been circulating in pigs — pushed out the previous H1N1 viruses. The replacement viruses — officially called H1N1pdm09 in an attempt to minimize confusion — do not appear to work as well in the nasal mist vaccine. MedImmune scientists have tried two different versions of the new H1N1 viruses in the vaccine, with similarly disappointing results.
But company officials told the committee that a new candidate has been identified that appears to function more like the pre-2009 H1N1 viruses.
Dr. Jeffrey Duchin, head of communicable diseases epidemiology with the Seattle and King County health department, described that news as hopeful.
“It’s more important that they find a strain that works than they find out what was wrong with the strain that didn’t work, in my opinion,” said Duchin, a non-voting member of the committee representing the National Association of County and City Health Officials.
But Atmar remained concerned. “If that is what the problem is, then the steps they’re taking may address it adequately. But if they’re wrong, then we may still have problems with their quadrivalent vaccine.”
There are a number of factors that further complicate the path back to a recommendation for use from the ACIP.
Paradoxically, studies conducted on FluMist outside the United States didn’t show the same poor findings — or at least not to the same degree. Canadian vaccine advisers last year dropped their assessment that FluMist was superior to injectable vaccine in children, based on its recent performance there. But they did not recommend against its use. Britain and Finland also continue to use the vaccine.
But any hopes that vaccine effectiveness data for this flu season from those countries might cast FluMist in a better light have been dashed because H1N1 is a non-player this flu season in North America or Europe. Another influenza A virus, H3N2, has been the dominant flu pest this winter.
ACIP members noted that until there is a flu season in which H1N1 viruses again play a big role, there won’t be a clear way to test whether replacing the vaccine virus has fixed the problem. There is no way to predict when H1N1 viruses will next make up a significant portion of flu activity.
The officials said MedImmune is testing the new H1N1 vaccine virus in ferrets — the best animal model for flu — and in cell cultures derived from human respiratory tract cells.
Read more: Contentious flu vaccine policies at hospitals are based on flawed research, study says
That led to a discussion of what kind of evidence might persuade the committee to give FluMist another chance if it turns out to be several years before there is enough H1N1 flu activity to test the updated vaccine.
Atmar worried that if the committee moves too soon, it could undermine its credibility. “We don’t want the public to lose confidence if the vaccine ends up being recommended again and the problem hadn’t been solved,” he said.
But the sustainability of the vaccine was clearly also on some minds. Dr. Bruce Gellin, director of the National Vaccine Program Office and a non-votin member of the committee, asked how long MedImmune could stay in the flu vaccine business without an ACIP recommendation for use in the US.
Dr. Raburn Mallory, senior director for clinical development of vaccines, gave a diplomatic but vague answer, saying the company is committed to protecting children from influenza. AstraZeneca declined STAT’s request to interview Mallory after the meeting.
“We remain committed to FluMist Quadrivalent and working with the CDC and ACIP,” AstraZeneca said in a brief emailed statement. “We look forward to continuing conversations with the ACIP as data becomes available in the coming months.”
Earlier this month the company said it expected to make vaccine available in the US for the 2017-2018 flu season. It did not repeat that prediction at or after the ACIP meeting.
The question of how long a company can to remain in vaccine production when its major market remains out of reach hangs over these discussions, Atmar acknowledged. “That’s a reality,” he said. “That’s a real concern. And I’m sure that’s something they’re thinking about.”







































