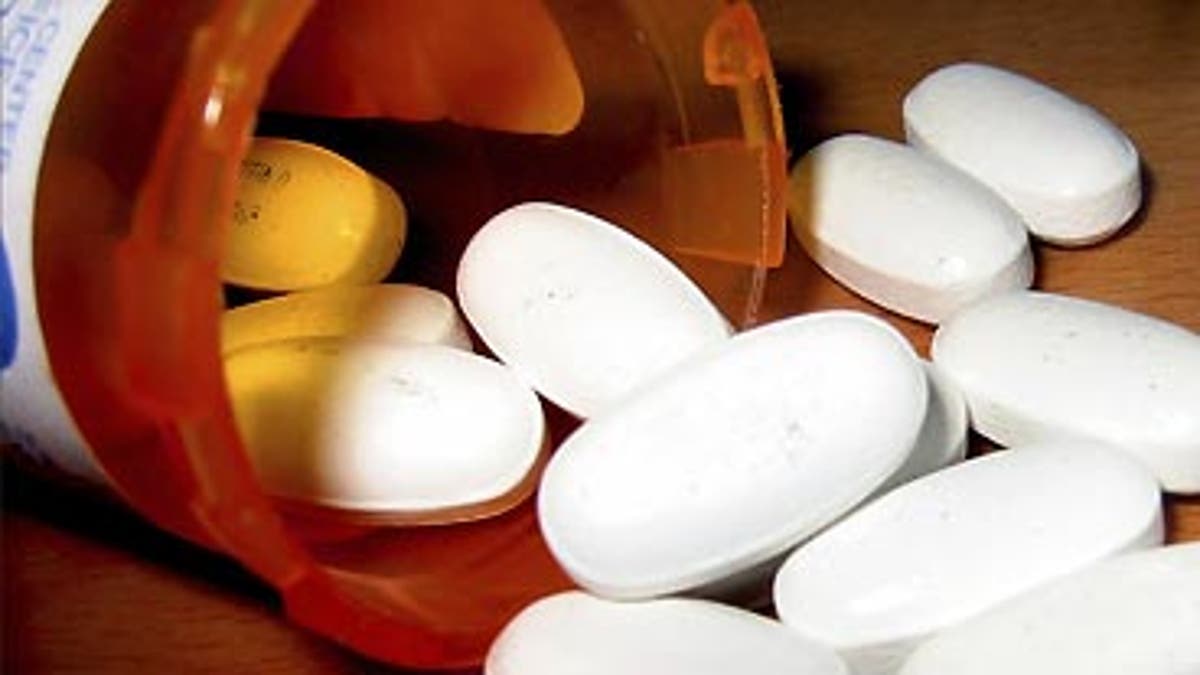
People taking certain prescription sleeping pills are four times more likely to die than people who do not—even if they are only taking low doses of the medication, according to researchers. The drugs are also linked with a significantly increased risk of cancer among people taking high dosages.
Researchers from the Scripps Clinic Viterbi Family Sleep Center in La Jolla, Calif., and the Jackson Hole Center for Preventative Medicine, in Jackson, Wyo., tracked the survival of more the 10,500 people who were prescribed sleeping pills for approximately 2.5 years and then compared those rates with more than 23,500 people who had not been prescribed sleeping pills. The average age of the participants was 54.
The study, published in the online journal BMJ Open, included common sleep medications such as benzodiazepines, non-benzodiazepines, barbiturates and sedative antihistamines, which are sold commercially under names like Ambien, Restoril, Sonata and Lunesta.
Participants assigned low doses of any of these medications—less than 18 pills per year—were more than 3.5 times more likely to die than people who did not take sleep medication, while those prescribed between 18 and 132 pills were more than four times more likely to die.
For example, the researchers said there were 265 deaths among 4,336 people taking Ambien—the most frequently prescribed sleeping medication in the study—compared with 295 deaths among the 23,671 people who had not taken sedatives or sleeping pills in the same time period.
People who took more than 132 pills a year were not only five times more likely to die, but were also at greater risk of developing several types of cancer, and 35 percent more likely to be diagnosed with any type of cancer, overall.
“The sense has been with newer medications that shorter-acting drugs are safer, and the major take-home message from our study is these drugs are not safer,” Dr. Robert Langer, principal scientist for the Jackson Hole Center for Preventative Medicine and co-author on the study, told FoxNews.com.
“The medications may have role in temporary use of insomnia, but need to be used sparingly,” Langer added. “People need to go in with their eyes wide open that the risks are there.”
These associations held even after taking into account other factors such as lifestyle, weight and previously diagnosed cancer, and were observed in every age group. The greatest relative risk of death was among those aged 18 to 55.
“That was actually the most disturbing thing,” Langer said. “We tried to rule out virtually any other explanation and looked at all other major diseases…No matter how we looked at things, the risk still held—and increased as intake increased.”
Langer and his colleagues speculated that the increased risk of death may be due to side effects of the medications, such as driving while asleep and unaware; sleep apnea, which can increase the risk of cardiovascular disease and stroke; and potential associations with pneumonia.
According to statistics, more than one in 20 U.S. adults took a sleeping pill in 2010. While the researchers said the link between sleeping pills and death does not necessarily imply a cause-and-effect relationship, they said growing data supports finding alternatives to sleeping pills for the treatment of insomnia.
Meanwhile, past research in rats has linked sleep medications with chromosomal damage, which could account for the increased risk of cancers such as lung, colon and prostate cancers.
"Although the authors have not been able to prove that sleeping pills cause premature death, their analyses have ruled out a wide range of other possible causative factors,” commented BMJ Open editor Dr. Trish Groves in a press release. “So these findings raise important concerns and questions about the safety of sedatives and sleeping pills."








































