Ruth Felton, of Tiburon, California is a real fireball, even in her 90s.
Her daughter, Sherry Brier, interviewed her while she was working out on a rowing machine at a gym where she had been going for several years When Brier asked if she felt it helped, her mother replied with a twinkle “I hope so,” as she continued to row.
But when she was 95, Felton fell late one night at home and was taken by ambulance to the emergency room, where doctors found she'd broken her pelvis in three places.
Brier said the doctors told her that after leaving the hospital, her mother "would have to go to rehab and learn to walk again and learn to function again."
But Brier and her sisters were told that would mean a skilled nursing facility, which is expensive. But, if she "stayed three full nights, we were told that was the criteria for having Medicare pay for the rehab," Brier said.
There's a nasty catch, however-- many people in the hospital are not officially considered "in-patients" but rather "under observation" although the difference is not obvious.
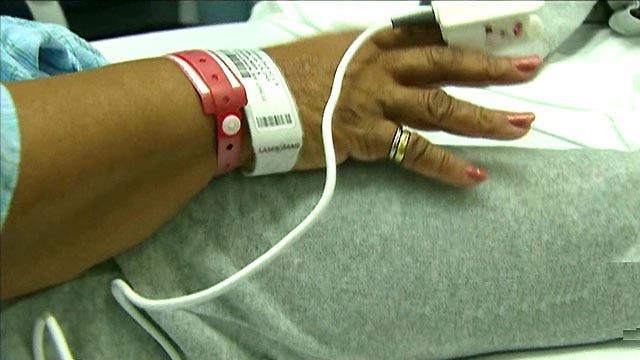
Says Toby Edelman of the Center for Medicare Advocacy, “Once they are in the hospital and in a bed for several days, getting care and treatment and medicine and food, (a) wristband, they think they're in-patients. People have no idea that they're out-patients."
Felton’s daughters learned just ten minutes before her discharge that she was only under "observation" -- meaning Medicare would pay nothing for nursing care and rehab -- leaving them to pay a $17,000 bill.
Many others pay tens of thousands more. Rep. Joe Courtney, D-Conn., says "the inspector general calculated that there were 600,000 cases across the country just last year alone."
And ObamaCare itself contributes to the problem.
Hospitals say they're caught in the middle with the government challenging medical decisions, and imposing fines under ObamaCare if they admit too many in-patients.. and then the patients return.
Ashley Thompson of the American Hospital Association says, "hospitals are penalized for excessive readmissions and that is for any patient that's admitted. That might be one of reasons why physicians are more cautious admitting patients to the hospital."
Scott Gottlieb is a doctor and analyst at the American Enterprise Institute and serves on a board that examines physician practices at hospitals.
"They are trying to keep more patients on observation so they don’t have to formally admit them to the hospital," he says.
One reason? The government hires contractors -- which some call bounty hunters -- to go out and challenge Medicare claims going as far back as three years, giving them 9 to 12.5 percent of any claim denied, creating a financial incentive for second guessing doctors and hospitals.
Ashley Thompson of the American Hospital Association says, "These claims are held up in the appeal process for two-and-a-half years. There's over $1.5 billion that's tied up right now as hospitals are appealing these denials."
Although they win 70 percent of their appeals, that doesn't help families stuck with tens of thousands of bills from skilled nursing facilities.
Gottlieb blames the government.
"So you get hospitals, basically overshooting and keeping more patients on observation status because they know if they make the wrong decision and admit a patient that could have been put on observation status, they're gonna face a penalty when the auditors come in."
Courtney wants to fix all this. He has 136 co-sponsors from both parties for a bill requiring that any three-day stay at a hospital be entitled to Medicare payment for skilled nursing care.
Meanwhile, Sherry Brier has been fighting the Medicare bureaucracy for months. She calls the whole situation a travesty.