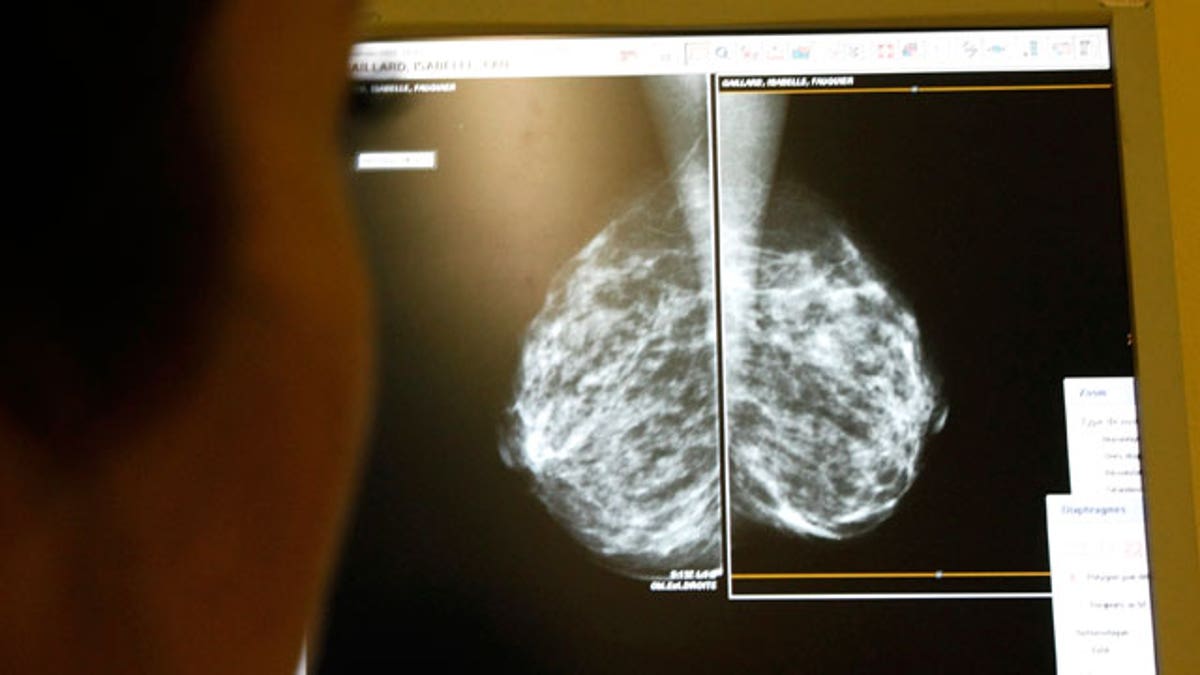
An injectable form of progestin-only birth control has been found to double the risk of breast cancer in young women after just a year or more of use, a new study suggests.
According to the researchers, this is the first large-scale U.S. study to examine the link between depo-medroxyprogesterone acetate (DMPA) and an increased risk of breast cancer. DMPA is the main component in the branded progestin-only contraceptive Depo-Prevara.
The contraceptive contains the same type of progestin used in a certain kind of menopausal hormone-therapy regimen that uses both estrogen and progestin to treat the symptoms of menopause. A clinical study of the regimen by the Women’s Health Initiative revealed an increased breast cancer risk in the postmenopausal women who utilized the therapy.
These findings were what prompted the researchers to study DMPA specifically.
“We know that women who use DMPA - it works by providing a high enough level of progestin that confers contraception for a long period of time,” said Dr. Christopher Li, a breast cancer epidemiologist at the Fred Hutchinson Cancer Research Center in Seattle, Wash., and the lead author of the study. “Other studies have implicated progestin as potentially harmful for the body. Such a sustained incidence of progestin could increase this risk.”
Li and his team conducted a case controlled study of 1,028 women aged 20 to 44 in the Seattle area who had been diagnosed with breast cancer. After gathering information about their birth control methods, the researchers then compared this group to another group of similarly aged women who had no history of breast cancer.
The research spanned over a five-year period and ultimately concluded that the women who had used DMPA for at least 12 months had a 2.2-fold increased risk of breast cancer. It also found that those who used DMPA for less than a year or who had stopped using it more than a year ago did not have an increased risk – meaning a discontinuation of use could help prevent women from contracting breast cancer.
While studies of this kind have been conducted in other countries around the world – such as Kenya, Thailand, Mexico and Costa Rica – Li said the results were somewhat distinct due to the differences in how women use contraceptives in less-developed nations.
“There have been other studies conducted in other countries, but the way this contraception is used in developing countries is much different,” Li said. “In the U.S., this contraception is primarily used by women who have never been pregnant, but in other countries it is used by women who have been pregnant to prevent further pregnancy.
“The breast tissue is more susceptible to potential carcinogens before women have their first pregnancy, so that’s why these results are different from what we see in other countries.”
Because of the discrepancy in findings, Li noted that people should put these results into context. But, he also said it’s important for women to know what they’re putting in their bodies.
“Breast cancer is a rare disease among young women,” Li said. “This doubling of a risk - it probably has little impact on the disease burden overall. But the main thing is that women need to have conversations with their doctors to understand what should be the right contraception.”
The study is published online ahead of the April 15 print issue of Cancer Research.








































