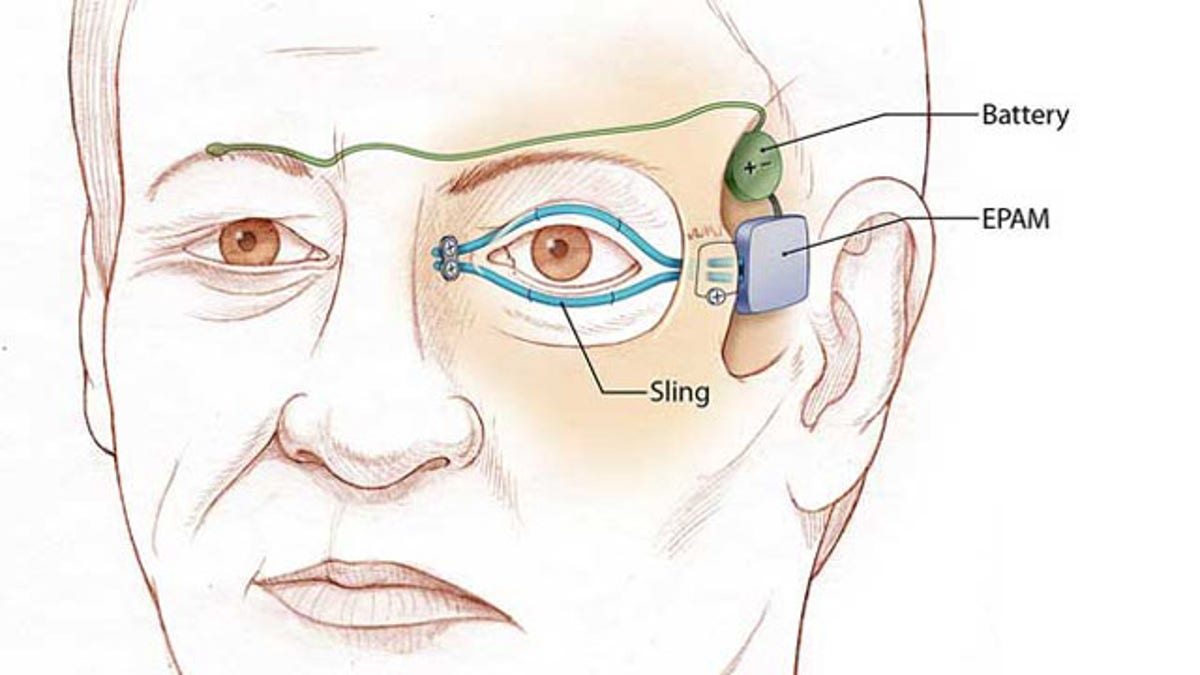
Illustration of left eyelid "sling" that is attached to an artificial muscle. The power supply and artificial muscle are implanted in the temple. When the normal right eyelid blinks, the electrical sensor (green) sends a signal to the battery to activate the artificial muscle. (University of California Regents)
Surgeons made cadavers blink with artificial muscles, experiments that could in the future help restore the ability of thousands of patients with facial paralysis to open and close their eyes on their own.
Some people can't blink their eyes. In most patients with so-called permanent eyelid paralysis, the cranial nerve that controls involuntary eye blinking has been damaged by an accident, stroke, injury or surgery to remove a facial tumor.
Many of these patients have no functioning nerves nearby that can be rerouted to close the eyelid. Others are born with Mobius syndrome, which is characterized by underdeveloped facial nerves. These people are expressionless and can neither blink nor smile.
Without lubrication from the blinking lid, the eye can develop ulcers and the person can eventually go blind. Currently, eyelid paralysis is treated by one of two approaches. One is to transfer a muscle from the leg into face. However, this option requires six to 10 hours of surgery, creates a wound that can impair the body elsewhere, and is not always suitable for elderly or medically fragile patients.
"I would estimate under 100 of those are done in the United States every year," said researcher Craig Senders, an otolaryngologist at the University of California at Davis.
The other treatment involves suturing a small gold weight inside the eyelid, which helps close the eye with the aid of gravity. Although such therapy is successful in more than 90 percent of patients, the resulting blink is slower than normal and cannot be synchronized with the opposite eye, and some patients also have a hard time keeping the weighted lid closed when lying down to sleep. In the United States, roughly 3,000 to 5,000 patients undergo this surgery every year.
To look for an alternative, surgeons at the University of California at Davis experimented with artificial muscles with six donated human cadavers.
"This is the first-wave use of artificial muscle in any biological system," said researcher Travis Tollefson, a facial plastic surgeon at the University of California at Davis.
The artificial muscle they used acts like human muscle by expanding and contracting in response to electrical input. Developed by engineers at SRI International of Palo Alto, Calif., the muscle includes a piece of soft acrylic or silicone sandwiched between carbon particle electrode layers. When a current is applied, the outer layers get pressed together and squash the soft center, expanding the artificial muscle as a whole. When the charge is removed, it contracts.
The surgeons placed the artificial muscle and its battery into a natural hollow at the temples of the cadavers to disguise its presence. It was then attached to cords of either Gore-Tex fabric or soft connective tissue harvested from the corpses' temples that were inserted around the eye. The resulting "sling" of sorts was secured in place with small titanium screws in the small bones of the eye. Whenever the artificial muscle contracted and expanded, it pulled this sling, blinking the eye.
Making cadavers blink "wasn't disconcerting to us in any way," Senders recalled of their work. "I can understand how others might feel that way about it, but from our standpoint it was a tremendous victory toward a goal that can help so many people."
For patients who have one functioning eyelid, a sensor wire threaded over the normal eyelid could detect the impulse triggering this natural blink and fire the artificial muscle at the same time. When it comes to patients lacking control of either eyelid, an electronic pacemaker similar to ones used to regulate heartbeats could blink the eyes at a steady rate. They may also design these systems to respond to magnetic fields, either to get deactivated so that patients can sleep or as a means to recharge their batteries.
Future research with synthetic muscles could also give children born with facial paralysis a smile and help many patients regain control of other parts of the body.
"There are many ideas and concepts where this technology may play a role," said Tollefson.
The researchers estimated their procedure might be available for patients within the next five years, and they are now conducting animal studies with live gerbils. They detailed their research in the January-February issue of the journal Archives of Facial Plastic Surgery.
Copyright © 2010 LiveScience.com. All Rights Reserved. This material may not be published, broadcast, rewritten or redistributed.







































