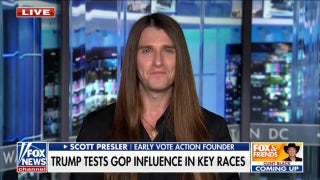
Dec. 21, 2011: Dr. William Sullivan, an emergency department physician at the University of Illinois at Chicago hospital, is seen through a re-enforced window of a psychiatric evaluation room in Chicago December 21, 2011. (REUTERS)
To the outside world, it came across as mood swings and anger. But Regina Cullison would later be told by psychiatrists she struggled with depression and anxiety—and that she needed help. And that is where her trouble began and ended.
According to her mother, there were few psychiatrists in the county who took private insurance. When Ms. Cullison lost her job as a dentist's assistant, and with it her insurance, she switched to a nonprofit facility. Doctors came and went, and none stayed long enough to establish a regular pattern of treatment.
After two years, Ms. Cullison abandoned her search for professional help and tried marijuana. Her mother, Carolyn Cullison, who is the director of a mental-health peer support group, said that helped push away the demons. But in May, while living together, the pair argued. Ms. Cullison apologized, retreated to a bedroom and shot herself. She was 26.
As hard as it might be to acknowledge having a mental-health illness, finding professional help can be even harder.
Last year, according to the U.S. Department of Health and Human Services, almost 91 million adults lived in areas like here where shortages of mental-health professionals made obtaining treatment difficult. A departmental report to Congress earlier this year said 55 percent of the nation's 3,100 counties have no practicing psychiatrists, psychologists or social workers, a combination of budget cuts and doctors leaving the profession.
Even in well-served areas, such as Washington, D.C., and Massachusetts, demand is so high practitioners frequently decline to take new patients or private insurance, according to a Kaiser Family Foundation survey.
Such shortages are expected to only grow now, as the federal health-care law goes into effect and allows more people to seek help. Indeed, according to the National Association of State Mental Health Program Directors, some 6.8 million uninsured people with a mental illness will gain coverage after federal and state health insurance exchanges implement the new law. More people will be chasing after scarce resources, an influx that will "overwhelm if not inundate" the field, said Dr. Jeffrey Lieberman, president of the American Psychiatric Association.
For years, much of the country's struggles with mental-health treatment remained out of the spotlight. But a series of high-profile shootings over the past two years, such as in Aurora, Colo., and Newtown, Conn., and Tucson, Ariz. has drawn attention to a host of deficiencies. Those include privacy laws that end up limiting families' ability to guide their children's care and a tightening of commitment standards that exclude all but the most obviously violent patients. The result is increasing and sometimes fatal encounters with police and prisons overflowing with the mentally ill.