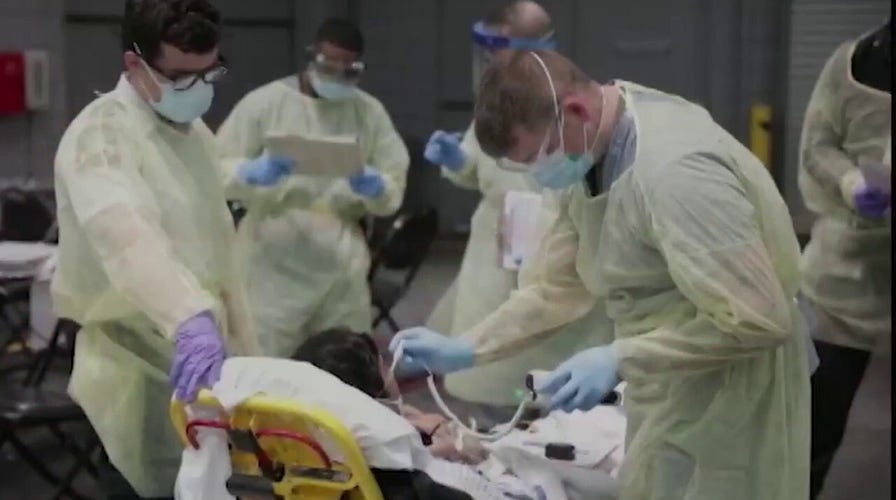
How hospitals were incentivized to diagnose patients with COVID-19
Dr. Marc Siegel addresses the 20% add-on payment hospitals receive for treating coronavirus patients and if this may have led to fraud
Get all the latest news on coronavirus and more delivered daily to your inbox. Sign up here.
Americans cannot be blamed for feelings of suspicion and confusion surrounding publicized COVID-19 death counts. Disparities in the way our health care system counts and catalogs these fatalities shift attention away from important health risks and how to mitigate them.
Dr. Deborah Birx, the response coordinator for the White House Coronavirus Task Force, inadvertently sparked controversy when she said suspected COVID-19 deaths were included in the overall reported death count. "The intent is ... if someone dies with COVID-19 we are counting that," she said.
Death is more often from a variety of factors, but when Americans are tuned in watching our nation’s leaders reporting on daily coronavirus cases, uniformity and full transparency are crucial to instill public trust and minimize insurgency.
NIKKI HALEY: CORONAVIRUS STIMULUS – HELP THOSE TRULY IN NEED BUT STOP WASTING BILLIONS ON OTHERS
Information from cause-of-death documentation is used for policy-making, resource allocation, determining the need for prevention programs, and monitoring overall public health trends. Therefore, uniformity in reporting causes of death is the most efficient mechanism to ensure the quality of the conveyed information.
The International Classification of Diseases (ICD) provides codes to categorize illnesses and external causes of injury or disease and is the standard diagnostic tool for epidemiology, health management and most clinical purposes. The use of the ICD allows comparability of morbidity and mortality statistics across countries and contributes to a better understanding of the health of nations.
More from Opinion
The ICD includes coding rules for causes of death. These rules identify the single condition on the death certificate that is considered most informative from a public health point of view, called the “underlying cause of death.” The single underlying cause of death is defined as “the disease or injury which initiated the train of morbid events leading directly to death.”
From a public health perspective, it is necessary to specify the sequence of events, distinguishing the precipitating or underlying cause from the consequences of the condition. For example, if someone who suffers from a heart attack and diabetes dies, the underlying cause of death is more often attributed to diabetes. The heart attack that caused the fatal event is usually listed as secondary given that diabetics are up to four times more likely to die from heart disease than adults without diabetes because the disease itself predisposed the individual to the subsequent heart attack.
Regarding reporting of cases in the current pandemic, some states, like Minnesota and California, list only laboratory-confirmed COVID-19 diagnoses. Other states, such as New York and New Jersey, are reporting all presumed cases, which is allowed under guidelines from the Centers for Disease Control and Prevention as of mid-April and is why an overnight increase of cases spurred the comment from Birx.
In addition to the need for more uniform reporting, greater transparency is required to maintain faith in the integrity of the data and the science behind it.
However, the lack of uniformity among the states is confusing and promulgates distrust in the system, particularly because reimbursement rates for COVID-19 patients are being publicly acknowledged as higher than for non-COVID-19 patients.
In addition to the need for more uniform reporting, greater transparency is required to maintain faith in the integrity of the data and the science behind it.
While state public health officials are reclassifying deaths to now include presumed deaths, they are also including “excess deaths.” Such cases were not obviously linked to the virus, but might not have occurred absent the pandemic, either from a chronic illness or because it overwhelmed the health care system.
In order to divert resources to the patients in the greatest need, hospitals were told to postpone non-emergency care, canceling “elective” surgical procedures and halting the appointments that are necessary to keep hospitals and medical practices in business.
A 2011 study highlighted the financial importance of surgical patients to hospitals: while only 29 percent of U.S. hospitalizations involved surgery, these cases accounted for 48 percent of hospital costs and, therefore, an even greater percentage of revenue. In order to prepare for the influx of COVID-19 patients, hospitals were forced to cancel procedures that provide nearly half of the revenue to keep them open.
CLICK HERE TO SIGN UP FOR OUR OPINION NEWSLETTER
The Coronavirus Aid, Relief and Economic Security (CARES) Act was intended to financially stabilize hospitals that faced short-term reduced income due to the ending of non-urgent procedures and increased costs for items like personal protective equipment and personnel. It did this by creating a 20 percent premium, or add-on, for COVID-19 Medicare patients. (The initial concern was that COVID-19 patients were being undercounted given the lack of access to testing, which is why presumed cases could be recorded in the numbers of deaths and hospitalizations.)
There have been whisperings of abuse of this add-on reimbursement rate but no official public reports that hospitals are exaggerating COVID-19 numbers to receive higher Medicare payments. Rather, the higher number of cases is more likely due to the counting of excess deaths.
However, there are sporadic reports that deaths are being reclassified as pertaining to COVID-19 despite physicians claiming they likely were not. For instance, a CBS4 Investigation found that the Colorado Department of Public Health and Environment reclassified three deaths at a Centennial nursing home as COVID-19 deaths, even though attending physicians ruled all three were not directly related to coronavirus. It is uncommon for public health officials to intervene on a physician’s cause of death declaration so full transparency as to why this is occurring is essential.
CLICK HERE TO GET THE FOX NEWS APP
It would behoove the scientific community to differentiate between those dying from direct consequences of the virus — for instance, acute respiratory distress syndrome and sepsis — or whether preexisting underlying conditions, exacerbated by COVID-19, are the true cause of death. Presenting Americans with the startling truth about how many of us live with chronic illnesses, which lead to higher death rates, may actually promote a healthier nation. Americans need to know that a healthier lifestyle can increase their ability to fight off a viral infection and perhaps lessen the need for government-ordered lockdowns in the future.
Once we can spend less time reporting daily death counts, we can begin focusing on the larger issues at hand: abundant existing chronic illness, a health system functioning at near capacity and a nation on the brink of revolt if leadership does not provide a creative means to re-opening the economy.
CLICK HERE TO READ MORE BY DR. NICOLE SAPHIER
Jason Chaffetz is a Fox News contributor who was the chairman of the U.S. House Oversight Committee when he served as a representative from Utah. He is the author of “Power Grab: The Liberal Scheme to Undermine Trump, the GOP, and Our Republic.”