Army Major Ed “Flip” Klein is an outdoorsman. Born in Arkansas, the 35-year-old always found a calming presence in nature, but when he was severely injured during a 2012 deployment to Afghanistan, he wasn’t sure he’d ever find that calm again.
In October 2012, Klein was a company commander in his seventh month of a nine-month deployment and out on patrol with one of his platoons. The troops split in two, and were walking through a compound with a mine detection K-9 and officer, who crossed over an improvised explosive device (IED) before Klein unknowingly stepped on it with his left foot and it detonated.
A medivac was called and an emergency plan that Klein had helped craft weeks earlier saw him taken from the point of his injury to a helicopter, and transported to the Kandahar Regional Military Hospital inside the so-called “golden hour.” The golden hour refers to the time period lasting for one hour or less following a traumatic injury in which there is the highest likelihood that prompt medical treatment will prevent death.
For the nine days following the explosion, Klein would remain unconscious, and unable to reach Walter Reed National Military Medical Center in Bethesda, Maryland, due to his unstable medical status and Hurricane Sandy battering the East Coast.
The first memory he can recall is waking up the day President Obama was elected to his second term.
‘Not many people prepare to come home in pieces’
At Walter Reed, surgeons like Army Lt. Col. Benjamin “Kyle” Potter, deputy chief of orthopedic surgery, were waiting to begin their work on Klein and other limb causality patients.
“I think because of the unique nature of blast wounds, even though we’ve written book chapters and papers and textbooks, it’s not something that you can sort of read about and understand and know how to manage until you’ve done it a lot,” Potter, who has operated on Klein multiple times, told FoxNews.com. “It requires us to be very creative in terms of our reconstructions.”
“Most of the limbs are missing when I get there,” Potter said. “Whether you’re completing the amputation or trying to close an amputation, it’s about trying to give them the most functional residual limb possible given the tissue you have to work with.”
The blast cost Klein both legs above the knee, his right arm above the elbow, and three fingers on his left hand. While his left thumb and index finger remain, muscle and nerve damage infringe on their functionality.
“As a soldier, I think a lot of people prepare to not come home,” Klein told FoxNews.com. “Not many people prepare to come home in pieces.”
In 2011, limb amputations among military personnel deployed as part of Operation Freedom’s Sentinel (OFS) in Afghanistan and Operation Enduring Freedom (OEF) in Afghanistan reached an all-time high. According to a Congressional Research Service report issued in August 2015, 257 of the 1,645 major limb amputations among service members dating back to 2001 came in 2011 alone. The report classifies a major limb amputation as loss of one or more limbs, the loss of one or more partial limbs, or the loss of one or more full or partial hands or feet.
"I think that, if you go to a faraway land and keep me safe, and you get injured, when you come back you should have everything you need to be normal.”
What lies ahead for patients at Walter Reed that differentiates them from most civilian amputee patients, is the immediate reintroduction to physical therapy at the Military Advanced Training Center (MATC) and community recovery. For Klein and others, seeing and interacting with other troops who have similar injuries but are further down the path of recovery serves as a source of inspiration and motivation.
‘They all want to be normal’
On-site physical therapy also offers an opportunity for Potter and his colleagues to follow up with patients without the hassle of making formal appointments.
“I typically try to walk through [MATC] at least twice a week, and just sort of check on the guys and gals, and see how everybody is doing and talk to the therapists,” Potter said. “Mostly just say hi, checking people’s hands, and sometimes you can sort of nip something in the bud, if it’s keeping a small problem from becoming a big one, because certainly when we put the last stitch in I don’t feel like my job as a surgeon is done.”
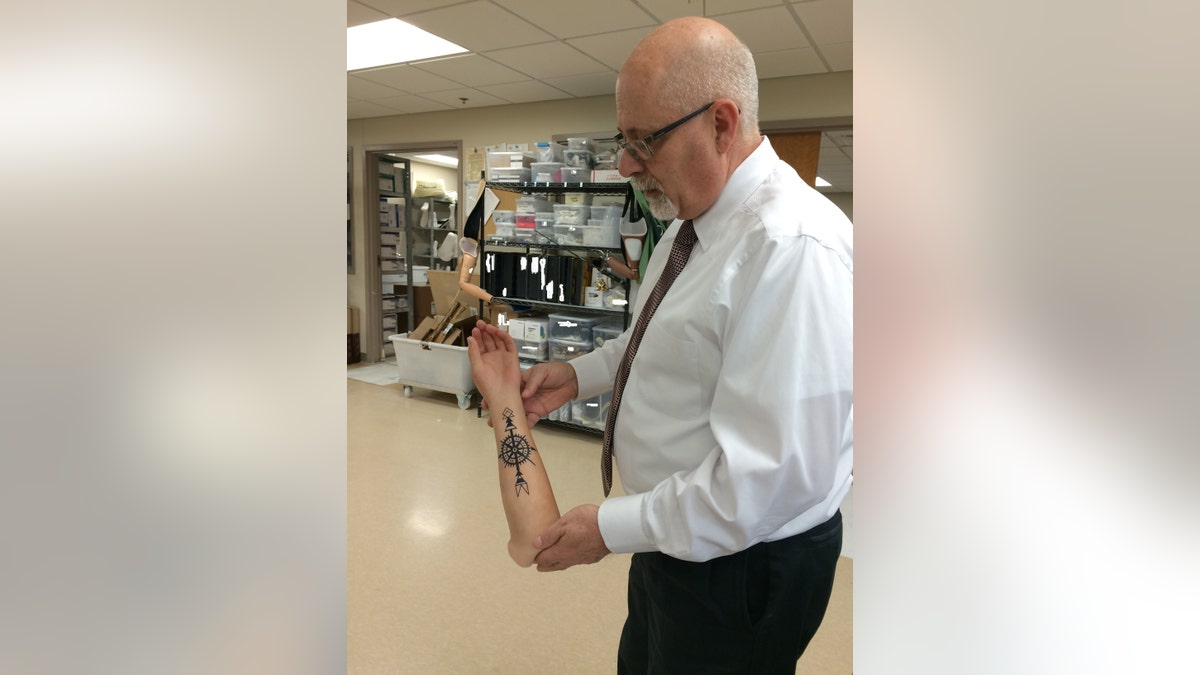
Dave Laufer, director of orthotics and prosthetics at Walter Reed National Military Center, displays a customized limb featuring a tattoo. (Fox News)
For patients like Klein, having a near-on-demand prosthetics department and 3-D medical application center can make all the difference. Dave Laufer, director of orthotic and prosthetic service, heads a staff that works hand-in-hand with patients and physicians to craft the perfect limb or attachment for amputees.
“When the war started, we started receiving casualties, and amputee prosthetic care was not near this end-state that it is now,” Laufer told FoxNews.com. “We had a lot of difficulties with matching proper devices with 23-year-old people that wanted to go out and do what they did before they got hurt, and we continue to have those same kinds of problems because the prosthetic industry is geared toward getting somebody up and able to work, and the third party reimburses are very, understandably, conservative in terms of what they’ll allow a civilian prosthesis to use in the care of a patient.”
In other words, while Walter Reed has the capacity to craft customized limbs and holders, they cannot be mass-produced by civilian companies due growing costs and limited reimbursement. From the start, Laufer and his team faced an uphill battle in trying to better many of the terminal devices, which is any type of limb that enables an amputee to connect to the world, like a hand, foot, or foot attached to a knee which then fastens to the socket.
For upper-extremity amputees, Laufer said devices are really geared toward independent activities and daily living, but not specific hobbies like fishing, golfing or swimming. There are also the patients who have received wounds that did not destroy the entire limb, but affected the functionality. On any given day, his department is buzzing with new limb attachments and designs to make the options better.
For Laufer, the process to help returning soldiers get to where they want to be is fulfilling. His department has seen arm devices recreated to have the same tattoos that the soldier had before his injury, terminal devices customized to have pictures of cats and dogs, and no request, so far, has proven to be too great.
“They all want to be normal,” Laufer said. “I think they’re new normal— they get used to that really quickly, that they have lost a limb. But then they want to be normal for their age group. Everybody goes out and runs, or they want to go out and play tennis, they want to do everything that anybody else at their age does, and I don’t think that’s unreasonable.
‘I let nature do the healing’
Such was the case with Klein, who quickly accepted that his limbs were missing. Due to training that he had received with the Army to prepare him to deal with both combat stress and life stress, he was able to recall the techniques needed to keep a positive outlook during recovery. He also found that his age and maturity helped him keep his focus on one day at a time.
“It never really occurred to me that I could not make it. It just never came up,” he said. “It’s almost like there wasn’t a whole lot of coping, I just woke up, and they said, ‘Hey, you’ve gotta live,’ and I said ‘OK, cool,’ and I just did it.”
Klein said he quickly learned that he wouldn’t know what he was capable of unless he continually pushed his limits. He credited exposure to other amputees in MATC with helping him set goals and explore his abilities, rather than focus on his disability. Through a Special Forces friend of his brother, he was hooked up with a program called Operation Healing Towers that would prove critical to his healing process. The program is run by Vietnam-era veterans and sponsors fishing expeditions in Alaska.
Initially, Klein didn’t know if he would be able to go because he wasn’t sure if he would be able to fish or even hold a pole, but Laufer's team had a solution.
Laufer’s team worked with Dr. Peter Liacouras, director of services in the 3-D Medical Applications Center at Walter Reed, to create a 3-D printed attachment that would be fastened to a terminal device, rather than act as the terminal device so that amputees would have the functionality of two hands. This device cut out the process of attaching a prosthetic hand to bait the hook, taking the hand off and attaching the pole to cast it, reeling in the fish and then removing the pole device to reattach the hand to deal with the fish. The new attachment attached to the existing hand device and was even fastened with a quick-release button for when the fish was reeled in.
Klein was fitted with the device and set off on his first trip to Alaska, where he met program founder Garry Morfit. In talks while out on the water with Morfit, Klein rediscovered his sense of self.
“I don’t think I would have even tried fishing with the pre-existing terminal devices because I had been introduced to them before, and I said that’s not going to be effective enough for me to put any energy into fishing. When they showed me the 3-D printed device, I allowed myself to say, ‘Well, that’s going to work well enough to overcome the physical challenges that I face in every other aspect.’”
Klein said the attachment gave him the opportunity to not just be a recipient of the experience, but to also be a part of the experience. The device gave him the confidence to go on the trip where he learned other skills he didn’t know he had, like the ability to climb a ladder out of the boat. He even credits the trip with helping to save his life when a catastrophic fire tore through his house shortly after his return. He had been in the basement with his dogs and had to climb stairs to get out. Without the trip, he’s not sure if he would have known how to climb the stairs.
Klein said he wants other amputees to understand the importance of pushing themselves and their recovery to the limits. He believes the practice has had a trickledown effect in every area of life. Laufer agrees, and is he ready to accept the challenge placed before him by amputees looking to define their new normal. He also admits that, while prosthetics have advanced over the last 15 years, there still is a long way to go but that’s what keeps his team motivated.
“It’s really fortunate to be in a medical center that has the command structure that supports our, you might call it, craziness,” Laufer said. “Because frequently there’s things that we do that cost money that just don’t work, and I have never had anybody in the leadership say to me, ‘You need to stop doing this, it just costs too much money.’ They always figure out a way to give me the resources I need.”







































