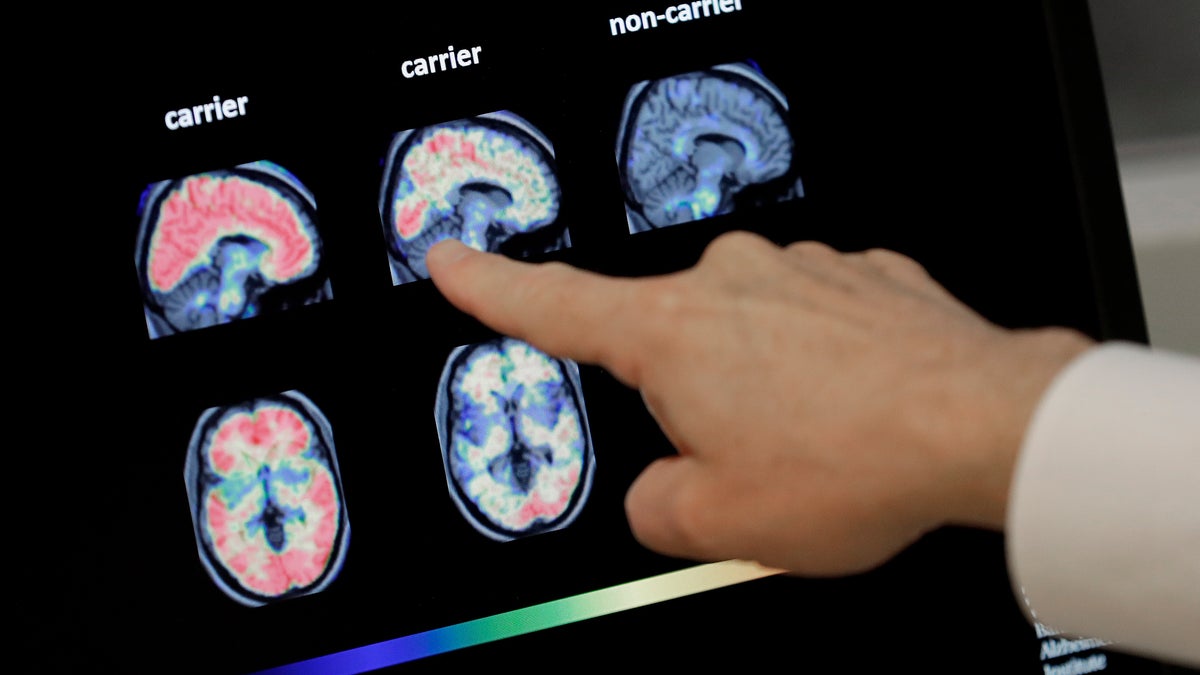
(AP Photo/Matt York)
Today there are new reasons to be hopeful about the fight against Alzheimer’s disease.
First, according to research published in Nature Medicine, the disease may be detectable by a blood test 16 years before the onset of symptoms. Such a test, which detects certain proteins that may indicate early stages of the disease, would allow doctors to identify those individuals most at risk of developing it.
Second, there is a new Alzheimer’s vaccine known as UB 311, produced by a small company, United Neuroscience, in Dublin, Ireland, that has just delivered promising results in phase two clinical trials in humans.
In phase two trials, which are blinded, one group receives the study drug while the other group may receive a placebo. The numbers in this trial are small – just 42 subjects with mild cognitive impairment (pre-Alzheimer) – but the results are impressive, especially considering that the vaccine was both well-tolerated and effective.
The response to the vaccine was a whopping 96 percent. It didn’t cause the brain inflammation that previous vaccines did, and it did reduce the amount of amyloid plaque that had built up in the brain. Subjects also performed better on tests of thinking and memory.
A longer-term extension of this trial is next, and if successful, I think we will see this vaccine in widespread use sometime soon, not just for those with early Alzheimer’s disease, but for those at risk as well.
Vaccines work by triggering the immune system to make antibodies against a certain protein often found on the surface of an invading virus or bacteria. In the case of Alzheimer’s, the protein (beta amyloid) is made by the body itself. It is a clunky protein that gums up the brain. UB 311 has been shown to produce high amounts of antibodies against amyloid.
According to the National Institute on Aging, “Alzheimer’s disease is an irreversible, progressive brain disorder that slowly destroys memory and thinking skills and eventually, the ability to carry out the simplest tasks. In most people with the disease – those with the late-onset type – symptoms first appear in their mid-60s.”
Alzheimer’s is the most common cause of dementia in the elderly. Close to 6 million people have it and the number is on the rise. It devastates not just the patient, but the entire family as the basic skills of self-care and ay-to-day function deteriorate. Patients lose not just memory but orientation and the ability to reason.
There continues to be debate about the cause of Alzheimer’s disease. It involves the buildup of amyloid plaques and tau proteins (neurofibrillary tangles) as well as the loss of connections between nerve cells. But what is the actual cause? Is the beta amyloid protein a cause or simply a result of the disease?
A clue to the answer came in 2012, when Icelandic researchers found a variant of a gene (APP) in 0.5 percent of the Icelandic population – a variant mutation that actually protects against Alzheimer’s disease. The gene itself produces the amyloid precursor protein which is broken down to form beta-amyloid. But in people who have the protective variant of this gene, the breakdown of the protein to beta-amyloid is markedly diminished. Icelanders with the mutation were found to be five times more likely to reach the age of 85 without developing Alzheimer’s.
CLICK HERE TO GET THE FOX NEWS APP
This evidence is indirect, but is nevertheless an important argument in the case for beta amyloid buildup in the brain as a direct cause of the disease. Previous attempts to target beta amyloid have not been successful, but the new vaccine is more promising.
If it continues to be proven safe and effective with larger groups, it may become a necessary tool in the immunological war against one of the most devastating diseases of all.








































