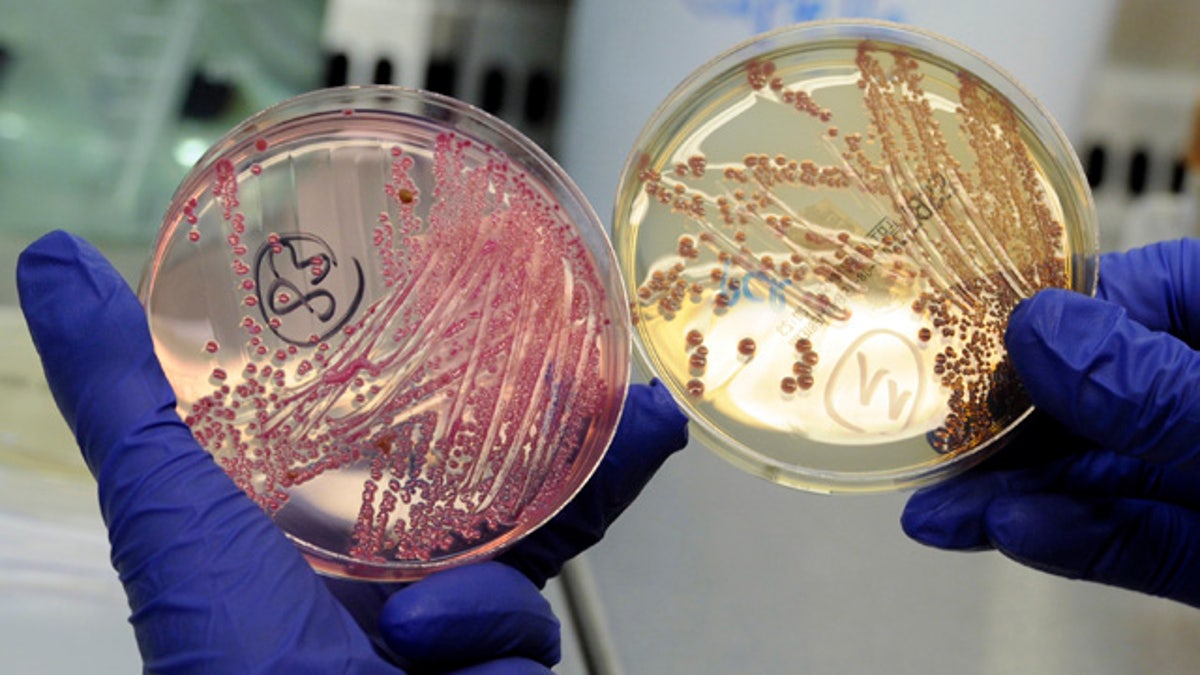
An employee holds petri dishes with bacterial strains of EHEC bacteria (bacterium Escherichia coli) in the microbiological laboratory of the Universitaetsklinikum Hamburg-Eppendorf (University Clinic Eppendorf- UKE) in the northern German town of Hamburg, June 2, 2011. (Reuters)
A strain of E. coli bacteria that killed 39 people in Germany, and sickened others in Europe and North America, was characterized by a lethal ability to stick to the surface of intestinal walls.
According to a study published Thursday in The Lancet medical journal, a team led by Helge Karch, a professor at the University of Munster, found the mixing of two genetic traits—a toxin that causes severe illness coupled with the uncommon adhesive qualities—is what made the germ so virulent and deadly.
One strain, called enterohaemorragic E. coli (EHEC), releases poisons called Shiga toxins. The other, called enteroaggregative E. coli (EAEC), adheres in a "stacked brick" fashion to epithelial cells which constitute the intestinal lining.
The team said the bug existed in a rare form for a decade and is a clone of a strain first detected in a young German patient in 2001. The germ is difficult to treat because it resists a wide scope of antibiotics called beta-lactams. To make matters worse, treatment with strong antibiotics may have wiped out rivals to the germ, the study suggested.
"The enhanced adherence of this strain to intestinal epithelial cells might facilitate systemic absorption of Shiga toxin and could explain the high frequency of progression to HUS," the study said. "Antibiotic resistance might also play a part if beta-lactam drugs used to treat the infection suppressed competing microbiota."
The study was funded by the German Federal Ministry of Education and Research and involved the team studying stool samples from 80 patients.







































