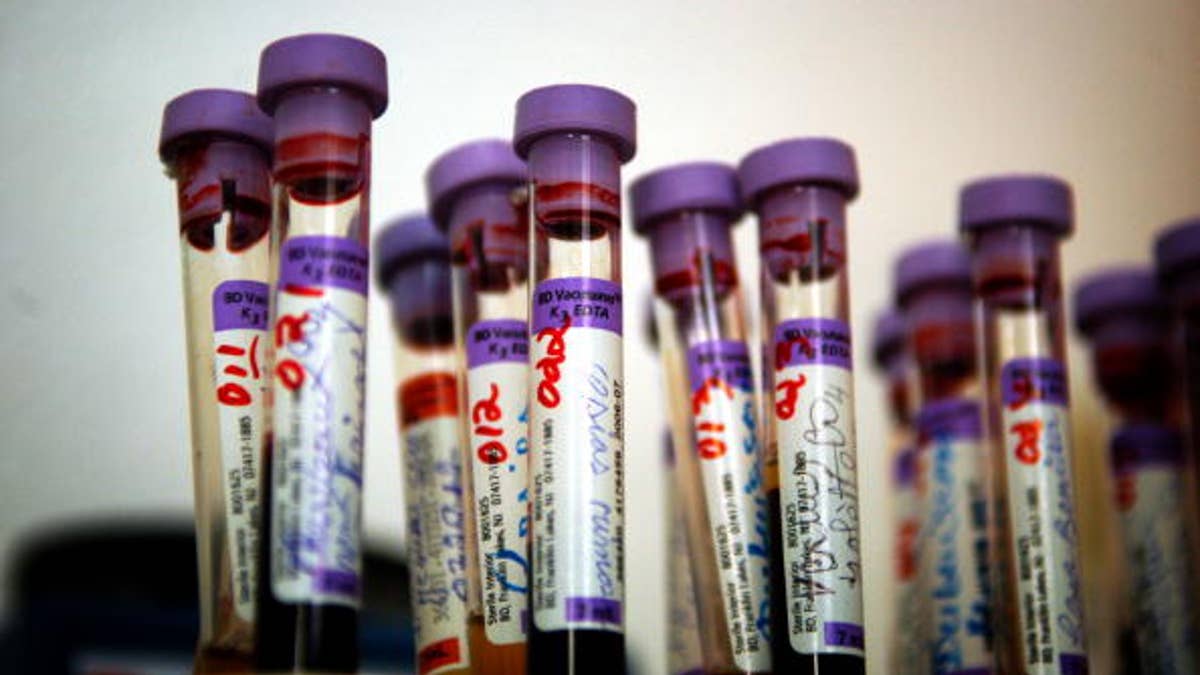
CANGE, HAITI - MARCH 24: Blood tests wait to be inspected at the lab of Zanmi Lasante Hospital March 24, 2005 in Cange, Haiti. Many HIV positive patients come to be hospitalized here, but the majority of HIV infected people will stay at home in their final stage of life and will die there as most hospitals in the country can not take them. (Photo by Shaul Schwarz/Getty Images) (Getty)
As researchers uncover more genetic variations in blood types, they are identifying new risks to patients needing transfusions.
Hospitals and blood banks are turning to more precise genetic methods to screen blood donors and recipients to prevent a mismatch, which can be fatal. The first such test to be approved in the U.S., called PreciseType, which promises quicker, more accurate results than traditional lab testing methods, has been adopted by 15 health systems and 25 donor centers including the American Red Cross, which supplies about 40% of the nation’s blood. PreciseType and similar tests are already in use in Europe.
Testing for an accurate donor-recipient blood match has gotten more complicated. People fall into one of four main blood groups—A, B, AB and O—and they have a so-called Rh factor that is either positive or negative. But scientists over the last few decades have discovered around 33 blood groups and continue to identify more. Each group also contains multiple variations that go to make up a patient’s exact blood type.
Most transfusions can be safely performed with routine matching to test for just the main blood types. But people who have had one blood transfusion and then need another may want to discuss with their doctor whether to have more sophisticated blood analysis.
The greatest risks are for people with certain diseases who need multiple transfusions. These include patients with cancer, intestinal bleeding, kidney failure, anemia and inherited blood disorders such as sickle cell disease.