Fox News Flash top headlines for April 23
Fox News Flash top headlines are here. Check out what's clicking on Foxnews.com.
Doctors have observed a strange trend in more COVID-19 patients: people with blood oxygen saturation levels that are very low but who aren't gasping for breath.
Although often quite ill, these patients are not presenting symptoms like most acute respiratory distress syndromes, which is a lung failure previously associated with the SARS outbreak in 2003 and other respiratory diseases.
These types of patients are alert and feeling relatively well, but their lungs are not performing their proper function. This presentation is known as "silent hypoxia" and it's causing some people to arrive at the hospital in worse health than they realize.
In a recent New York Times op-ed, Richard Levitan, an emergency room doctor who invented a procedure for teaching intubation -- the insertion of breathing tubes that many COVID-19 p patients require, explained that there might be a way around this issue.
CHALLENGE OF TRACKING COVID-19'S 'STEALTHY SPREAD' REVEALED IN NEW STUDY
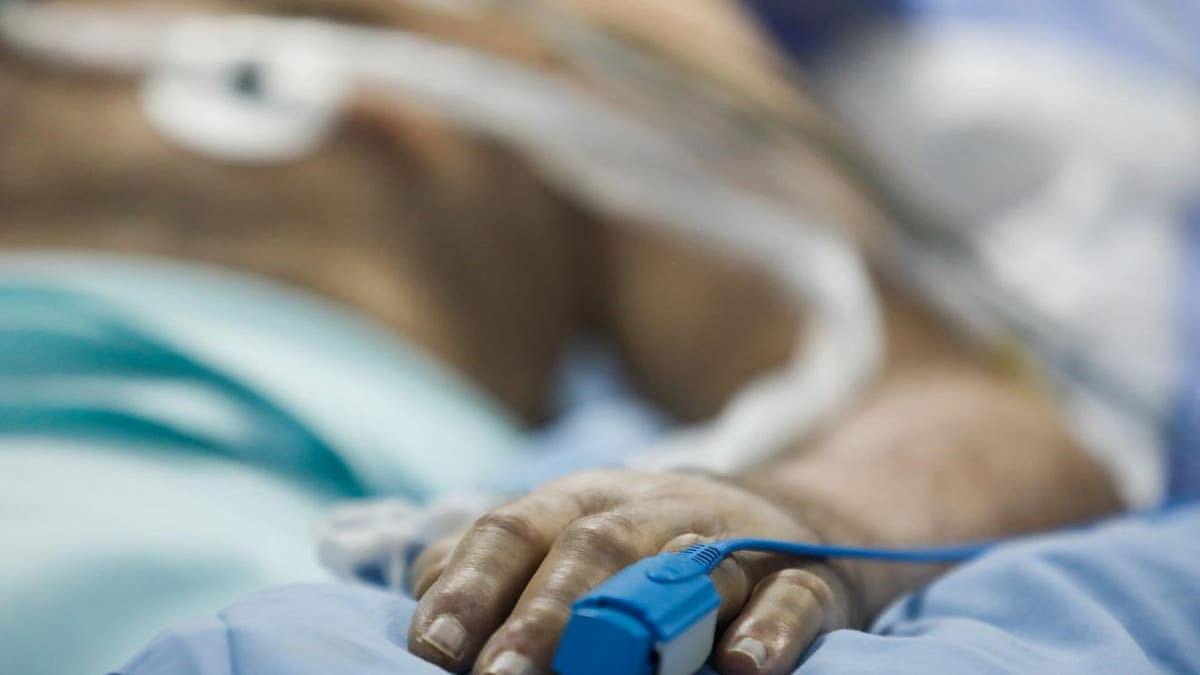
A pulse oximeter is seen above. (Reuters)
Silent hypoxia progressing rapidly to respiratory failure explains cases of COVID-19 patients dying suddenly despite not feeling short of breath.
As Levitan notes in his op-ed, one reason COVID-19 is putting a strain on our public health system is the severity of lung injury patients have when they arrive in emergency rooms. Unfortunately, many patients aren't arriving in hospitals until their condition has already worsened, and then they often need to be put on ventilators.
That can lead to a shortage of those machines -- and doctors having to make untenable decisions about rationing of care.
"There is a way we could identify more patients who have Covid pneumonia sooner and treat them more effectively — and it would not require waiting for a coronavirus test at a hospital or doctor’s office," Levitan writes in the Times. "It requires detecting silent hypoxia early through a common medical device that can be purchased without a prescription at most pharmacies: a pulse oximeter."
Pulse oximeters, which are carried by most EMTs, are small devices placed on a person's fingertip; with the press of a button, they display oxygen saturation and pulse rate.
CORONAVIRUS HAS MUTATED INTO AT LEAST 30 DIFFERENT STRAINS, STUDY FINDS
According to Levitan, the small devices saved the lives of two physicians he knows.
"Widespread pulse oximetry screening for Covid pneumonia — whether people check themselves on home devices or go to clinics or doctors’ offices — could provide an early warning system for the kinds of breathing problems associated with Covid pneumonia," the doctor writes.