(iStock)
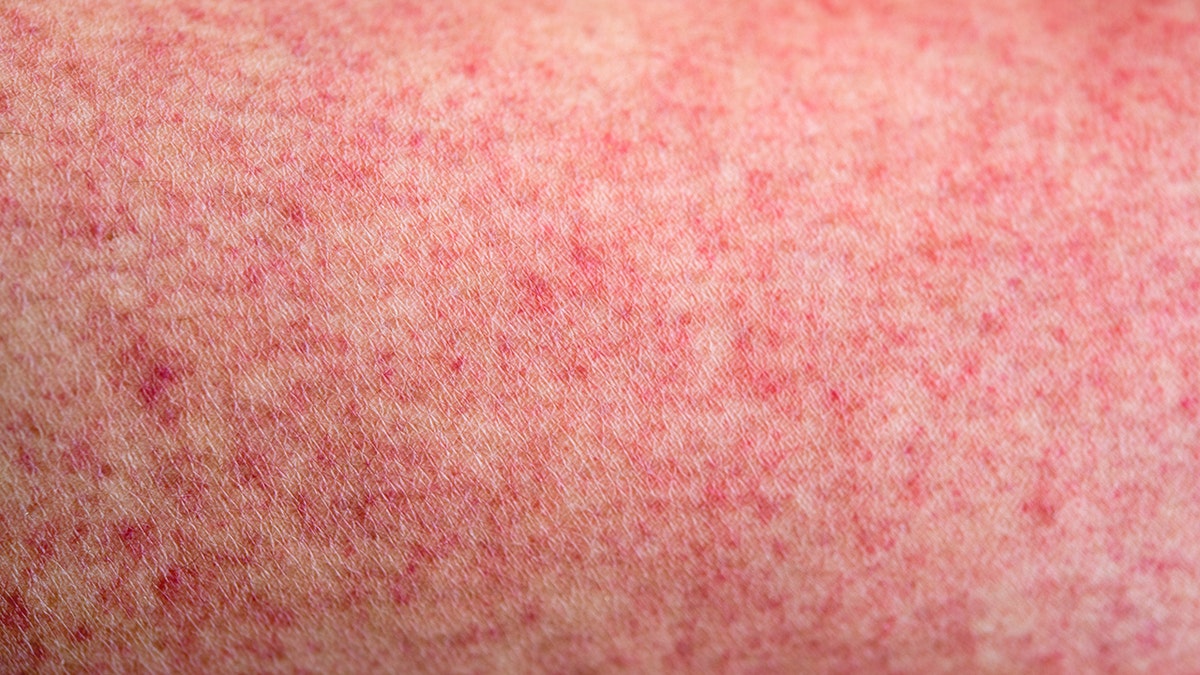
Numerous reports of skin rashes in patients with COVID-19 are cropping up around the world.
The rashes can take many forms — some appear as tiny red spots, while others appear as larger flat or raised lesions. Some have a hive-like appearance, while others look like frostbitten toes.
However, it's too early to say whether these rashes are indeed caused by the new coronavirus, or whether they are related to other factors. "That's really the million dollar question," said Dr. Kanade Shinkai, a professor of dermatology at the University of California, San Francisco, and editor-in-chief of the journal JAMA Dermatology.
"It's unclear whether the skin lesions we see in COVID are actually a direct manifestation of the virus" in the skin, or whether they are a "reaction pattern" due to a generally ramped-up immune system, Shinkai told Live Science.
Related: What are symptoms of the coronavirus?
It's also possible some rashes are due to complications from the disease, reactions to medications or even due to other viruses in patients with "co-infections," Shinkai and colleagues wrote in an editorial published April 30 in the journal JAMA Dermatology.
Social media posts and online forum discussions have called attention to these rashes, but "it is now time for rigorous science," the authors wrote. Work is needed to address many unanswered questions, such as how common the rashes are, and what they mean with regard to the patients' ultimate outcomes.
How common are these rashes?
It's well known that some viral illnesses, such as chickenpox, measles and hand, foot and mouth disease, can cause rashes. But virus-related rashes are more typically seen in children, Shinkai said. "That's why it's much more striking" to see numerous reports of rashes in adult patients with COVID-19, she said.
Exactly how common the rashes are remains unclear. In one early study of more than 1,000 COVID-19 patients in China, published Feb. 28 in the New England Journal of Medicine, rashes were noted in only 0.2% of patients. However, in a more recent study of about 150 hospitalized COVID-19 patients in Italy, rashes were found in 20% of patients. The latter study, published March 26 in the Journal of the European Academy of Dermatology and Venereology, was conducted by dermatologists, who "are going to be able to detect more subtle skin changes" than doctors in other specialities, Shinkai said.
More studies are needed that follow patients over a period of time to get a better idea of the true prevalence of rashes tied to COVID-19, Shinkai said. Still, one challenge to this is that some patients may have mild or no other symptoms of disease, and may never be diagnosed with COVID-19, she said.
What do the rashes look like?
Distinct rashes can sometimes be a "telltale sign" of a particular infection. Whether this will be the case for COVID-19 patients remains to be seen, the JAMA editorial said.
So far, a variety of rashes have been noted in COVID-19 patients. A Spanish study published April 29 in the British Journal of Dermatology grouped coronavirus-related rashes into five categories: a "maculopapular" rash, or one that's characteristic of viral infections such as measles, with red bumps on reddish skin; a "urticaria" rash characteristic of hives; a 'livedo" rash with a lace-like or fishnet pattern; a "vesicular eruption" or blistering rash; and a frostbite-like rash on the toes, unofficially dubbed "covid toes."
In addition, one recent case report published April 30 in JAMA Dermatology described the case of a man in Spain who developed "petechiae," or tiny red dots on the skin; and a separate case report, also published in JAMA Dermatology, described a patient in France who developed larger lesions known as a "digitate papulosquamous eruption."
The timing of rash symptoms with COVID-19 also seems to vary widely — in some cases, rashes precede symptoms such as fever; in other cases, rashes may appear a few days into the illness or not show up until late in the course of the infection.
Related: 13 coronavirus myths busted by science
Unanswered questions
Research is needed to comprehensively evaluate these rashes and when they occur, Shinkai said. Doctors will also need to examine tissue samples to determine if the virus that causes COVID-19, known as SARS-CoV-2, can be detected in the skin itself, which is the case for some viral illnesses that cause rashes, Shinkai said.
In addition, the significance of these rashes — such as whether they are tied to better or worse outcomes for patients — should also be studied, she said. For example, some patients with covid toes have been reported to have mild or asymptomatic cases of COVID-19, Live Science previously reported.
To help doctors learn more about COVID-19 and rashes, a task force with the American Academy of Dermatology has created an online COVID-19 dermatology registry, where health care providers can report skin findings linked to the disease, Live Science previously reported.
- The 12 deadliest viruses on Earth
- 20 of the worst epidemics and pandemics in history
- 11 (sometimes) deadly diseases that hopped across species
Originally published on Live Science.







































