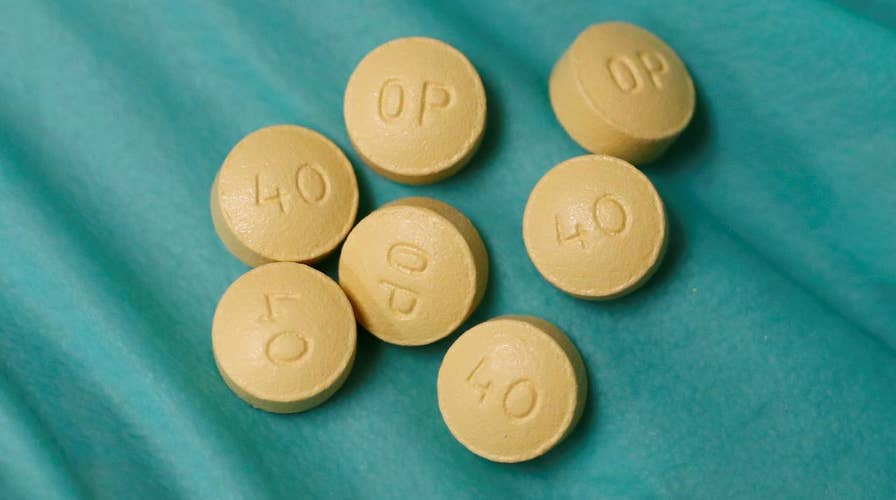
President Trump pledges action on opioid epidemic
Administration hosts summit of wide array of people determined to do something about the crisis; Kevin Corke reports from the White House.
The stories and headlines are far too common these days, featuring individuals, families and communities devastated by opioid addiction. But with more than 100 Americans dying each day from opioid overdoses – in every city and town across the nation – it’s hard to find someone who hasn’t been personally impacted by this epidemic.
Unfortunately, new federal Centers for Diseases Control and Prevention (CDC) data reveal that opioid overdoses continue to increase among men and women, most age groups, across all regions and in most states.
CDC’s latest Vital Signs report found that in just over a year, emergency department visits for suspected opioid overdoses increased 30 percent in all parts of the U.S. The most dramatic increase was in the Midwest, which saw a 70 percent jump in opioid overdoses.
In addition, our report revealed rate increases in every demographic group, including: men (30 percent); women (24 percent); people between the ages of 25 and 34 (31 percent); 35- to 54-year-olds (36 percent); and those 55 and older (32 percent).
And the increases weren’t limited to small towns or rural areas. Opioid overdoses in large metropolitan areas rose by 54 percent.
These statistics are a clear signal that America’s complex and fast-moving opioid overdose epidemic isn’t slowing down anytime soon. However, our Vital Signs report also highlights some opportunities for progress, and reveals how timely data can potentially save some lives.
Although CDC typically analyzes deaths from opioids, this report looked at recent emergency department visits for suspected opioid overdoses, most of which were nonfatal.
Research shows that people who have had at least one overdose are more likely to have another – and if that person is seen in the emergency room, we all have the opportunity to prevent a repeat overdose.
Data from emergency departments can be used as a warning system – sending us a wakeup call about the need to improve what happens when patients leave the emergency department, including linking them to mental health services and medication-assisted treatment. The sharp increases and variation seen in this report across regions and states point to the need for better coordination for regional or multiple state outbreaks.
So how can we use this information to prevent opioid overdoses and deaths? Communities, law enforcement, the medical community, public health and government must all work together.
? Health departments can alert communities to rapid increases in overdose data so they can plan an effective and timely response. For example, health departments can work to increase the distribution of naloxone, an overdose-reversing drug, in affected communities. They can also support the CDC Guideline for Prescribing Opioids for Chronic Pain, which recommends using prescription drug monitoring programs to inform clinical practice.
? Local emergency departments can develop plans for all opioid overdose patients, including offering overdose prevention education, naloxone and related training for patients, family members and friends. They can also link patients to the appropriate follow-up treatment and services.
? Public safety and law enforcement can quickly identify changes in the illicit drug supply of an area, and coordinate responses with local partners, like public health departments.
? Community-based organizations can help mobilize response for those most at risk, such as supporting programs that offer screening for HIV and Hepatitis B and C, along with referral to treatment.
? And finally, families, friends and neighbors of those who use opioids can help support them in treatment and counseling, and learn about the signs and risks of opioid use.
We know this will not be easy. We’re now seeing the highest drug overdose death rates ever recorded in the U.S., driven by prescription opioids and illegal opioids such as heroin and illicitly manufactured fentanyl.
As a doctor, I’m familiar with the complexities of pain management, and I’ve seen the devastating impact that opioid addiction can have on individuals, families and communities.
As a public health leader, I recognize the importance of data in planning treatment and prevention efforts. Having the right data available at the right time can help direct the right resources to the most impacted areas.
This epidemic does not distinguish by age, sex, or state and county lines, and it shows that we still have a lot of work to do to protect Americans from the dangers of opioids. But working together, we can fight this crisis and save lives.