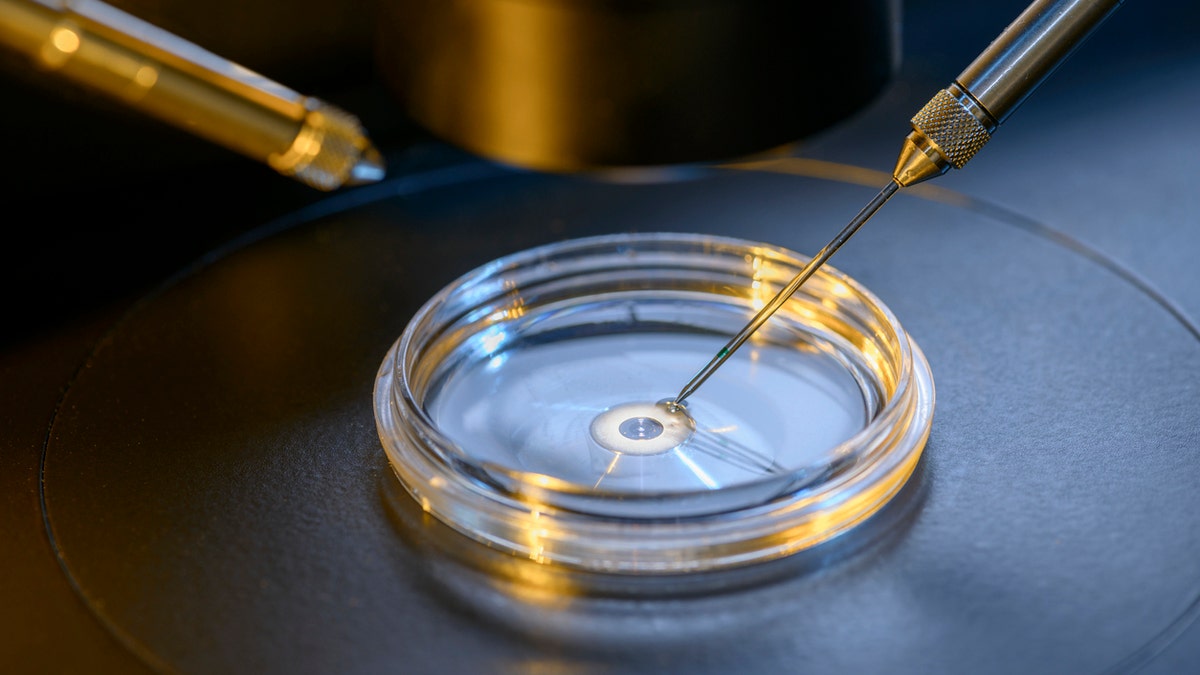
An estimated 8 million babies have been born from IVF worldwide since 1978, according to a report. (iStock)
In her soon-to-be-released memoir, former First Lady Michelle Obama revealed she and former President Barack Obama used in vitro fertilization (IVF) to conceive their two daughters, Malia, 20, and Sasha, 17.
The 54-year-old revealed that she had a miscarriage prior to conceiving Malia, an experience she said “left her physically uncomfortable and cratered any optimism we felt."
"I felt like I failed because I didn't know how common miscarriages were because we don't talk about them," the former first lady said in an interview broadcast Friday on ABC's "Good Morning America." ''We sit in our own pain, thinking that somehow we're broken."
More than 8 million babies have been born from IVF worldwide since 1978, the European Society of Human Reproduction and Embryology estimated in July.
Read on to learn more about IVF.
What is it and why may some people choose IVF?
IVF is a process where a woman’s eggs are extracted and then combined with sperm in a laboratory dish, according to the American Pregnancy Association. From there, the fertilized egg (or sometimes multiple eggs) are placed in a woman’s uterus.
One IVF cycle — which includes “ovulation induction,” “egg retrieval,” “sperm retrieval,” “fertilization” and finally the transfer of the embryo into the uterus, according to the Mayo Clinic — takes roughly two weeks, though it's possible another cycle will be necessary.
CONJOINED TWINS SUCCESSFULLY SEPARATED IN 6-HOUR SURGERY
Donated eggs, sperm, and embryos are sometimes used during IVF, depending on the individual’s or couple’s needs.
Women over 40 years of age are typically offered IVF as a "primary treatment," the Mayo Clinic says. Patients may choose IVF if they or their partner has a certain medical condition.
For instance, IVF may be an option for women who have fallopian tube damage or blockage, an ovulation disorder, endometriosis or premature ovulation failure, among other conditions, according to the Mayo Clinic. IVF may also be an option for men who have impaired sperm production or function.
How successful is it?
The process, which the American Pregnancy Association notes is an “assisted reproductive technology (ART),” is the “most effective form” of ART, according to the Mayo Clinic. But the success of IVF depends on multiple factors, such as a woman’s age and cause of infertility.
Women under the age of 35 who use “fresh embryos from non-donor eggs” have a 21.3 percent chance of having a “full term, normal birth weight and singleton live birth per ART cycle,” according to Penn Medicine, which cited a 2015 U.S. Society of Assisted Reproductive Technology report.
After 35 years of age, a woman’s chances continue to decrease.
What are the risks?
According to the Mayo Clinic, IVF increases the risk of “multiple births if more than one embryo is implanted in your uterus,” and a “pregnancy with multiple fetuses carry a higher risk of early labor and low birth weight than pregnancy with a single fetus does.”
IVF can slightly increase the chance of delivering a baby prematurely, while the chance of miscarriage increases by a small amount if a woman uses a frozen embryo and not a fresh embryo.
MOM LOOKING TO SWAP GIRL EMBRYO FOR A BOY GETS OFFERS FROM AROUND THE GLOBE
Birth defects and ectopic pregnancy — when a fertilized egg attaches outside of the uterus — are also risks. The Mayo Clinic states roughly 2 to 5 percent of women using IVF have an ectopic pregnancy.
You can learn more about potential uncertainties here and side effects of IVF here.
What’s the cost?
IVF can be costly — typically costing thousands of dollars for every "cycle," and many couples require more than one attempt.
Penn Medicine estimated the average cost of “a single IVF cycle” ranges between $10,000 and $15,000, though the price is “dependent upon insurance coverage, patient characteristics and the treatment center.”
The Associated Press contributed to this report.







































