Researchers at Cincinnati Children’s Hospital Medical Center have discovered a new gene and cell therapy that could treat a rare lung disease in children.
In the study, published in the journal Nature, researchers found that transplanting pulmonary macrophages— immune cells— into the lungs of mice corrected hereditary pulmonary alveolar proteinosis (hPAP).
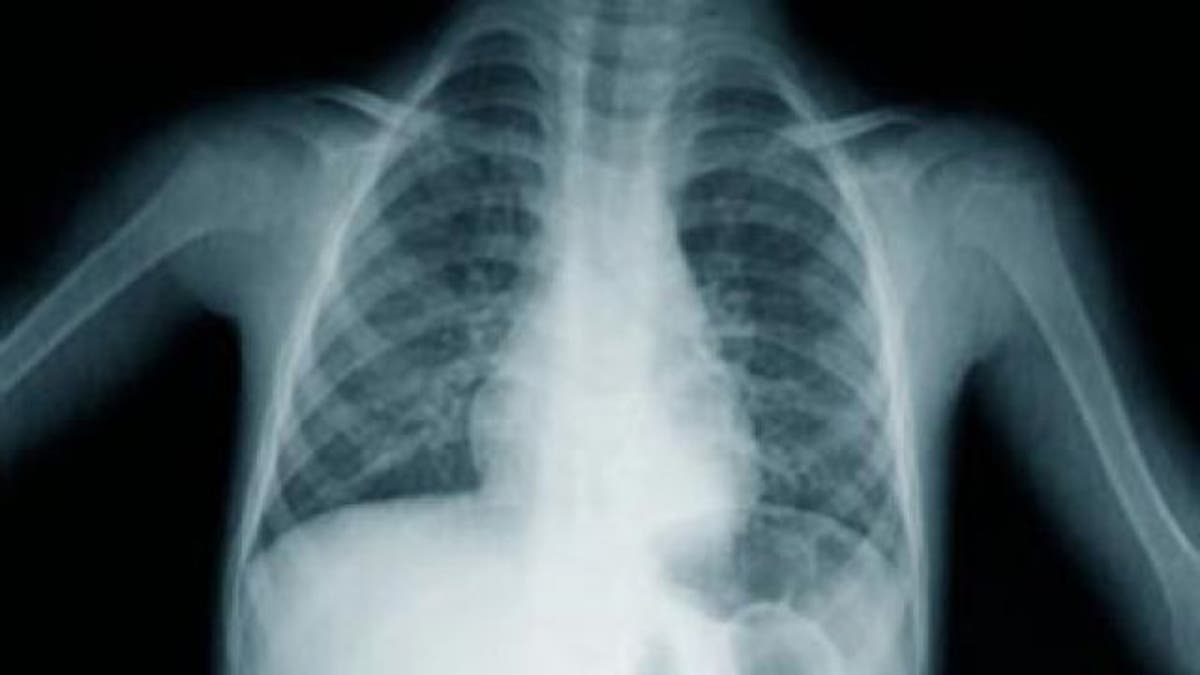
The lung disease is caused by a build-up of surfactant, an oily substance in the air sacs of the lungs, which results in reduced lung function and eventually failure. The condition is the opposite of a common condition in premature babies, whose lungs are at a higher risk of collapsing because their air sacs will not stay open. Children with hPAP, on the other hand, have such high levels of surfactants that the children’s air sacs overinflate, and they drown internally as a result.
Between 2,000 and 3,000 children in the U.S. have hPAP, senior study author Bruce Trapnell, a physician in the division of neonatology and pulmonary biology at Cincinnati Children's Hospital Medical Center, told FoxNews.com.
The only available therapy for the rare disease— whole-lung lavage— is a difficult procedure that’s invasive, requires anesthesia and involves mechanical ventilation, Trapnell said. For the surgery, doctors must attach a breathing tube to one lung and fill the other with salt water. A few days later, the procedure is repeated on the opposite lung.
“It’s like trying to wash butter out of a sponge by squirting it with a garden hose,” Trapnell said.
Searching for a different type of therapy, researchers studied transplantation of naturally healthy macrophages or gene-corrected macrophages into the lungs of mice with hPAP. The therapy corrected the disease in mice for at least one year and prevented disease-related death.
Researchers are planning clinical trials of macrophage transplantation, but they noted that questions remain. Previous research using bone marrow transplantation was successful in animal models, but failed in human trials.
“We have to address how many cells to transfer, and how the human body processes these cells," study co-author Takuji Suzuki, a scientist in the division of neonatology and pulmonary biology at Cincinnati Children’s, told FoxNews.com.
Researchers hope to begin the clinical health study in two to three years.