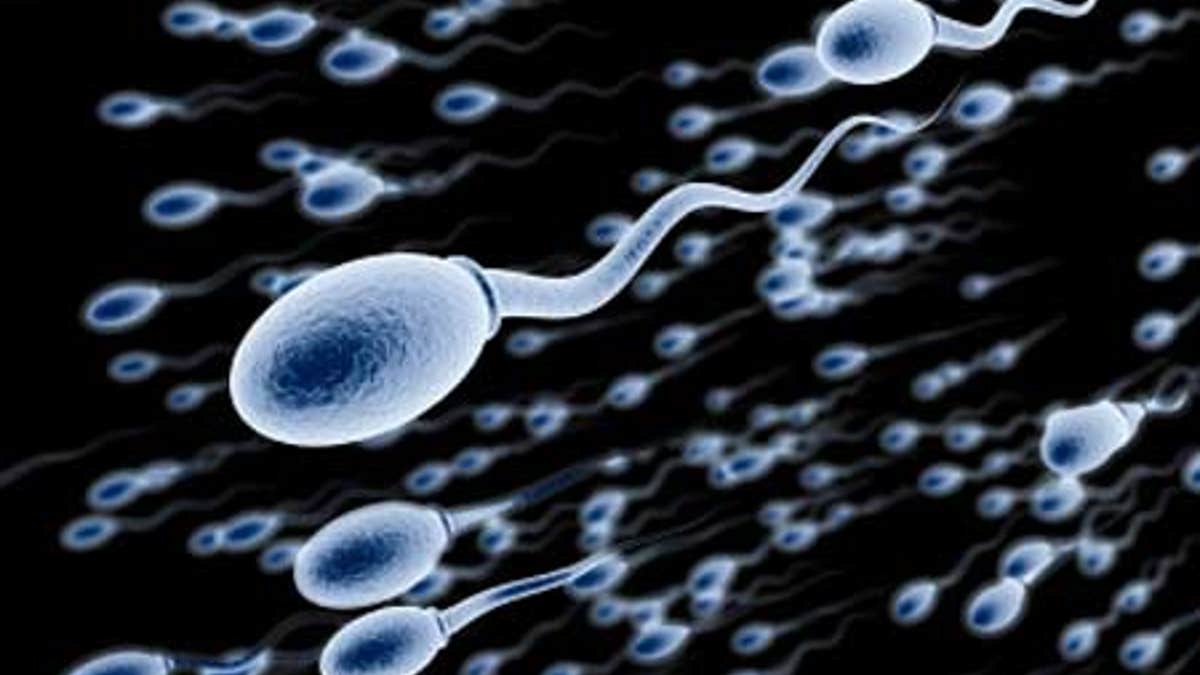
Researchers at Stanford University have sequenced the entire genomes of 91 human sperm from a single man – providing insight into the genetic variation that naturally occurs in a single individual.
The project marks the first time the whole-genome of a human gamete has been sequenced.
Published in the journal Cell, the study offers more detailed knowledge about the process of genetic recombination – the method in which DNA from both a mother and a father blend together in the children they produce. Recombination facilitates both the breaking apart and rejoining of chromosomes during reproduction.
“We learned some really interesting details about how the body mixes together the genomes from parents to create new genomes for their potential children,” said Steve Quake, professor of bioengineering and applied physics at Stanford University as well as the study’s lead author. “That’s why every sperm cell has a different genome. Your body mixes to create unique genomes so your offspring have different genetic diversity.”
Providing greater detail
Quake and his colleagues isolated and sequenced nearly 100 sperm cells from a 40-year-old man with healthy children. They compared the sperm sequences with the man’s whole-genome sequence, ultimately allowing them to identify where and when recombination took place.
Until this sequencing project, scientists could only rely on genetic studies of population to estimate how often recombination occurred in sperm and egg cells as well as the amount of genetic mixing the process needed.
The Stanford study essentially confirmed what these previous studies theorized: Each sperm in the sample underwent 23 recombination events, or mixing events. However, the study also showed that the degree of genetic mixing varied greatly between individual sperm, as well as the frequency and severity of spontaneous genetic mutations. According to the researchers, the sequencing technique used in their study can provide a better guide as to what exactly happens during a sperm’s development.
“[Before this study], we have no way to catalogue the mutations and the recombination events of an individual,” co-author Barry Behr, professor of obstetrics and gynecology and director of Stanford’s in vitro fertilization laboratory, told FoxNews.com. “Once we get our understanding of these, we can map them and see how they change as a man ages. We could map these in healthy versus unhealthy people. We could map these in fertile and infertile people, and really get a better understanding as to what the fundamental makeup of a good sperm versus a bad sperm is.”
Understanding infertility
The majority of cells in the human body carry two copies of each of 23 chromosomes. Recombination occurs during meiosis – a type of cell division necessary for reproduction in which one copy of each chromosome is separated into a sperm (for men) or an egg (for women). This ensures that when a sperm fertilizes an egg, the resulting embryo has a full set of matching DNA.
However, when the pairs of chromosomes align during recombination, sometimes portions of matching chromosomes are randomly swapped out – what is known as genetic mixing. This process allows for much more genetic variation in potential children. According to Behr and Quake’s research, the degree and frequency of this genetic mixing was unique for each sperm and egg cell.
The sequencing technique revealed that spontaneous genetic mutations – variability in sperm that happens randomly – varied greatly in between individual cells as well.
“We discovered that measuring the rate at which new mutations form in sperm is somewhat higher than we expected,” Quake said. “It presents a nifty puzzle for us to solve…. We’re now in position to use this technique to work out what is the truth between new mutation rates in between individuals.”
While genetic mutations can also be responsible for genetic variation in offspring , if they occur at particular points in the genome, adverse effects can occur. According to Behr, this insight into mutation rates could potentially be used to get a better understanding of male infertility in the future.
“I would put money on the fact that we or others will be able to demonstrate using our approaches that infertile men have higher mutation rates or have different types of mutation rates than those men who have normal fertility rates,” Behr said. “That in and of itself will be a huge contribution to understanding fertility, but specifically male fertility, which is really a decade or two behind studying female fertility.”
Behr also noted that each individual cell is destroyed by the sequencing process, so the sperm they studied could not go on to fertilize eggs. However, Behr said that having such intricate knowledge of just a few sperm from a sample could provide a good snapshot of a man’s overall sperm trends.
“I anticipate as technology proceeds, we may be able to find information out about individual sperm cells and then use them,” Behr said. “But currently what we’re able to do, which I think is valid, is that we can look at maybe a subset of the whole sperm population and make a very accurate determination on the compliment or the characteristics of that sample.”