Emergency Medical Services struggle to stay afloat amid pandemic
In addition to the mental and physical toll the virus is taking on these men and women, prices of certain PPE materials has more than tripled, striking the EMS industry with a major financial blow.
DALLAS, Texas – The coronavirus pandemic has strained the country's hospital systems and pushed front-line workers mentally and physically as the number of cases spikes upward again. Some agencies dealing with budget issues due to demand in personal protective equipment (PPE) and an uptick in calls have been forced to shutter, begging the question of who will respond in the event of an emergency?
Ryan Snow, a paramedic and firefighter with the Dallas Fire and Rescue in Texas has been working on the front lines since the beginning of the coronavirus pandemic.
“Initially there was obviously a fear factor when responding to COVID calls because there was that unknown factor,” Snow told Fox News. “Making that transition to pre-COVID to actually working in COVID conditions is very difficult because you are not able to leave work at work.”

Snow has been helping COVID-19 patients since the pandemic began.
The father of two said nine months into the pandemic, the work is taking a mental toll on him and others in the field.
FDA TO MEET ON PFIZER'S CORONAVIRUS VACCINE EUA APPLICATION: WHAT TO EXPECT
“Mentally, just trying to work through being able to function on a high level, knowing there are people suffering and everything is going to hell in a handbasket around you and still trying to be the best that you can be,” Snow said.
The workflow for most people has changed, and that includes paramedics who now respond to every call as if it is a COVID-19 call.
“Our overall run volume hasn’t actually changed that dramatically, but the makeup of the calls is where we have seen the differences,” Tami Kayea, Dallas Fire and Rescue Deputy Chief over EMS, said. “When you had a lull in the numbers of COVID-19 cases, you had a lower number of patients we assumed to be COVID-positive and when the cases were higher, the number of patients that had COVID-19 were higher.”
Gearing up for response has also changed the way the crew manages calls.
“Originally it was just like wear a mask and when you get there, assess if it is COVID or not, but now, you basically assume everybody is positive for COVID and everyone will need to be wearing a mask, gloves, gowns and goggles every time," Kayea said.
It's also not clear as to when paramedics will be able to receive the much-anticipated coronavirus vaccine, and may vary state-by-state. Dallas Fire and Rescue has already sent a request to include paramedics in the first round of distribution.

Invoice from Medstar in Fort Worth, Texas shows PPE material cost skyrocketing.
In addition to the mental and physical toll the virus is taking on first responders, prices of certain PPE materials have more than tripled, striking the EMS industry with a major financial blow.
Matt Zavadsky, director of Medstar and president of the National Association of Emergency Medical Technicians, said the cost of N-95 masks alone has skyrocketed.
FAUCI SAYS BUILDING CORONAVIRUS VACCINE TRUST ESSENTIAL: 'WE HAVE A TASK CUT OUT FOR US'
“We used an average of six N-95 masks per day and they cost us 67 cents. Today, we are using an average of 200 per day and they are costing us $3.50,” Zavadsky said.
Zavadsky added that the strain could result in delayed responses to calls and for some providers, it could mean going out of business.
“EMS agencies are already closing, nationally we know there are agencies that are just unable to weather this storm,” Zavadsky said. “One of the things that we have always been fearful of is, what if you call EMS and nobody comes? In some of these communities where agencies are having to close because they don’t have the personnel, they don’t have the funding and they can’t afford to operate anymore, that is beginning to happen.”
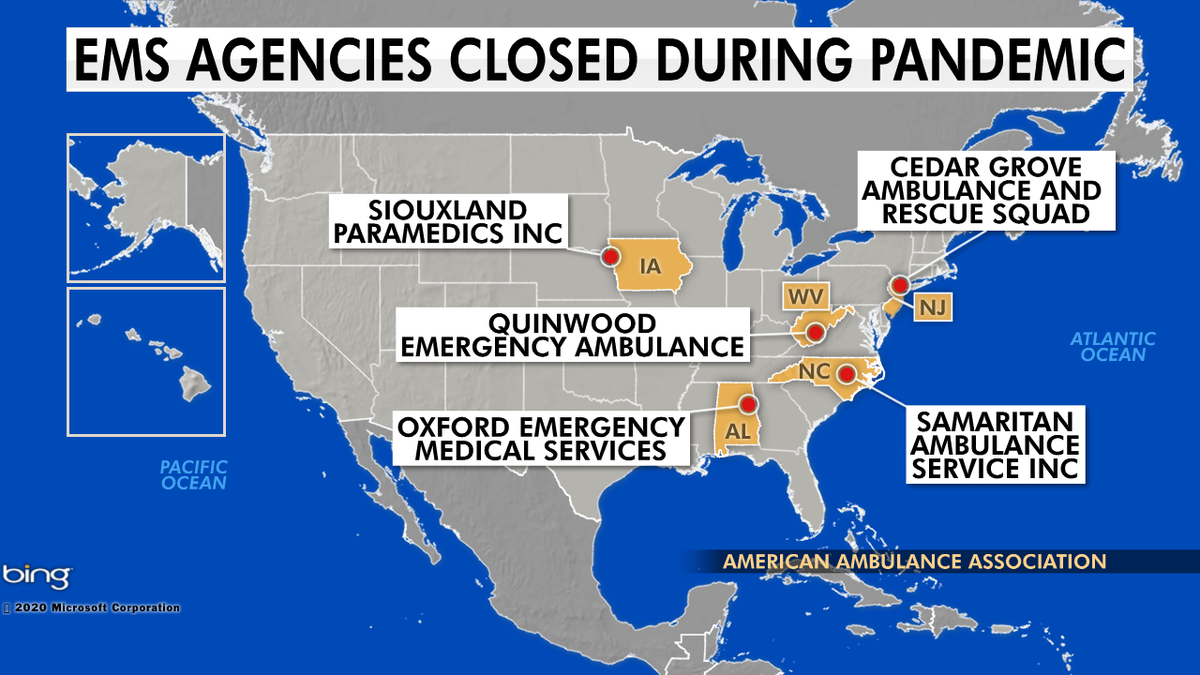
The American Ambulance Association reached is working to secure fund for EMS agencies across the country.
The American Ambulance Association reports at least six services have closed, and it’s trying to get more funding to keep others open.
CLICK HERE FOR COMPLETE CORONAVIRUS COVERAGE
The non-profit sent a letter to the Department of Health and Human Services asking for $2.6-billion in emergency funding. The letter said that across the country, EMS is at a “breaking point.”
If funding is received, it would be available for any agency with operating ambulances.









































