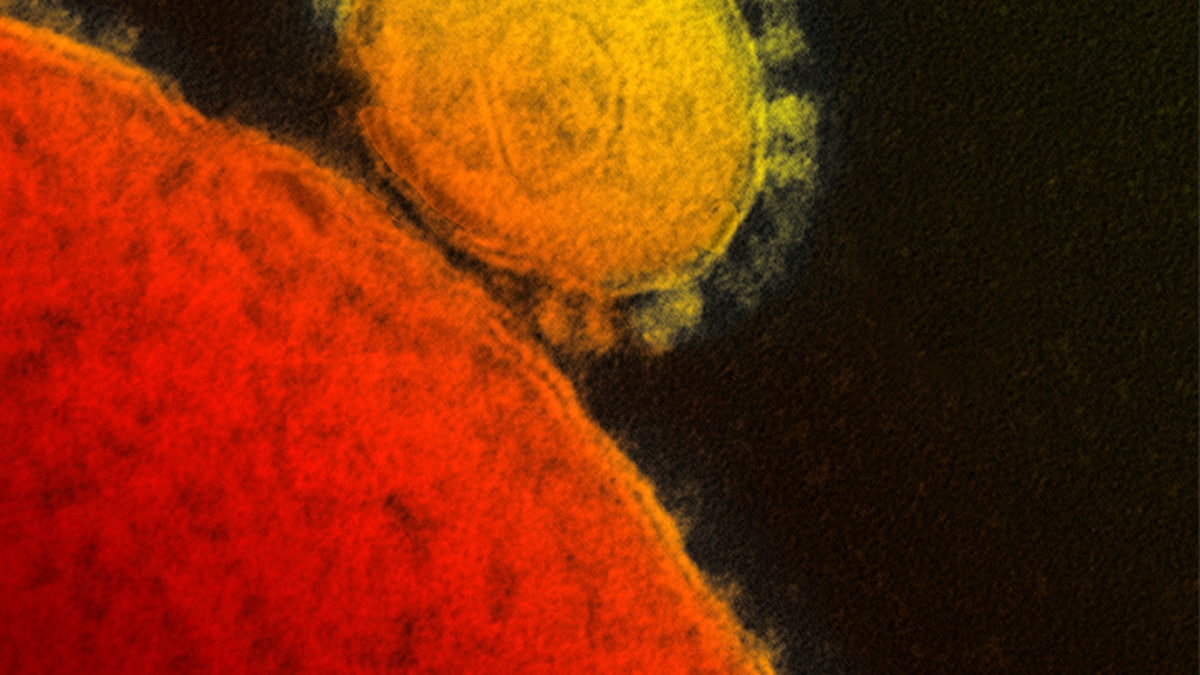
This undated electron microscope image shows a novel coronavirus particle, also known as the MERS virus, center. (AP Photo/NIAID - RML)
As the deadly MERS virus continues to infect people throughout the Middle East and Europe, the Centers for Disease Control and Prevention (CDC) has begun to prepare for the disease’s potential spread to the United States.
Currently, the U.S. has had no confirmed cases of the MERS virus, a respiratory infection that researchers say is similar to SARS – though more deadly.
More than 60 cases of MERS, including 38 deaths, have been recorded by the World Health Organization in the past year. Though most cases have appeared in Saudi Arabia, the virus has also been reported in Jordan, Qatar, the United Arab Emirates, Britain, France, Germany, Italy and Tunisia.
Currently, the CDC says that the risk of the virus appearing in the U.S. is low – but still present.
“We know that the experience in Europe says the risk is not zero,” Dr. Mark Pallansch, director of the CDC’s division of viral diseases, told FoxNews.com. “They’ve had at least four events of importing the virus in a traveler from (the Middle East). Since their travel volume is much higher with that region than ours, that would make sense in terms of us not having had a case, but still tells us the risk is not zero.”
As a result, the CDC is taking a three-pronged approach to prepare for MERS.
According to Pallansch, the CDC has already begun equipping hospitals with tools that will allow them to rapidly detect and report instances of the virus.
“The CDC has prepared diagnostic kits, these are being distributed to the states,” Pallansch said. “There are more than 40 states now that have these kits.”
If MERS were to be detected in a U.S. hospital, the CDC would then confirm the presence of the virus, and the hospital would simultaneously begin to prepare to contain the spread of the disease.
“We would be reinforcing messages about infection control in the hospital setting and setting up surveillance in hospitals for workers but also…family, coworkers, community exposures that might potentially be there,” Pallansch said.
Pallansch noted that current research on MERS indicates an absence of sustained community transmission – meaning the virus isn’t spreading from person to person outside of hospital settings. However, cases of the virus spreading from person to person within hospital settings have been reported.
“We’re highly concerned, as with SARS, that spread within the hospital is a risk, so we’re trying to update advice and guidance for hospitals in case they are in that situation,” Pallansch said.
Additionally, the CDC is preparing a strategy for communicating information about the disease at the hospital, local, state and government levels.
“At the moment, we’re not monitoring travelers, but we are encouraging physicians who have sick patients to ask about a travel history, specifically to the four countries affected so far in the Middle East,” Pallansch said.
The CDC has also posted signs in some airports, warning travelers to watch out for signs of the disease.
“Fourteen days is the interval of time, is the period of concern,” Pallansch said. “Right now (symptoms include) fever, cough, shortness of breath, anything people would be concerned about in terms of ability to breathe.”
So far, illnesses haven't spread as quickly as SARS did in 2003 when it triggered a global outbreak that killed about 800 people. However, the disease so far appears to be more deadly than SARS, according to researchers.
“The severity for MERS appears to be much higher – 50 to 60 percent of known infections have resulted in death. This is significantly higher than SARS,” Pallansch said.
Pallansch noted that it is hard to say how wide of an impact the MERS virus will have – which is why the CDC continues to work on preparedness.
“The major challenge we have at the moment is inadequate information about a lot of the cases,” Pallansch said.
The Associated Press contributed to this report.







































