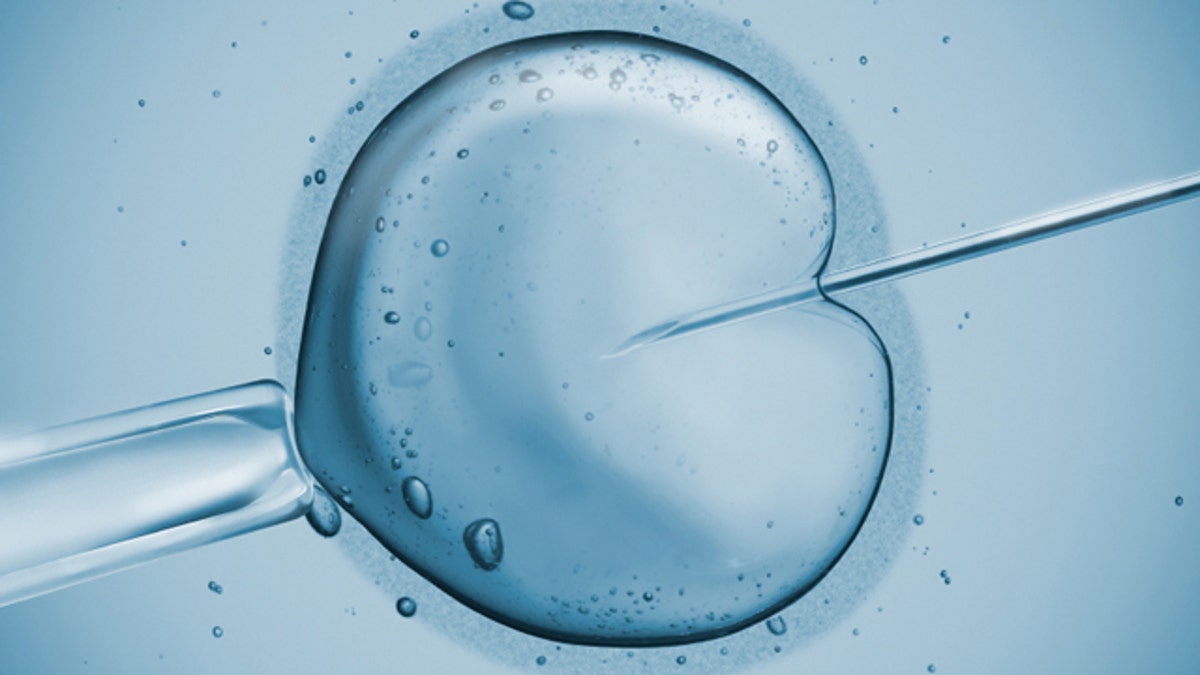
When it comes to infertility, most people immediately think about in-vitro fertilization (IVF), but there’s a lesser-known fertility treatment that is used along with IVF. It’s called ICSI (pronounced ik-see) or intracytoplasmic sperm injection.
Although ICSI has been around since the early 1990s, it’s increasingly being used to help couples struggling with infertility. And as with any new technology, some experts have concerns about its overuse as well as how it may affect the health of the babies born to it.
Here, find out what ICSI is, who the best candidates are, and what you should consider before opting for treatment.
What is ICSI?
Unlike conventional fertilization, whereapproximately 30,000 sperm are dropped onto the egg in a Petri dish, during ICSI, a single sperm is injected into the egg in order to improve the chances of fertilization.
“It has allowed many couples to have children who otherwise wouldn’t be able to,” said Dr. Thomas Molinaro, a reproductive endocrinologist at Reproductive Medicine Associates of New Jersey in Eatontown.
According to the American Society for Reproductive Medicine (ASRM), 50 to 80 percent of eggs are fertilized using ICSI.
ICSI is primarily indicated for men with male factor infertility, which accounts for up to one-third of infertility cases. Male factor infertility problems include low sperm count and issues withmotility (movement), or morphology (shape) of the sperm. Men may also use ICSI if they don’t have sperm in their ejaculate either because of a production problem or a blockage. Their sperm would then be extracted from the testicle. ICSI can also help men who had a vasectomy or who were born without a vas deferens.
“For those indications, ICSI is much better than doing regular IVF,” said Dr. Philip Werthman, a urologist and director of the Center for Male Reproductive Medicine and Vasectomy Reversal in Los Angeles, Calif.
ICSI can also help couples that attempted IVF but had what’s known as “failed fertilization.”
Failed fertilization happens when more than one sperm fertilizes the egg which makes the embryo unusable, or when the sperm is unsuccessful at fertilizing the egg.
If no fertilization occurs after 12 hours of the incubation period, a “rescue ICSI” can be used but it’s usually unsuccessful, too.
“For the most part, it’s rare that we have good outcomes after failed fertilization,” Molinaro said.
ICSI is also used when couples opt for pre-implantation genetic testing (PGD), which screens embryos for chromosomal abnormalities or genetic conditions.
When conventional fertilization is used, many sperm bind to the egg and their DNA remains on the surface of the embryo.
“When we biopsy the embryo for testing, this residual sperm can create interference which affects the fidelity of the testing. Using ICSI removes this contamination and results in better accuracy,” Molinaro said.
Success rates for ICSI are similar to IVF alone. When looking at ICSI for male factor infertility, the percentage of cycles that resulted in a live birth were about the same as those cycles who didn’t use ICSI and had no diagnosis of male factor infertility, a report by the Centers for Disease Control and Prevention (CDC) found.
Like all fertility treatments, ICSI is not perfect.
There is growing concern in the medical community about ICSI. Namely, about its overuse and the potential problems it may cause down the line.
In fact, a recent report in the Journal of the American Medical Association found that fresh IVF cycles using ICSI increased from 36.4 percent in 1996 to 76.2 percent in 2012 and the largest increase was when male factor infertility was not present. Plus, there was no association with better outcomes whether male factor infertility was present or not.
“If the sperm aren’t healthy enough to travel to penetrate the egg, there is some issue there that goes beyond just that one task,” Bridgit Danner, a licensed acupuncturist specializing in holistic fertility in Portland, Ore. said.
ICSI is also associated with a slightly higher risk for birth defects and chromosomal abnormalities. In fact, a study in the journal Fertility and Sterility found that more boys conceived using ICSI were found to have undescended testes.
Another study in the New England Journal of Medicine found a 9.9 percent risk of birth defects using ICSI, compared to 7.2 percent using IVF. Compared to natural birth, birth defects were 77 more likely with ICSI and 26 percent more likely with IVF.
There is also some concern that ICSI could affect how the genes are expressed.
“Maybe it’s not going to be the gross abnormality that couldn’t produce the healthy child but maybe there will be some subtler things in that child’s later fertility or learning ability, for example,” Danner said.
Experts caution that despite the data, the studies can’t control whether ICSI was done for male factor infertility or for other reasons. Plus, severe male factor infertility is a risk factor for the same problems.
“The question has always been and still sort of remains is: Is it ICSI itself which leads to this increased risk or is it the patient who needs ICSI?” Molinaro said.
“ICSI overcomes many sperm problems but it doesn’t overcome all problems,” Werthman said.
For example, men who have high levels of DNA fragmentation in their sperm can cause the egg to stop developing or not develop at all, or result in a miscarriage.
Another potential drawback and deal breaker for some couples is that there is no longer the same natural selection process of sperm that happens during traditional IVF.
“There’s always concern when we’re intervening at this level. But the great majority of data suggest that ICSI is a very safe procedure,” Molinaro said.
The future of fertility treatments.
There are techniques currently under development that may be able to examine and test sperm even more effectively so the best sperm can be selected. For now, however, “there is no real evidence that these techniques improve the success of ICSI,” Molinaro said.
Whether the choice is between ICSI and IVF, another treatment or none at all, it’s key to look at the reasons why infertility is present in the first place.
“The important thing for most couples is to realize that the sperm actually do play a very significant role in the fertility process,” Werthman said. “If someone has an abnormal semen analysis, the recommendations are that the man should get evaluated before they undergo any sort of fertility treatments.”
Plus, experts agree that optimizing both partners’ fertility with diet and lifestyle changes is important and may even make intervention unnecessary altogether.
“Both parties have to improve their health, especially if there are parameters that show there was a sperm quality issue,” Danner said.
“We have a lot of tools in our toolbox,” Werthman said. The most important thing is to use the most appropriate tool in the right situation.”








































