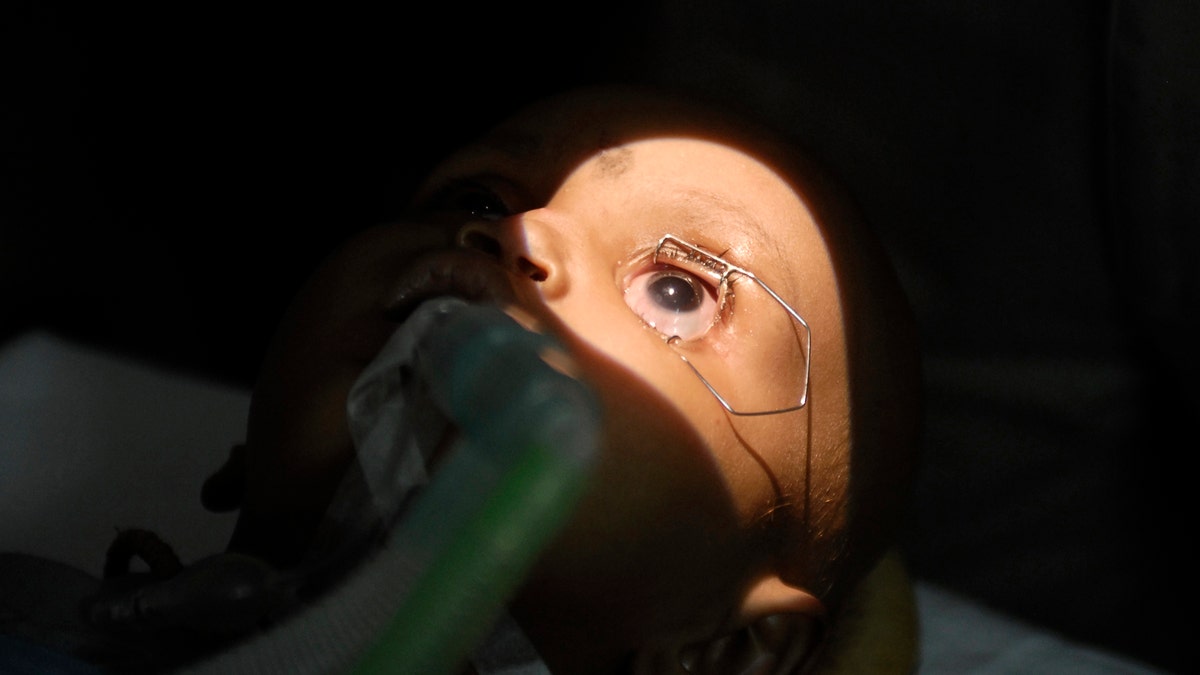
File photo - 15-month-old Tanishka has her eyes examined inside a operation theatre during a free treatment for poor patients to mark World Retinoblastoma Awareness week in the southern Indian city of Hyderabad May 12, 2010. Retinoblastoma is the most common primary ocular malignancy (eye cancer) of childhood, a doctor said. (REUTERS/Krishnendu Halder)
Product design and development firm Cambridge Consultants created a medical robot capable of performing one of the world's most common but delicate operations: cataract surgery.
Carried out around 20 million times per year, this life-changing surgery helps restore sight when a patient develops cataracts, turning their eye cloudy and making it hard for them to see. To counter this, surgeons slice a tiny hole in the eye's lens, remove the part which has clouded over and replace it with a plastic lens -- similar to a contact lens but inside, rather than outside, the eye.
While cataract surgery is common, however, things can and do go wrong. The lens being operated on is just 10mm across and -- while surgeons are necessarily steady-handed -- they are performing a 15-20-minute procedure on a tiny surface, using little more than tweezers and a microscope. Complications can include anything from a minor misalignment of the plastic lens to more serious issues like accidentally using the surgical instrument to pierce the back of the actual lens.
"The serious complications rate is fairly low, in the order of one percent, but when you're talking about one percent of 20 million that's still a ridiculously high number," Cambridge Consultants roboticist Chris Wagner told Digital Trends.
More From Digital Trends
Wagner led the project to create Axsis, a teleoperated robot which goes to work using dual arms equipped with miniature pincers. Although it is just a tech demo at present, should Axsis find its way into the operating theater, these pincers will be upgraded to scalpels.
"The robot is an intermediary between the surgeon's motions and the interaction with the tissue," Wagner said.
One advantage of the robot is motion scaling, meaning that surgeons could be free to perform larger gestures with their hands, which the robot would then transform into tiny millimeter-sized movements.
Another is the ability to add virtual boundaries and imaging guidance, which may stop accidental damage to the eye. "It's the equivalent of a surgical 'no-fly zone,'" Wagner explained. "It reduces the cognitive burden on the surgeon."
The robot also boasts some nifty innovations like the incorporation of haptic feedback so that surgeons can still rely on their sense of touch.
At present, Axsis remains more of a tech showcase than anything -- showing where surgical robots may go next and demonstrating that they are capable of performing even tiny, subtle motions like operating on an eye.
Will it eventually be used by real surgeons? Sadly, that question is out of Wagner's control. "We're just trying to show what's possible," he said, "although if a client comes to us and wants to develop this technology further, we're more than happy to do that."