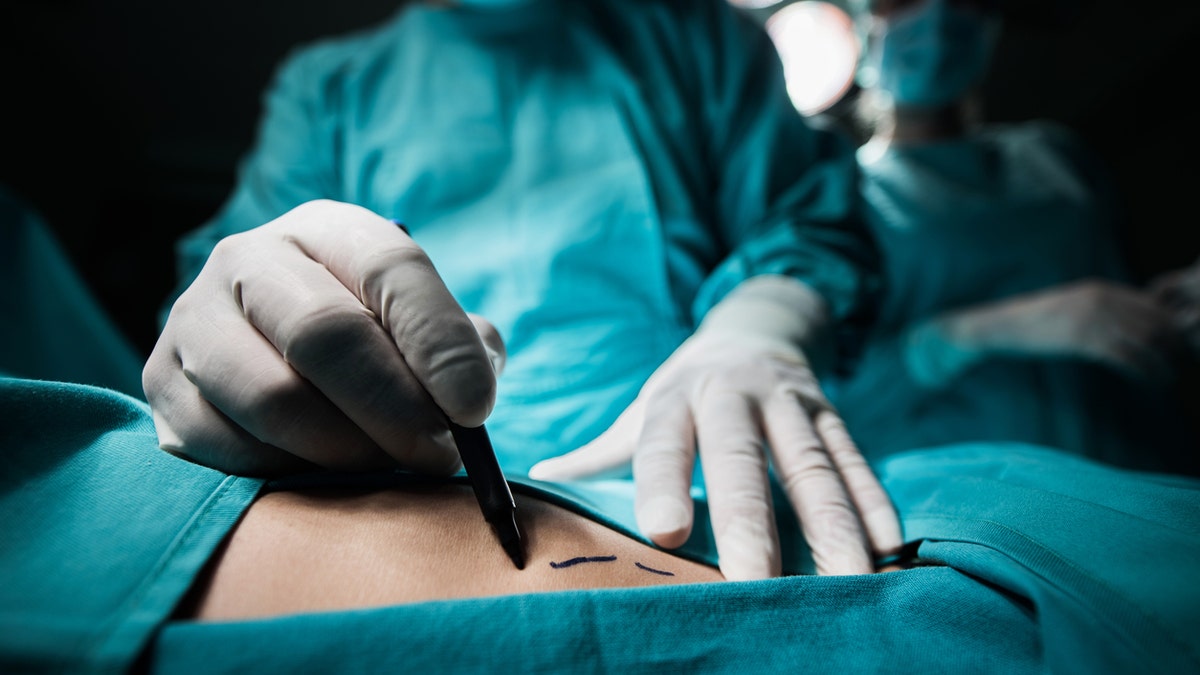
Close up of a plastic surgeon marking the human skin for surgery. (iStock)
When Ms. N came to Dr. John Hogan’s office last August, it had been nearly three months since she had felt like herself. Previously completely healthy, the 25-year-old woman had been plagued by shaking chills, fevers, and unremitting fatigue, barely able to drag herself to her job in a Boston-area accounting office. Most troubling, though, was the thin yellow fluid draining from her thighs and the undersides of her breasts. Little did she know this was the beginning of a life-changing saga.
Ms. N’s symptoms had started a little over two weeks after she underwent an operation in the Dominican Republic last May. The cosmetic surgery – known colloquially as a Brazilian butt lift – had entailed sucking fat out of the belly and low back, then injecting it into the buttocks and thighs. She also underwent breast augmentation.
The clinic had looked pristine, Ms. N later relayed. She received a weeklong course of antibiotic pills after the operation, and the surgical wounds seemed to be healing well. As instructed by the doctor, she kept the incisions clean, and didn’t swim or use hot tubs.
Just a few days after she returned to her home near Boston, she started draining the fluid from her breasts and thighs.
More From Stat News
“My first day back at work, I noticed my shirt felt wet,” Ms. N said in an interview with STAT. “I looked in my bra and saw this thin liquid.” Some days, the towels she stuffed into her bra to absorb the fluid became soaked within an hour or two.
Read more: Finding the world’s unknown viruses — before they find us
Around this same time, Ms. N noted large bruises on her legs; these became red and excruciatingly painful, sometimes opening up at night and releasing the same thin fluid.
“It stung like something was trying to push through my skin,” she said. “Sometimes I’d wake up soaked in the fluid.”
She’d become extremely fatigued — falling asleep at 5 p.m. some days — and was spiking fevers. She was also losing weight without trying to.
Worried about these symptoms, Ms. N went to see her primary care doctor, who took samples of this draining fluid and prescribed antibiotics, presumably thinking the draining sores stemmed from a standard postoperative infection. Over the next few months, the samples would show just a sprinkling of the types of bacteria that normally live on the skin, such as Staphylococcus aureus. Doctors prescribed Ms. N various types of antibiotic pills, and although her symptoms sometimes improved temporarily, they always returned.
Alarmingly, the silicone breast implants also eroded through her skin about a month after her surgery; they were visible through the incision. The implants were removed at a hospital in the Boston suburbs; the surgeon told Ms. N he thought they might be infected. Although the wounds were rinsed with an antibiotic called cefazolin, no samples were sent for microbiological studies.
Ms. N knew she didn’t feel quite right, but her doctors didn’t seem concerned.
“They were all telling me it was normal,” she said.
Putting it all together
By August 2016, Ms. N was fed up. She was then seen by Hogan, a fellow in infectious diseases at Massachusetts General Hospital.
In Hogan’s office, her vital signs were normal; she did not have a fever. On exam, Hogan noted that the opening in the fold beneath her left breast was draining something that was thinner than pus, but was nevertheless indicative of infection. He was alarmed at the way the infection had bored holes through Ms. N’s flesh.
“She had multiple draining ulcers separate from the surgical sites,” said Hogan, who has followed Ms. N closely ever since that first appointment. “It looked like a deep infection from within the soft tissue” making its way to the skin, he said.
Labs showed slightly high white blood cell and platelet counts, both of which can be high when there’s an infection or inflammation. Her kidney and liver tests were normal. Looking over Ms. N’s imaging, Hogan noticed what looked like areas of infection in the parts of her breasts seen in a CT scan of her chest – done a few weeks before to look for a clot in the blood vessels of the heart and lungs. Although it wasn’t noted in the radiology report, Hogan thought it might show some smudges indicating a collection of infected fluid. He made a mental note to dig deeper into this later.
Given her ongoing fevers, lab results, and skin findings, Hogan felt confident Ms. N was infected. The timing of her symptoms made Hogan fairly certain her infection was related to the surgery. He ruled out other possible sources of infection: Ms. N had no pets. She was not a drug user and never had been. She hadn’t traveled out of the country other than her recent trip for the cosmetic surgery.
The question was which microbe was causing the infection, and why the previous treatments hadn’t gotten rid of it.
Something didn’t quite fit
There were a few options, Hogan thought. Ms. N’s primary care doctor might have treated her with the wrong antibiotics, or for too short a time, for a commonplace bacterial infection. There also might be a walled-off collection of pus inside of her body that the antibiotics couldn’t reach. Yet if that were the case, the samples collected from the wounds should have grown a lot more bacteria; a mix of a few bugs commonly found on the skin wasn’t exactly a slam-dunk for an infection that just wouldn’t quit.
The other possibility, he thought, was an infection different from the usual ones after surgery in the United States. As opposed to fast-moving staph and strep infections, for example, bacteria in the mycobacterial family could cause chronic, draining infections.
At the forefront of his mind were Mycobacterium fortuitum, Mycobacterium chelonae, and Mycobacterium abscessus, which can cause infections of the skin and underlying tissue and are cousins to Mycobacterium tuberculosis, which causes tuberculosis. M. abscessus can cause lung infections, and more rarely meningitis or infections in the brain; thankfully, Ms. N did not have any of these. Special material is needed to grow mycobacterial species, so it wouldn’t be surprising that previous lab tests hadn’t revealed these bacteria.
Read more: My son had a devastating, mysterious illness. The conversation about palliative care knocked me flat
Another clue pointing to a mycobacterial infection was where Ms. N had undergone surgery. Operations performed outside of the United States — known as medical tourism — have been linked to Mycobacterium abscessus infections, particularly after cosmetic surgery, although the infection has occurred domestically as well. In fact, there was a recent outbreak among patients at a major US hospital who underwent a lung transplant or heart surgery.
But Hogan needed microbiological proof of what was causing the infection, so he cast a wide net, sending samples of the fluid from her legs and chest for analysis for fungi, mycobacteria, and nocardia, another rare cause of chronic bacterial infections. He also ordered breast and thigh ultrasounds to look for the hidden pockets of infection possibly seen on the CT scan. Finally, he switched Ms. N’s antibiotic to better treat staph on the off-chance that this was the cause of her symptoms.
At last, a diagnosis
Hogan and Dr. Raj Gandhi, his more senior colleague on the case, were not surprised when the cultures revealed Mycobacterium abscessus. The defining characteristics of the case — from the chronicity, to the sites and nature of fluid drainage, to the preceding surgery, to the recalcitrance of the infection to many antibiotics — pointed to an infection by this bug.
“It really was classic for mycobacterial disease,” Hogan said.
The tempo of the infection — never disappearing, but never ramping up to the extent that Ms. N developed a life-threatening systemic infection — was also typical. If the staph isolated from her wounds had been causing the infection, for example, Ms. N likely would have become much sicker, much more quickly — progressing over days, instead of lingering for months. The staph bacteria in her samples were innocent bystanders, not the root of her infection.
Another clue pointing to M. abscessus was the way more and more wounds kept popping up; run-of-the-mill postoperative infections tend to solely entail the area where the surgery was originally performed.
“This was an inside-out kind of thing,” said Gandhi. “Something that was inside from the procedure was expressing itself as drainage.”
For Ms. N, getting a diagnosis after months of searching felt like a breakthrough.
“I was relieved, because at least I had an answer,” she said.
Read more: 5 strange disease outbreaks that still puzzle scientists
The story continues
Although Ms. N is improving on powerful antibiotics, the infection isn’t gone yet; she has already undergone seven surgeries on her thighs and breasts to combat it, and may need more to eliminate it completely. Unfortunately, the antibiotics have serious side effects, including irreversible hearing loss. And her medical care has become so all-consuming that she had to leave her job. Still, she and her doctors hope she’ll end up infection-free.
Ms. N’s experience is a good reminder for clinicians of the importance of recognizing when a diagnosis doesn’t quite fit a patient’s constellation of symptoms.
“Doctors are taught certain patterns,” said Gandhi. “What you learn is then what you see, and if you see it a few times, it gets solidified, and that recognition gets easier.”
And for Ms. N, her story has driven home how crucial it is to listen to the body’s cues.
“Trust yourself and trust your body; you know when something is wrong,” she said. “I knew from the beginning that something wasn’t right.”
If you have dealt with a diagnostic puzzle, either as a caregiver or a patient, please email Allison at allisonbondmd@gmail.com.