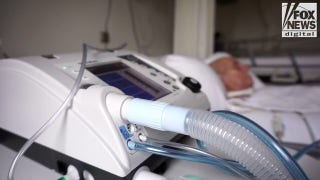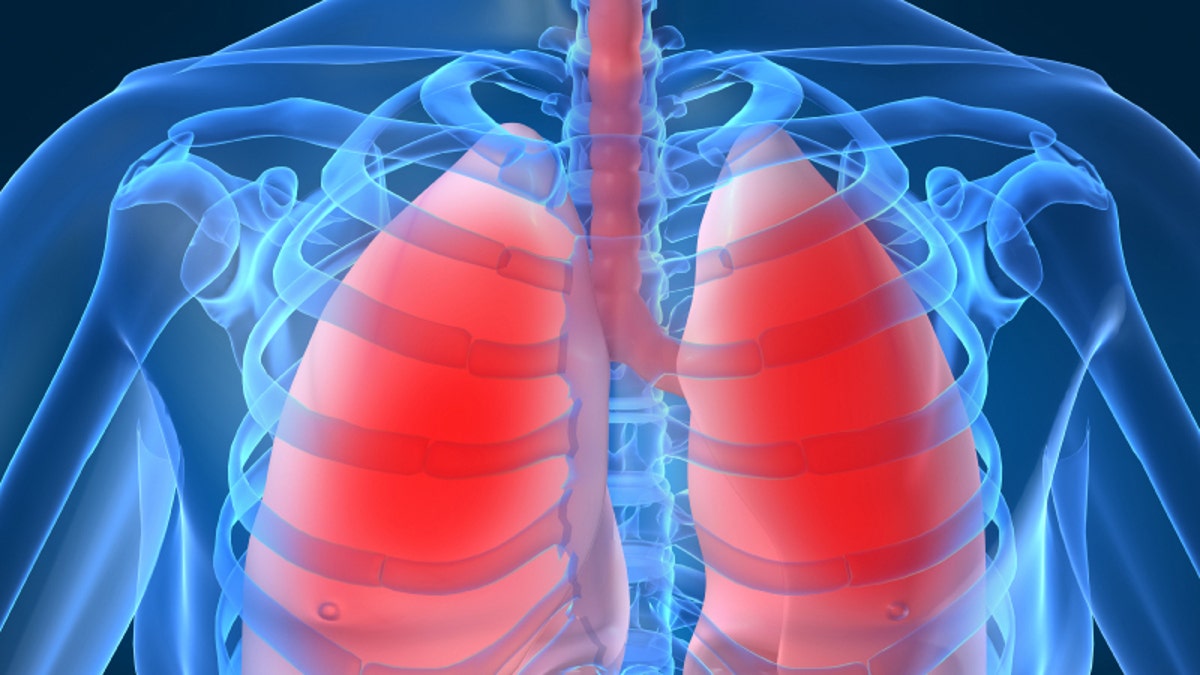
New treatments are helping slow the deadly course of a rare lung disease that is on the rise in the U.S. and world-wide.
Idiopathic pulmonary fibrosis leads to a buildup of scar tissue that makes it increasingly difficult for the lungs to function normally and provide the body with oxygen. The disease has no known cause, setting it apart from related pulmonary diseases where doctors can identify specific irritants or exposures to toxins such as asbestos. Its symptoms—shortness of breath and persistent cough—resemble diseases like asthma and emphysema, often leading to missed or delayed diagnoses.
Now, with improved understanding of IPF and better diagnostic guidelines for catching it in earlier stages, researchers say the number of people afflicted is substantially higher than previously thought. According to the National Institutes of Health, it affects an estimated 200,000 Americans, mostly middle-aged and older adults. A study last year in the Lancet Respiratory Medicine found that prevalence among Medicare patients over 65 more than doubled between 2001 and 2011 and is increasing annually.
Historically more men have been diagnosed, but IPF in women is increasing. It kills about 40,000 patients each year, the same number that die of breast cancer. Only half survive more than two to three years from the initial diagnosis as their lungs stop working, from causes including respiratory failure and pneumonia. Lung transplants are one option for treatment, but can be done only for a limited number of patients.
Two new drugs have been shown to slow progression, and pharmaceutical companies are exploring potential new therapies that may offer improvement to current medicines. They are looking at combinations with other drugs and the use of an approved therapy for basal cell carcinoma, a skin cancer, as a potential treatment for IPF.
Researchers suspect the disease is linked to an exaggerated or uncontrolled healing response, possibly triggered by the immune system, which produces excessive scar tissue in the lungs and thickens the walls of the alveoli, or air sacs. Smoking is one of the most recognized risks. Exposure to wood or metal dust, viral or bacterial lung infections, and a history of acid reflux disease are possible culprits.
Charles Boetsch, a 69-year-old consultant, says he was always fit and active, so he knew something was wrong in 2011 when he began experiencing a dry cough and extreme shortness of breath. After multiple tests with different doctors, a high-resolution CT scan in 2013 showed he had IPF; he decided against an invasive lung biopsy for further confirmation. He had never heard of the disease and was stunned to learn there is no cure.