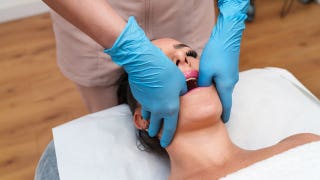
When Liz Cooper was 25, she felt a lump in her right breast, but didn’t think much of it. She was young, had just lost 70 pounds and was being counseled by a nutritionist and trainer. Breast cancer also didn’t run rampant in her family -- her grandmother had been diagnosed with it, but not until well into her 80s.
“There were no real symptoms, there was just the lump under my armpit in the breast area,” Cooper, now 26, told FoxNews.com.
Cooper works in the billing department at Stamford Hospital near her home in Connecticut, and told a nurse about the lump.
“She asked if I was on my period because during menstruation it’s common to feel lumps or fluid in your breast,” she said. “Two weeks later it was still there, so I made an appointment with my doctor, got a prescription for an ultrasound, had it done and they knew right away at the ultrasound,” she said. A subsequent biopsy confirmed the lump was cancerous.
Cooper was diagnosed with stage 1B invasive micropapillary breast carcinoma and micrometastasis in the lymph nodes. She tested positive for a protein called human epidermal growth factor receptor 2 (HER2), which promotes the growth of cancer cells; HER2-positive breast cancers tend to be more aggressive than others. Because her cancer tested positive for estrogen and progesterone, Cooper had her lymph nodes removed to avoid further spread.
“I can’t take birth control because it’ll feed it,” she said.
Cooper’s diagnosis shocked her doctors, and she underwent genetic testing to see if she might be susceptible to any other mutations. She tested negative for mutations to the BRCA 1 and BRCA 2 genes, and aside from her grandmother does not have a family history of the cancer.
Ultimately, she decided to undergo a bilateral mastectomy— removing both the breast with cancer and the healthy breast — despite results testing negative for the BRCA 1 and BRCA 2 mutation. Had she chosen a lumpectomy, she would have had to endure biopsies and imaging every six months to monitor any development in her affected breast. In addition to the stress of the surgeries, Cooper also had to decide whether to freeze her eggs before beginning chemotherapy.
“I went through two cycles of egg freezing – oocyte cryopreservation— and my insurance only covered $5,000 of it,” Cooper said. “I also had to get over the fear of giving myself shots for it.”
During this time, Cooper had five surgical drains attached to body and was unable to drive while she recovered from the double mastectomy. Her parents, boyfriend and best friend managed her medications around the clock and drove her to and from appointments. When all was said and done, she was ready to start chemotherapy in August 2015.
“I was terrified of being sick and losing my hair,” she said. “When you don’t have hair, [people] know that you’re sick.”
Cooper decided to donate 14 inches of her hair to Pantene’s Beautiful Lengths partnership with the American Cancer Society before she lost it to chemotherapy. Her treatment required a cocktail of four different drugs and six cycles of chemotherapy every 21 days. Once she completed it, Cooper began a targeted therapy that will last through August. At that time, she’ll be placed on a hormone blocker for five years, and continue to go for follow-up scans for the rest of her life.
“The feelings from chemotherapy were like having the flu, pneumonia and severe exhaustion all together,” she said. “It feels like you drink carbonated metallic gasoline – it does not make you feel very well.”
The drugs also affected her memory, and Cooper said she sometimes feels like she’s in a constant fog. She doesn’t have much time or energy to socialize, as she is in physical therapy three to four times per week to treat painful lymphedema, which is a result of the surgery to remove her lymph nodes.
“I feel like I live at the doctor’s office so my schedule is very hectic with appointments, and it’s just not your average 25-year-old’s schedule,” she said, adding that it's difficult to know she could be attending graduate school or traveling at this time.
“Instead I had to be careful going out in public because if my white blood count was low I could risk getting an infection,” she said. “I couldn’t relate to people’s conversations anymore – I had totally different problems and issues and nobody truly understands how many treatments are involved with having cancer.”
To stay inspired on her darkest days, Cooper turned to the wisdom of two co-workers who are breast cancer survivors, as well as her friends and family urging her to be strong. Her friends started a GoFundMe for her medical care, with the response helping to boost her morale even more. In addition, she found an online support group exclusively accessible to breast cancer patients. On April 2, her alma mater, Manhattanville College in Purchase, New York, is holding a lacrosse game benefitting breast cancer research in her honor.
The experience has taught he the importance of paying attention to your health, even when you’re young.
“It’s really important to go to your yearly gynecological visits and physicals with your primary care physician,” Cooper said. “If you’re ever worried or concerned about something that you think is unusual with your body – always go get it checked out just to be sure.”
Cooper will be back in surgery in two weeks to undergo another step in her breast reconstruction surgery, permanent implants. After the bilateral mastectomy, she had tissue expanders implanted behind the pectoral muscle. Over several procedures, her surgeon injected saline into the expanders to make room for permanent implants. The final step will be nipple reconstruction.
Cooper credits her diet and exercise with helping her to find the cancer early.
The biggest thing she learned? “Don’t doubt something just because of your age.”