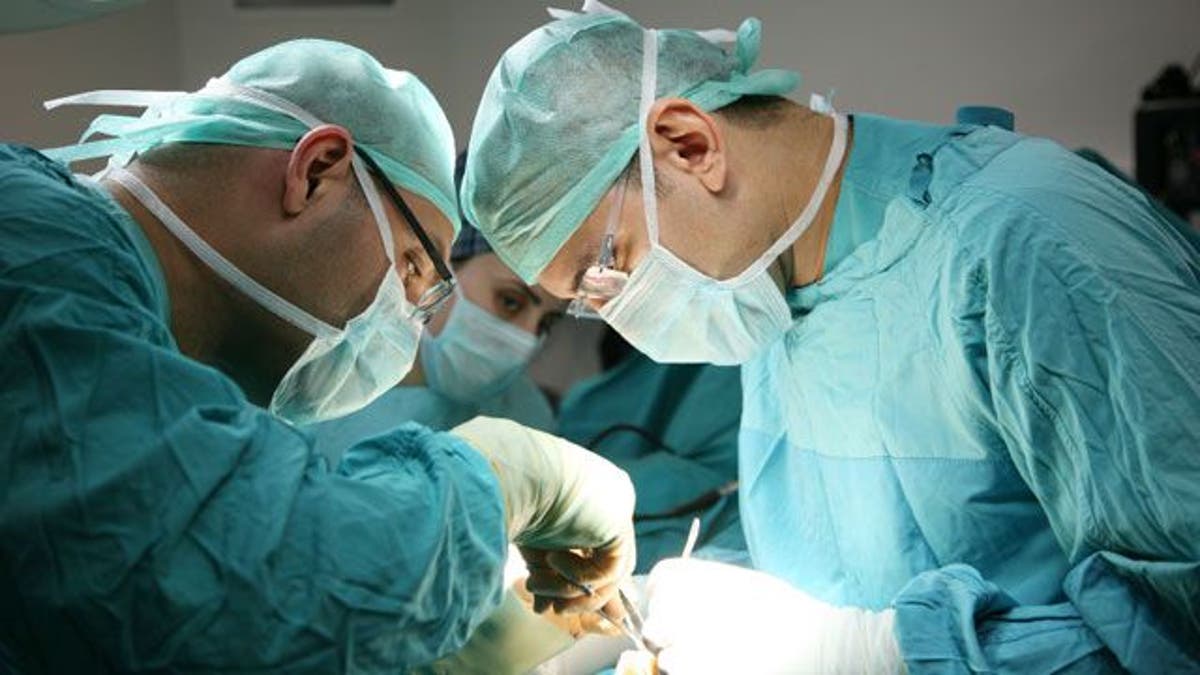
In a small long-term study, obese patients who had gastric bypass surgery were half as likely to die as those who didn’t have the surgery, researchers found.
They saw little difference in death rates for the first two to three years, but 10 years after gastric bypass surgery, even diabetic patients had significantly better survival if they had the surgery.
“There's really limited long-term follow-up data, especially comparing bariatric surgery to no surgery or the usual medical care,” Dr. Peter Hallowell, the study’s senior author, told Reuters Health.
“We’re hoping to fill that void with a study like this,” said Hallowell, a surgeon with the University of Virginia Health System in Charlottesville.
During a gastric bypass operation, a surgeon divides the stomach into two portions and connects the smaller upper portion directly to the small intestine.
The National Institutes of Health says patients may be candidates for weight-loss surgery, or bariatric surgery, if their body mass index (BMI) is 40 or above, or 35 or more along with diabetes or hypertension.
BMI is a measure of weight relative to height. A BMI of 30 to 39.9 is considered obese, and 40 or above is severe, or morbid, obesity.
As reported in the American Journal of Surgery, the study team carefully matched 430 obese patients who had gastric bypass surgery to another 401 patients who did not have gastric bypass, but were otherwise very similar.
They found very little difference in the first two years after the surgery (three years for diabetes patients).
But by ten years of follow-up, 6.5 percent of the surgery patients had died, compared to almost 13 percent of the patients who did not have the surgery.
When the researchers looked just at patients with diabetes, they found that 10 percent of the gastric bypass group had died, compared to 19 percent of the matched non-surgery patients.
“If you’ve tried dieting, exercise and medical management and that's all failed, then you really should consider a surgical option - especially if you have diabetes,” Hallowell said.
Currently, only one or two percent of patients who are eligible for weight loss surgery ever have it, he noted.
“We really have a long way to go both to educate the public, educate legislatures and educate (insurance companies) that this is safe, it's effective, and it increases long-term survival,” he said.
Hallowell said bariatric surgery is really quite safe.
“The current data of what we consider ‘early mortality’ in the first 30 days is basically about two people in about 1000, which is less than the mortality rate associated with having a gallbladder removed and it's getting down on the order of having your appendix removed,” he said.
There are different types of bariatric procedures. Hallowell said sleeve gastrectomy was the most popular bariatric operation in 2014, but the current study only looked at gastric bypass, an older procedure.
“Unfortunately for those (new) procedures the data is only three or four years old, so we just didn't have any patients that we could include in this type of study to be able to go out 10 years,” he said.
Martin Gulliford, a bariatric researcher at King's College London in the UK, said there is growing appreciation of the potential of surgery for severe obesity.
“In the short-term, weight loss surgery procedures may be associated with substantial weight loss and remission of diabetes in up to 60 percent of patients,” Gulliford told Reuters Health in an email.
However, less is known about long-term outcomes, said Gulliford, who was not involved in the new study.
He said the new findings must be treated with some caution, as there were only 26 patients who died in the surgical group, and 51 in the control group.
“Despite the carefully conducted matching procedure, there may have been unmeasured differences between the two groups, other than surgery, that influenced patient outcomes,” he added.
Nevertheless, Gulliford said, the new data add to earlier findings that suggest weight loss surgery may be associated with lower mortality in people with severe obesity.