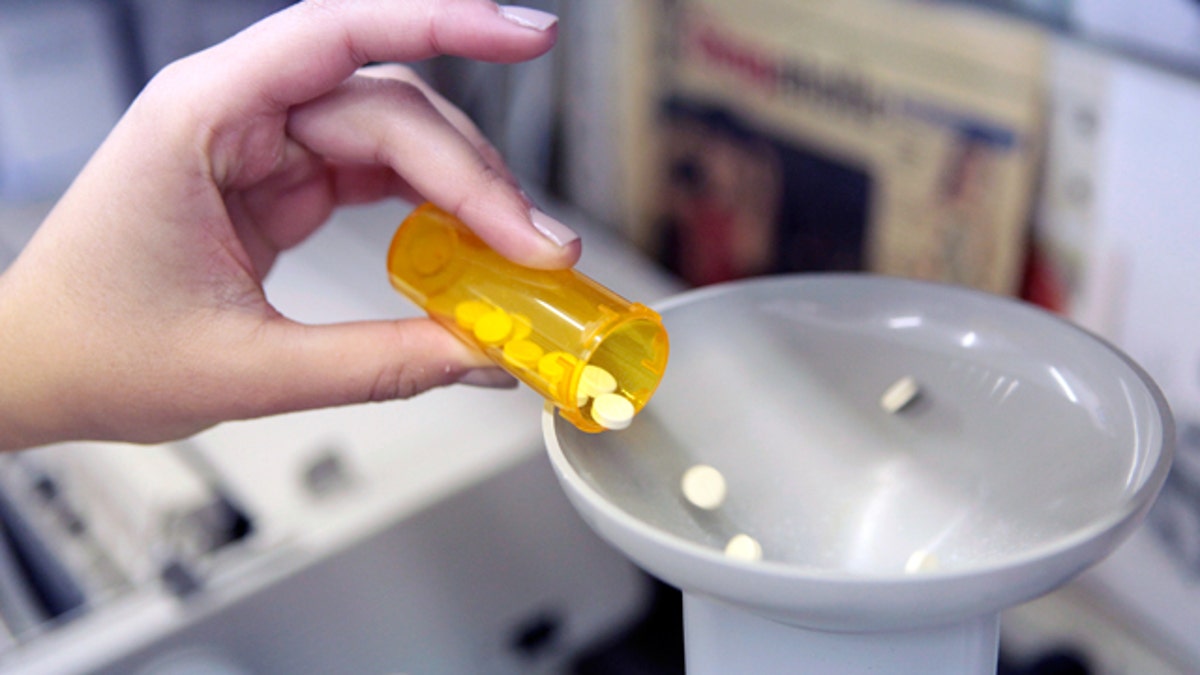
(Reuters)
Two years into an escalating shortage of life-saving cancer drugs, regulators and lawmakers are still unable to identify why it is happening, let alone how to solve the problem.
Hospitals and doctors across the country are postponing care or using second-best or more costly alternatives. The shortages have also forced delays in clinical trials for cancer, which use these drugs as a baseline to test the effectiveness of novel therapies.
While work-arounds can help for a while, what is perhaps most worrying is that the officials in charge of addressing the problem are no closer to identifying the underlying causes.
In the balance are hundreds of thousands of patients, and potentially millions, who may not get the full care they need.
"Anybody who is sure they know the answer to this question is probably kidding themselves," said Peter Lurie, a senior adviser in the Food and Drug Administration (FDA) Office of the Commissioner, who works on public health issues, including drug shortages.
"There appear to be multiple factors that are playing in it and it's very difficult to identify which one is most important," Lurie told Reuters.
Drug shortages have been around for years in the United States, but they were previously intermittent and largely temporary, pharmacists and doctors say. They have shot up in a very short time, with a record of over 200 scarce medicines this year alone, up from 56 in 2006, according to FDA data.
Health providers say the companies who make these drugs, long sold in generic form, have a diminishing interest in ensuring a strong supply. After a wave of consolidation, only five to seven companies produce 80 percent of these medicines, and stricter reimbursement policies have cut into the profits.
But a group representing companies such as Watson Pharmaceuticals Inc and Sandoz, a division of Novartis AG, blames the FDA for introducing unnecessarily strict inspections and shutting down manufacturing facilities for minor issues.
The finger pointing and lack of answers is leaving health providers and patients exasperated.
"Something has to be done soon in order to try to alleviate this problem," said Dr. Michael Link, the current president of the American Society of Clinical Oncology (ASCO), a non-profit group of cancer doctors and other providers.. "Right now we're already seeing patient care suffering... I think you're seeing a groundswell of concern."
In the meantime, distributors in the so-called "gray market" are exploiting the situation to peddle the drugs at hundred-fold mark-ups, according to lawmakers investigating the situation.
Senator Chuck Schumer, a Democrat from New York, has called for an investigation by the Federal Trade Commission. And last week, Representative Elijah Cummings, the top Democrat in the House Committee on Oversight and Government Reform, asked five companies in the gray market to provide information on their sales and how they obtain the drugs.
Patients in the Balance
In a July survey of 820 hospitals by the American Hospital Association, more than four-fifths of hospitals said they had to delay treatment and more than half could not provide patients with the recommended drug for their disease. Sixty-nine percent of patients had to settle for a less effective drug.
The non-profit Institute for Safe Medication Practices (ISMP) has reports of at least 15 patients dying from drug shortages since last September. In the most high-profile case, nine patients died from contaminated IV fluid in Alabama this past March, when the typical supply was unavailable.
Of the 140,000 patients diagnosed with colorectal cancer each year, about 80,000 are expected to rely on typical treatments such as fluorouracil or leucovorin, both currently in short supply, said Nancy Roach, a board member at the patient group Fight Colorectal Cancer.
The government is trying to create a better notification system for shortages, which could address some of the most immediate issues for patients.
Senator Amy Klobuchar, a Democrat from Minnesota, along with Robert Casey, a Democrat from Pennsylvania, introduced a bill in February that would force drug companies to inform the FDA about looming shortages. The FDA said early notification helped it prevent 99 shortages so far this year.
But the bill does little to prevent shortages in the long-term. "People aren't in agreement on how to solve it in the long term, and not a lot of bills are going through Congress," Klobuchar told Reuters.
Market Perfect Storm
The FDA began tracking drug shortages closely in 1999. Over a decade later, they have only gotten worse. Sterile injectables such as the cancer drugs, make up the lion's share and accounted for 132 out of 178 shortages in 2010.
Most are generic and have been around for years, meaning profit margins are lower.
The FDA can explain the immediate causes of the shortages—in 2010, over half of them came from product quality and "significant" manufacturing problems such as metal shavings found in vials or fungal contamination, said Sandra Kweder, deputy director of the FDA's Office of New Drugs.
But these reasons fail to address why these problems have gotten so much worse, officials and industry analysts said.
Industry consolidation and lower inventory levels could exacerbate the problem, leaving less slack in the system to deal with shortages when they arise, the FDA said.
The agency has also blamed an increasing number of production issues on older facilities that need to be renovated as manufacturers in the low-margin generic market avoid investments in maintenance. Makers of sterile injectables Teva, Hospira and Bedford Laboratories, part of privately-held Boehringer Ingelheim, have all had manufacturing issues in the past few years, shuttering production on multiple drug lines.
The FDA also acknowledges some manufacturers may have less financial incentive to make older, cheaper generic drugs. In 2010, 11 percent of shortages were due to companies that stopped making a certain drug, usually for business reasons.
Manufacturers are loathe to make a connection between the financial incentives and producing older medicines. Several, including Teva Pharmaceuticals and Hospira, say they are building new facilities as a back-up for future shortages.
The industry lays part of the blame with the FDA. The Generic Pharmaceutical Association (GPhA) said the agency has become more focused on enforcement in the past three years, shutting down factories for smaller problems that would have been dealt with less drastically in the past.
Stalled Proposals
Various proposals to address the long-term problem have stalled, not least because of the disagreement over the cause.
They include creating a national stockpile for emergency injectables—just like for vaccines—or offering tax incentives for manufacturers of low-cost but life-saving products. But those are unlikely to gain favor as the U.S. government is scrambling to cut costs and reduce the national debt, lawmakers and industry players said.
The International Monetary Fund and the U.S. Department of Health and Human Services are both investigating the issue, and a Government Accountability Office report is due to come out in November, according to a congressional staffer.
In the meantime, doctors like Steven Abrams, at Texas Children's Hospital in Houston, work to make sure newborn infants with intestinal damage have enough calcium and phosphates.
These essential minerals—manufactured by APP Pharmaceuticals, a company in the Fresenius Kabi Group, and Hospira—have been in short supply since April, Dr. Abrams said, forcing him to ration treatment to those most in need.
"Our task is to continue to advocate for long-term solutions," he said. "And the second is to manage this problem day to day. That's just what we have to do, ... to make sure the babies get the medicine they need."
