
Tracheotomy Alleviated Baby Joseph’s Pain
By , ,
Published October 28, 2015
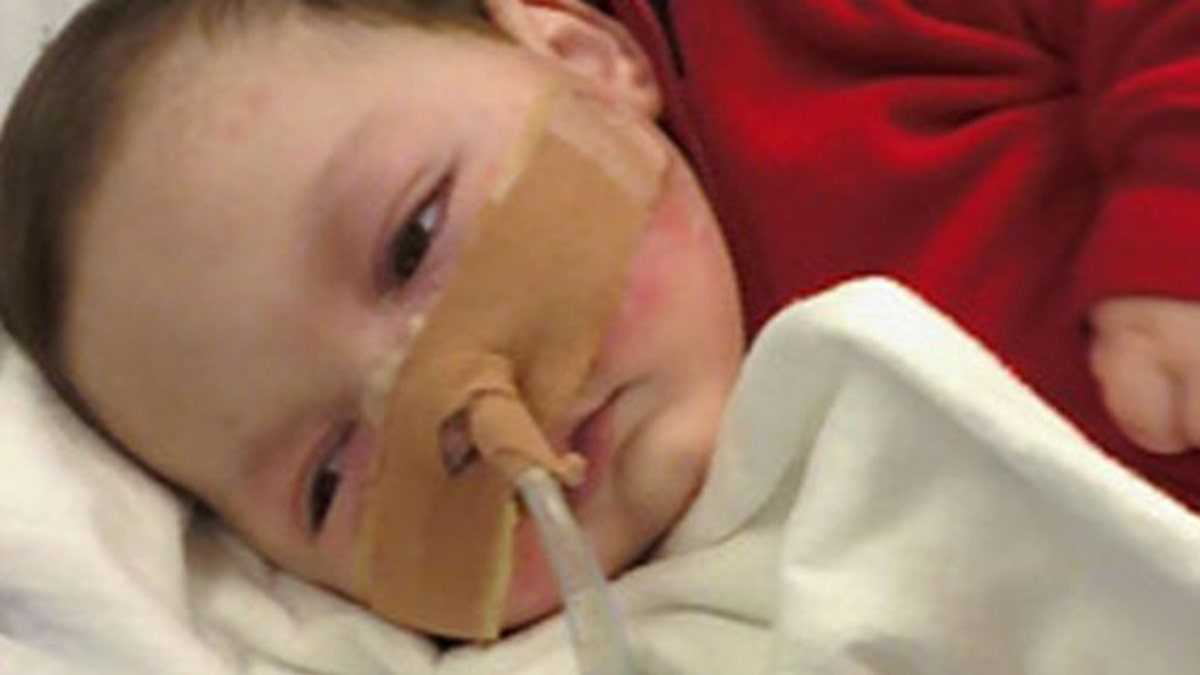
(Photo from Moe Maraachli)
I want to take this opportunity to commend the doctors at Cardinal Glennon Children’s Medical Center in St. Louis for performing a tracheotomy on little Joseph Maraachli.
Joseph Maraachli, a 13-month-old boy, known to the world as “Baby Joseph,” has sparked renewed vigor into the “right-to-life” debate.
Joseph was born with a progressive neurological disease called Leigh Syndrome. Doctors at the Canadian hospital where he was being treated determined that he was in a permanent vegetative state and were ready to remove his breathing tube.
Joseph’s parents, however, fought to have a tracheotomy performed, so that Joseph could spend his remaining days at home. But after a Canadian court upheld the doctors’ orders, the Maraachlis sought help from Rev. Frank Palone and the Priests for Life organization, who rescued Joseph and placed him in the care of the doctors at Cardinal Glennon Children’s Medical Center.
There, Joseph received the tracheotomy his parents requested and is expected to remain in intensive care for 7 to 10 days. When discharged, he will be treated at Ranken Jordan, a pediatric specialty hospital in St. Louis, and finally, he will be able to return to his family home in Windsor, Ontario.
I’ve heard many comments on this story, ranging from supportive to critical. Some people I’ve talked to are upset – they believe that by performing a tracheotomy, Joseph’s parents and doctors are prolonging his suffering.
I have to disagree. I believe the actions taken by the hospital fall in line with the standards that many institutions have in regard to palliative care for children with terminal diseases.
The goal of palliative care, as defined by the American Academy of Pediatrics, is to promote the welfare of infants and children living with life-threatening or terminal conditions and their families. The guidelines include having sensitivity to and respect for the child's and family's wishes as well as alleviating pain and providing access to therapies that will improve the child’s quality of life.
And as far as I’m concerned, that’s exactly what Joseph’s new doctors did in this case.
Let’s get something straight: A tracheotomy does not necessarily prolong the life of terminally ill patients. Its main purpose is to provide comfort to the patient.
Breathing tubes inserted through the mouth or nose can cause painful sores to develop along the inside of the mouth and throat. A tracheotomy, meanwhile, inserts a tube directly into the throat through an incision in the neck. This eliminates some of the pain and discomfort associated with intubation.
In this particular case, the tracheotomy will also allow Joseph to go home and live out his remaining days with his family.
So, according the guidelines for palliative care – it appears to me that Joseph’s doctors acted exactly as they should have acted. They respected the wishes of their patient’s parents, who wanted their son to come home, and they alleviated some of Joseph’s suffering.
It was the right care for the right patient, and I applaud them for their efforts.
https://www.foxnews.com/health/tracheotomy-alleviated-baby-josephs-pain