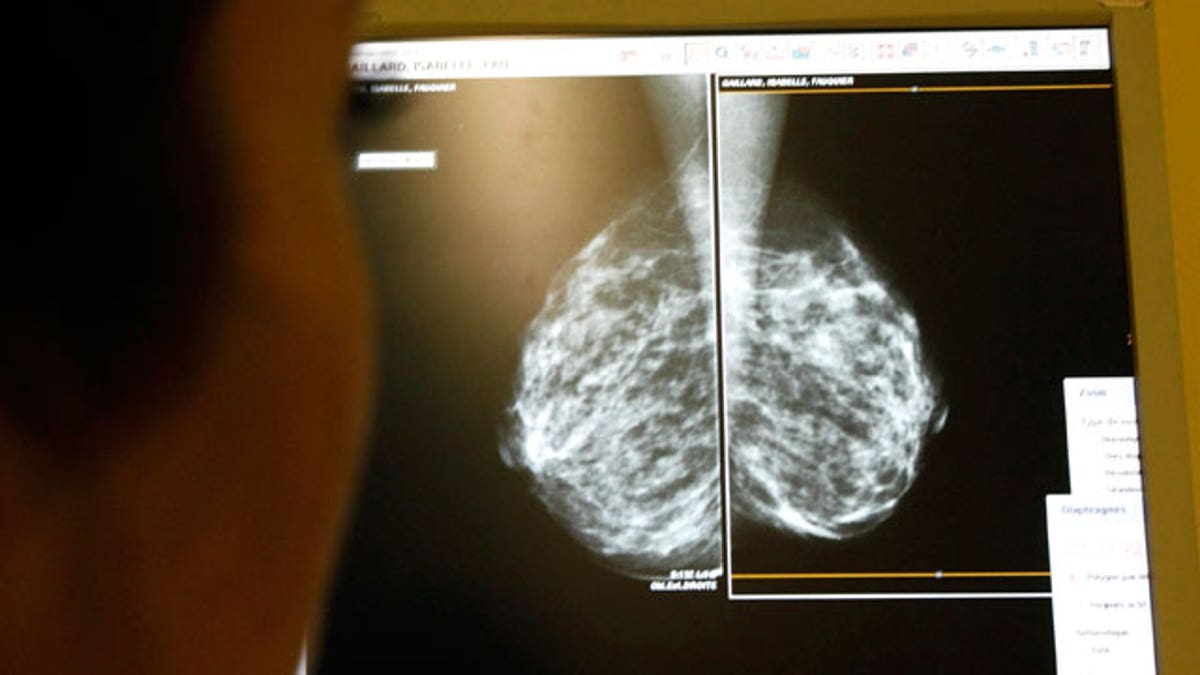
(Reuters)
Nearly nine in 10 women with early breast cancer have imaging exams to see if the cancer has spread, despite official recommendations against such tests, a new study suggests.
The American Society of Clinical Oncology and the National Comprehensive Cancer Network recommend against looking for metastatic cancer in women with stage I or II breast cancer. That’s because less than two percent of these women will have metastases, and there’s a high risk that the tests will be falsely positive, leading to unnecessary extra testing, delays and anxiety.
“The extensive evidence tells us that for women with asymptotic early stage breast cancer, the chance of seeing metastases is so low that the risk of harm is far greater,” said senior author Dr. Mark Clemons, an oncologist at The Ottawa Hospital and the University of Ottawa in Ontario.
Stage I and II breast cancers involve small tumors still contained within the breasts or sometimes the lymph nodes, according to the National Cancer Institute. More than 75 percent of women with these early stage cancers will survive at least five years. Doctors determine breast cancer stage by testing tumor cells and lymph node cells.
Doing many imaging studies on patients who do not need them delays these exams for patients with other diseases who do need them, and leads to more radiation exposure for the breast cancer patients, Clemons told Reuters Health by e-mail.
As reported in the Canadian Medical Association Journal, he and his coauthors analyzed 2007-2012 data from an Ontario cancer registry. They found that out of 26,547 women diagnosed with stage I or II breast cancer, 86 percent had at least one imaging test to see if the cancer had spread, like an X-ray, computed tomography (CT) scan, or magnetic resonance imaging (MRI) or positron emission tomography (PET) scan.
More than 90 percent of women with stage II cancer had imaging of the skeleton, thorax, abdomen or pelvis within three months of their cancer diagnosis.
Surgeons and oncologists most often ordered the imaging tests, both before and after the women had surgery to remove the breast cancer.
Women who were younger and those with multiple other medical conditions were most likely to have the imaging.
“Most of us will have tiny, clinically irrelevant abnormalities found on radiology tests that, in the absence of a cancer diagnosis would hardly be mentioned on an X-ray report,” said Dr. Daniel Rayson of Queen Elizabeth II Health Sciences Centre and Dalhousie University in Halifax, Nova Scotia.
Rayson, who coauthored an editorial accompanying the new results, added, “When these tests are done for a patient newly diagnosed with early stage breast cancer and the same tiny abnormality is found, the first concern is that of metastatic disease and this usually triggers further testing and evaluation which results in escalating anxiety, and occasionally can lead to wrong conclusions.”
The tests are easy to order and at one time were thought to be important for women with early breast cancer, he told Reuters Health by email.
“It does take considerable time to change what had been previously thought of as both important and routine in medicine,” Rayson said.
This unnecessary imaging adds up to many millions of dollars in extra costs, does not help the patient, and can harm her, Clemons said.
“Clearly in this setting, more is certainly not always better,” he said.
Several forces need to work together - advocacy groups, health care funders, patients and physicians - to encourage doctors to follow guidelines and not order imaging for these breast cancer patients, he said.
“This is a great example of a situation where we can spend less and actually deliver better care for individual patients as this is likely a global issue,” he said.
