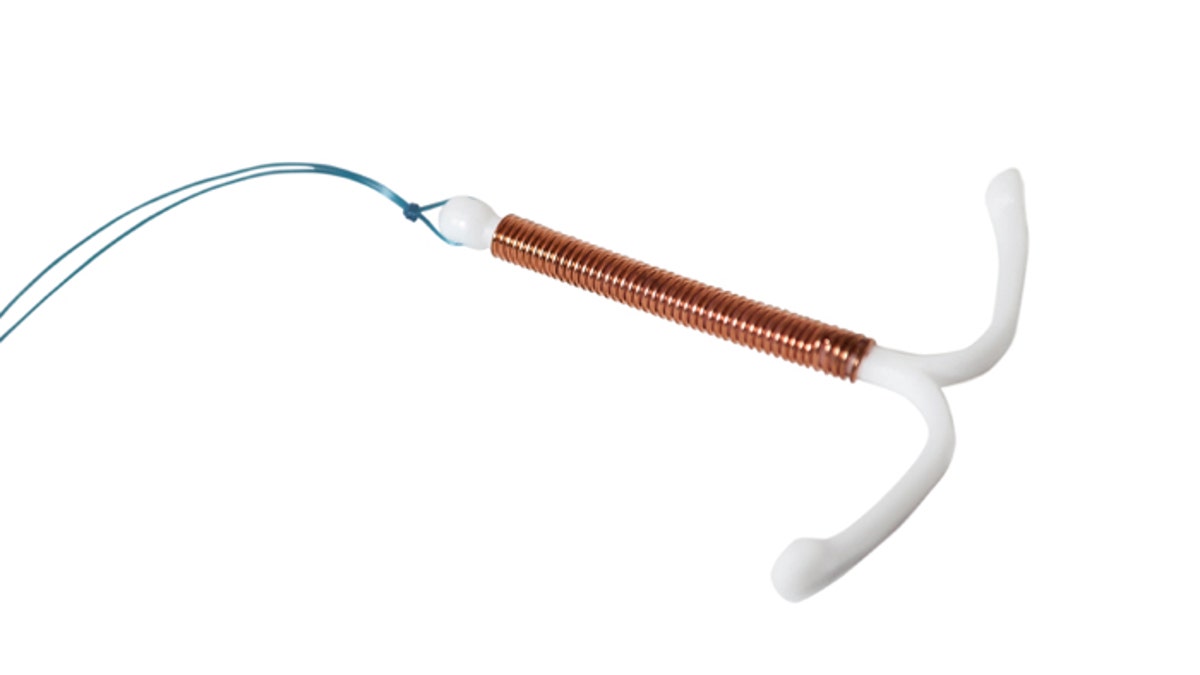
College women who choose an intrauterine device (IUD) for long-term contraception say it hurts to have the device inserted at first, but they are otherwise very happy with it more than a year later, according to a new U.S. survey.
The American College of Obstetricians and Gynecologists (ACOG) and the American Academy of Pediatrics (AAP) have both endorsed IUDs as first-line contraception for young women who have never had children, but many providers, especially in the U.S., still are not comfortable giving IUDs to these women, said lead author Dr. Alexandra M. Hall of the University of Wisconsin in Menomonie.
“It all comes back to the 1970s with the Dalkon shield IUD, people got terrible pelvic infections,” Hall told Reuters Health.
Soon after, IUDs were redesigned and now pelvic inflammatory disease is no more common among IUD users than among women on the pill, she said.
For reversible long-term contraception, the copper IUD, hormonal Mirena IUD and hormonal Implanon rod inserted under the skin of the arm are the most effective, with failure rates below 1%. They last for 10, five and three years, respectively.
Short-term methods including the birth control pill, patch and hormonal vaginal ring all have failure rates of 9%, according to the Centers for Disease Control and Prevention. Failure rates are higher for these methods because people may use them inconsistently or incorrectly. The diaphragm, and male and female condoms all have failure rates between 12 and 21%.
Despite the fact that IUDs are safe, effective and well-tolerated, “some people are a little more cautious, and very afraid of doing harm,” especially to young women who have not been pregnant, said Hall, who worked on the study while at Cornell University in Ithica, New York.
“Physicians and other healthcare practitioners who work more with younger people are going with (the ACOG and AAP) recommendation,” Hall said. “We view unintended pregnancy as significant harm.”
Researchers studied 109 students at Cornell who chose to have the Paragard Copper T 380A or the Mirena levonorgestrel intrauterine system placed in 2012 or 2013. The women, aged 18 to 30 years old, had never had children.
Most chose Mirena, while only 21 chose the copper IUD.
At one month, six months, one year and 18 months after having the IUD placed, they responded to online surveys about complications, bleeding patterns, plans to continue with the device and overall satisfaction.
Most women reported moderate to severe pain at the time of insertion and mild to moderate pain in the first 24 hours. Pain had dissipated for most by one week later.
Six months later, women with the copper IUD reported longer, heavier and more painful periods than those with the hormonal version, Mirena.
Three of the women expelled their IUDs spontaneously and seven chose to have theirs taken out, due to side effects like pain and bleeding or lack of benefit.
One woman became pregnant during the study, but there were no cases of uterine perforation, pelvic inflammatory disease, chlamydia or gonnorhea, the researchers reported online April 8 in the Journal of Family Planning and Reproductive Health Care.
After an average of 13 months of follow-up, 83% of women were happy or very happy with their IUD and 75% said the insertion procedure had gone “very well.’” Almost 90% were still using their IUD at the one-year point, and 87% were likely to recommend it to a friend.
These results should help prepare young women for the experience of having an IUD, Hall said.
“The copper T does make periods heavier and longer and crampier, you really need to be prepared for that,” she said.
In this and previous studies, many women have stuck with their IUDs likely because they were counseled about potential side effects beforehand, so those who would not tolerate them did not choose to have a device placed, she said.
“There is still a feeling among some providers and among a lot of parents and people helping young women with decision making that IUDs may not be right for them,” said Dr. Julie Strickland, chair of ACOG’s Adolescent Health Care Committee, who was not involved in the new study.
“The more we can get out there to show that it’s safe and efficacious and really well tolerated and well liked among young adults, the better,” Strickland told Reuters Health.
