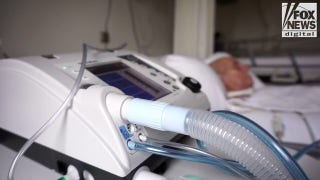
Heidi from Limburg, Belgium, smokes a joint in the Toermalijn coffee shop in Tilburg April 29, 2012. A controversial law that will make it harder for foreign tourists to buy cannabis at the Netherlands' famous coffee shops has been upheld by a Dutch court. The law, which goes into force in three southern provinces on May 1 before going nationwide next year, means coffee shops can only sell cannabis to registered members. Picture taken April 29, 2012. REUTERS/Michael Kooren (NETHERLANDS - Tags: SOCIETY BUSINESS DRUGS TRAVEL) - RTR31G54 (REUTERS/Michael Kooren)
A study published Monday in the journal Lancet Psychiatry has linked smoking strong, high-potency marijuana to an increased risk of developing psychiatric disorders.
Study authors from the Institute of Psychiatry, Psychology and Neuroscience at King’s College London, analyzed about 800 people ages 18 to 65. According to a news release, at the beginning of the study, 410 of those patients had reported a first episode of psychosis and 370 healthy patients were used as a control. After examining their marijuana use, researchers observed that compared to those who never smoked, study participants who tried the stronger variety of marijuana had a threefold increased risk of developing psychosis. Those who used the potent pot every day had a fivefold increased risk of developing psychosis.
“Skeptics still claim that this is not an important cause of schizophrenia-like psychosis. This paper suggests that we could prevent almost one-quarter of cases of psychosis if no one smoked high-potency cannabis,” senior researcher Sir Robin Murray, a psychiatric research professor at King’s College, said in the news release.
The use of hash, a milder form of marijuana, wasn’t linked to a heightened risk of psychosis. Hash has a higher concentration of cannabidiol (CBD) than more potent forms, which have a higher percentage of marijuana’s psychotropic ingredient, tetrahydrocannabinol (THC). CBD is believed to offset the effects of THC.
In the study, researchers defined high-potency weed as having greater than 15 percent THC content. Hash was defined has having less than 5 percent THC content.
According to the Washington Post, most of the marijuana in the U.S. is of the high-THC variety, and the average strength of weed that federal authorities have seized over time has risen. The Post noted that many retailers in Colorado, where recreational marijuana has been legalized, sell strains of weed that contain 25 percent THC or more. The newspaper likened today’s weed to “prohibition-era moonshine.”
The U.K. study authors said their findings are significant because cannabis potency and frequency of use are often overlooked when determining how harmful a drug can be, but that these factors are crucial in analyzing how the drug will impact a patient’s mental health.
“As with smoking tobacco and drinking alcohol you need a clear public message,” lead author Marta Di Forti, clinician scientist, said in the news release. “When a [general practitioner] or psychiatrist asks if a patient uses cannabis, it’s not helpful; it’s like asking whether someone drinks. As with alcohol, the relevant questions are how often and what type of cannabis. This gives more information about whether the user is at risk of mental health problems; awareness needs to increase for this to happen.”