
Major setback for AIDS cure: Study finds reservoir of hidden HIV bigger than once thought
By , ,
Published October 27, 2015
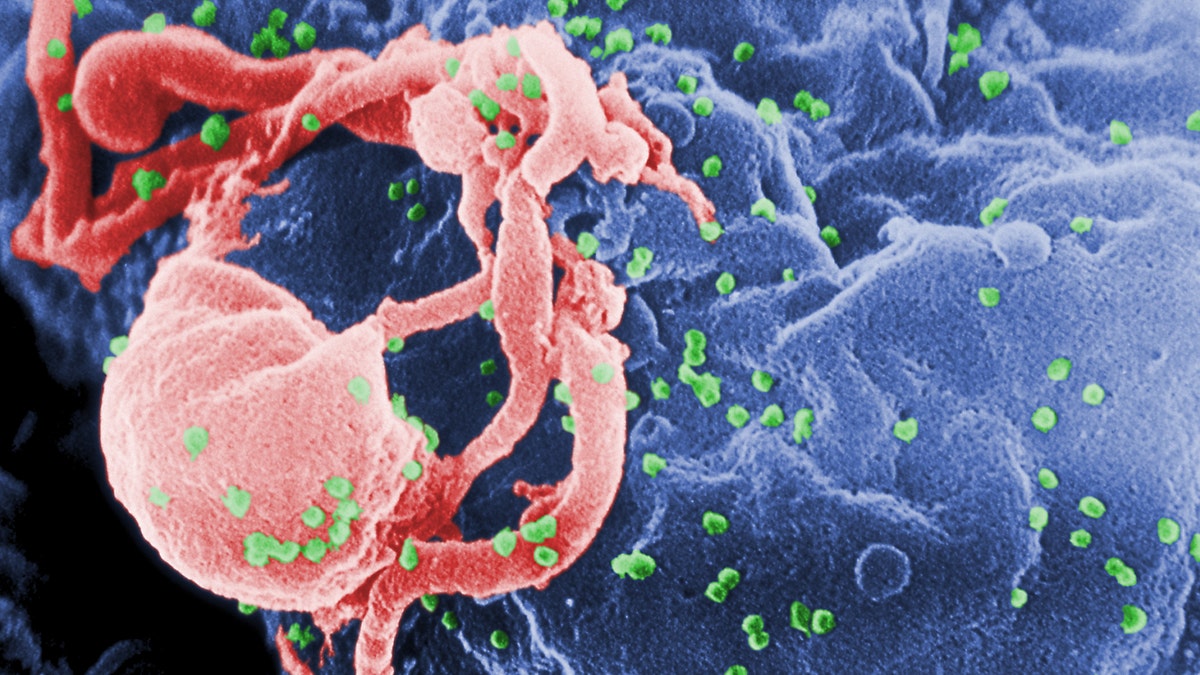
Scanning electron micrograph of HIV-1 budding from cultured lymphocyte. The multiple round bumps on cell surface represent sites of assembly and budding of virions. (CDC.gov)
Over the past decade, scientists have made incredible strides in the field of HIV research – leading to the development of numerous medications that can effectively manage the disease and provide patients with a near normal life expectancy.
But a cure for the human immunodeficiency virus has still eluded scientists, and now a new report from Howard Hughes Medical Institute (HHMI) has revealed that completely eradicating the virus may be much more difficult than previously thought.
In a new study published in the journal Cell, researchers have discovered that the reservoir of latent or inactive HIV that silently lingers in a patient’s body is much larger than scientists believed. In fact, this pool of viruses – known as HIV proviruses – may actually be 60-fold greater than previous estimates.
According to researchers, these findings are a major setback in the fight to cure HIV.
“We’re working very hard on developing better ways to assess the size of this reservoir,” lead author Dr. Robert Siliciano, an HHMI investigator at Johns Hopkins University, told FoxNews.com. “But I think there’s a lot more we really need to understand before we do a lot more clinical trials on (HIV cures).”
In order to effectively cure someone of HIV, the entirety of the virus must be eliminated from the body. This has been difficult to accomplish, since HIV exists in two states – an active version that is constantly replicating and destroying the immune system and an inactive version that hides in the body’s memory T cells and remains dormant.
When memory T cells respond to the virus and try to eradicate it from the body, they inadvertently become hosts for HIV. The virus “infects” some of the responding T cells by physically inserting itself into the cells’ DNA. Then, when the T cells go back to a resting state, the HIV is “turned off” and silently hides in its host cell.
Current antiretroviral medications for the treatment of HIV work by targeting the actively replicating form of HIV – but not this inactive form.
“In resting state…the virus is not actively replicating, so the drugs don’t affect it, and the immune system can’t see it, because no viral proteins are being made,” Siliciano explained. “That’s why you can’t cure the infection, because as soon as the patient stops treatment, some of these memory T cells get activated every day, and they start to replicate, and the virus takes off again.”
Finding the true size of HIV
Previously, researchers would estimate the amount of these latent proviruses by removing T cells from an HIV positive patient and activating them in test tubes. This approach was thought to force all of the functioning inactive proviruses hiding in the T cells to “turn back on.” Using this technique, approximately one HIV provirus was reactivated out of every million T cells.
But Siliciano and his colleague Ya-Chi Ho, an HHMI international student research fellow in Siliciano’s lab, believed this method did not provide the whole picture, since some of the proviruses remained inactive or latent in the T cells even in response to activation.
So the researchers developed a technique to further analyze the composition of the viral reservoir. In order to do this, they first activated the T cells but then focused on the non-induced proviruses. Using a genetic technique called polymerase chain reaction (PCR), the researchers were able to study the genomes of the proviruses that had failed to turn on, which remained in 300 out of ever million T cells.
While 88 percent of the non-induced proviruses contained some obvious mutation or defect in their DNA preventing them from replicating, approximately 12 percent had fully intact genomes, meaning they were entirely capable of being reactivated. And after a second and third attempt at stimulating the T cells, Siliciano and Ho found that these proviruses did, in fact, become active.
"If you take the T cells that did not produce virus, and simply reactivate them a second time, some start to produce virus,” Siliciano said. “…So the total number of cells you have to worry about is any cell that could turn on the virus…Maybe there’s some random process governing this, but those are the things that are not understood.”
These findings mean that scientists have many more proviruses to kill in order to fully cure an individual of HIV. However, Siliciano hopes his research will dissuade patients from entering into clinical trials testing a “shock and kill” approach to curing the virus, which involves activating many of the body’s T cells to force the proviruses to activate. Since the size of the provirus reservoir is so large, Siliciano said this technique could lead to major damage in the body.
“The current approach to curing patients is to try and turn on all of the latent virus and then get the cells to die,” Siliciano said. “You can’t do that in a patient because it would cause too many side effects. Having all your T cells turn on at the same time would lead to major toxicity.”
The HHMI study was released just as recent tests have found that a baby born with HIV in Mississippi is still in remission 18 months after being aggressively treated, potentially indicating that the child is cured. While Siliciano said this is great news and extremely important for HIV research, there is still much more to learn about the virus before a true cure can be developed.
“In the (Mississippi child’s) case, there are no memory T cells at the time of birth, and that’s why the infection is curable if you treat on the first day of life,” Siliciano said. “So for the vast majority of patients to cure them, we’ll have to deal with this reservoir. These cases of cures are exciting and have given people the feeling that ‘Yes, maybe this is something we can do.’ But it’s going to be a long and difficult struggle.”
https://www.foxnews.com/health/major-setback-for-aids-cure-study-finds-reservoir-of-hidden-hiv-bigger-than-once-thought